Strabismus (Crossed Eyes)
Strabismus (crossed eyes) is a condition in which one eye is turned in a direction that is different from the opposite eye.
Table of Contents
What is strabismus (crossed eyes)?
- Strabismus (crossed eyes) is a disease in which the eyes do not line up with each other.
- In other words, one eye is turned in a direction that is different from the opposite eye.
- Under normal conditions, the 6 muscles that control eye movement work combine and point both eyes in the same direction.
- Patients with strabismus have problems with the control of eye movement and may not keep normal ocular alignment (eye
- position).
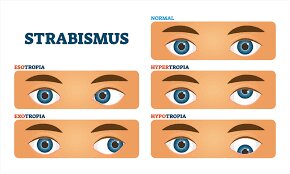
Strabismus may be classified by the direction of the turned or misaligned eye:
- Inward turning (esotropia)
- Outward turning (exotropia)
- Upward turning (hypertropia)
- Downward turning (hypotropia)
Other components to consider that help to identify the cause and treatment of strabismus:
- Did the problem come on immediately or over time?
- Was it available in the initial six months of life, or did it happens later on?
- Does it normally affect the same eye, or does it switch between eyes?
- Is the degree of turning little, moderate, or large?
- Is it generally present, or only part of the time?
- Is there a family history of strabismus?
Eye Muscles Anatomy
The ocular movement takes place around the 3 axes:
- Adduction (medial pupil movement toward the nose)/ Abduction (lateral pupil movement) around the vertical axis.
- Elevation (superior movement)/ Depression (inferior movement) near the transverse axis.
- Intorsion/ Extorsion (the move away and toward the nose) that we require at the time of tilting the head around the anteroposterior axis
- The 7 muscles of extraocular muscles are divided into four recti, two oblique muscles, and 1 levator palpebrae superior which are responsible for the elevation of the superior eyelid.

| Muscle | Origin | Insertion | Nerve supply | Action |
| Superior rectus | Common tendinous ring | superior and anterior aspect of sclera | oculomotor nerve (cranial nerve III) | elevation and contributes to adduction and intorsion |
| Inferior rectus | inferior and anterior aspect of sclera | oculomotor nerve (cranial nerve III) | depression and contributes to adduction and extorsion | |
| Medial rectus | medial aspect of the sclera | oculomotor nerve (cranial nerve III) | adducts eye | |
| Lateral rectus | lateral aspect of the sclera | abducens nerve (cranial nerve VI) | abducts eye | |
| Superior oblique | body of the sphenoid bone | at sclera posterior to superior rectus | Trochlear nerve cranial nerve IV) | abduction, depression, and intorsion of the eye |
| Inferior oblique | the anterior aspect of the orbital floor | at sclera posterior to lateral rectus. | oculomotor nerve (cranial nerve III) | abduction, elevation, and extortion of eye |
| Levator palpebrae superiors | sphenoid bone | superior eyelid | oculomotor nerve (cranial nerve III) | elevation of the superior eyelid. |
What are the types of strabismus?
There are several types of strabismus. The two most common are:
Accommodative esotropia:
- This frequently happens in cases of not treated farsightedness and a genetic predisposition (family history)
- for the eyes to turn in. Because the capability to focus is linked to where the eyes are pointing, the extra focusing effort required to keep distant objects in clear focus may cause the eyes to turn inward.
Symptoms of accommodative esotropia
- Double vision, closing or covering one eye when looking at something close, and tilting or turning the head.
- This form of strabismus generally begins in the first few years of life.
- This condition is usually treated with glasses, but can also require eye patching and/or surgery on the muscles of one or both eyes.
Intermittent exotropia:
- In this kind of strabismus, one eye will fixate (concentrate) on the target while the opposite eye is pointing
- outward.
Symptoms of Intermittent exotropia
- Double vision, headaches, difficulty in reading, eyestrain, and closing one eye when viewing far
- away things or when in bright light. Patients can have no symptoms while the ocular deviation (difference) can be noticed by others.
- Intermittent exotropia may take place at any age.
- Treatment can include glasses, patching, eye exercises, and/or surgery on the muscles of one or both eyes.
Infantile esotropia
- This condition is marked by a great amount of inward turning of both eyes in babies that generally begins prior to six months of age.
- There is normally no significant amount of farsightedness seen and glasses do not correct the crossing.
- Inward turning can begin start on an irregular basis but soon becomes regular in nature.
- It is seen when the baby is trying to look far away and up close.
- The treatment for this type of strabismus is surgery on the muscles of one or both eyes to correct the alignment.
- Adults may also experience strabismus.
- Most usually, ocular misalignment in adults is because of stroke. Still, it may also happen from physical trauma or from a childhood strabismus that was not previously treated or has recurred or progressed.
- Strabismus in a younger person may be treated in a variety of ways, involving observation, patching, prism glasses, and/or strabismus surgery.
How common is strabismus?
- It is estimated that 4% of the U.S. population, or about thirteen million individuals, have strabismus.
What causes strabismus?
- Most strabismus outcomes are from an irregularity of the neuromuscular control of eye movement.
- Our understanding of these control centers in the brain is still developed.
- List frequently, there is a problem with the actual eye muscle.
- Strabismus is frequently inherited, with about thirty percent of children with strabismus having a family member with an equal problem.
Other conditions connected with strabismus involve:
- Uncorrected refractive errors
- Poor vision in one eye
- Cerebral palsy
- Down syndrome (20-60% of these people are affected)
- Hydrocephalus (A congenital disease that outcomes in a buildup of fluid in the brain)
- Brain tumors
- Stroke (the leading cause of strabismus in young adults)
- Head injuries, which may damage the area of the brain responsible for the control of eye movement, the nerves that control eye
- movement, and the eye muscles
- Neurological (nervous system) problems
- Graves’ disease (overproduction of thyroid hormone)
When do the symptoms of strabismus appear?
- By the age of three to four months, the baby’s eyes should be able to focus on tiny objects and the eyes should be straight and well-aligned.
- A six-month-old child should be able to focus on something both near and far.
- Strabismus generally appears in infants and young children, and most frequently by the time a child is three years old.
- However, older children and even adults may develop strabismus.
- The onset appearance of strabismus, specifically with double vision, in an older baby or adult could indicate a more serious neurologic disorder. If this occurs, call the doctor as early as possible.
- A condition known as pseudostrabismus (false strabismus) may make it appear that a baby has crossed eyes when in fact the eyes are aiming in the equal direction.
- Pseudostrabismus can be caused by additional skin covering the inner corners of the eyes and/or a flat nasal bridge.
- As the baby’s face develops and grows, the eyes will no longer appear crossed.
How is strabismus diagnosed?
Anyone older than four months of age who appears to have strabismus should have a total eye examination by a pediatric ophthalmologist, with extra time, spent examining how the eyes focus and move. The exam may include the following:
- Patient history (to identify the symptoms the patient is having, family history, general health problems, medications being used
- and any other possible causes of symptoms)
- Visual acuity (reading letters from an eye chart, or examining a young baby’s visual behavior)
- Refraction (checking the eyes with a series of corrective lenses to estimate how they focus light).
- Children do not have to be old enough to give a verbal response when checking for glasses.
- Alignment and focus tests
- Examination after dilation (widening) of the pupils to identify the health of internal eye structures.
How is strabismus treated?
Treatment options involve below given:
Eyeglasses or contact lenses:
- Used in patients with uncorrected refractive errors.
- With corrective lenses, the eyes will require less focusing effort and can remain straight.
Prism lenses:
- Special lenses that may bend light entering the eye and help decrease the amount of turning the eye must do to see the
- objects.
Orthoptics (eye exercises):
- Can work on some types of strabismus, specifically convergence insufficiency (a form of exotropia).
Medications:
- Eye drops or ointments. Also, injections of botulinum toxin type A (such as Botox) may weaken an overactive eye muscle.
- These treatments can be used with, or in place of, surgery, based on the patient’s situation.
Patching:
- To treat amblyopia (lazy eye), if the person has it at the same time as strabismus.
- The improvement of vision can also improve control of eye misalignment.
Eye muscle surgery:
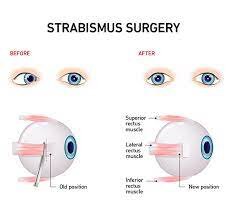
- Surgery changes the length or position of eye muscles so that the eyes are aligned perfectly.
- This is done under general anesthesia with dissolvable stitches.
- Sometimes people are offered adjustable strabismus surgery, where the eye muscle positions are adjusted after surgery.
What can happen if strabismus is not treated?
Some stated that babies will outgrow strabismus or that it will get better on its own. In truth, it can get inferior if it is not treated.
If the eyes are not perfectly aligned, the following may result:
- Lazy eye (amblyopia) or long-lasting poor vision in the turned eye.
- When the eyes are looking in different directions, the brain receives 2 pictures.
- To avoid double vision, the brain can avoid the image from the turned eye, resulting in poor vision development in that eye.
- Blurry vision, which may affect performance in school and at work, and enjoyment of hobbies and leisure activities
- Eye strain
- Fatigue
- Headaches
- Double vision
- Poor 3-dimensional (3-D) vision
- Low self-esteem (from embarrassment about someone’s appearance)
- It is also possible that by not identifying strabismus, a serious problem (like a brain tumor that is causing the condition) can be overlooked.
Physiotherapy management
Pencil pushups
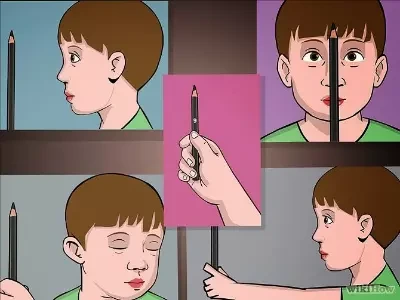
- Pencil pushups are simple ocular workouts that get both eyes aimed at the same fixed point.
- They are also identified as near points of convergence exercises.
- Start by grasping a pencil out at arm’s length, pointing away from the patient.
- Focus the glare on the eraser or a letter or numeral on the side.
- Gently move the pencil toward the tip of the nose.
- Keep it in focus for as long as a person can, but stop once the vision gets blurry.
Barrel cards

- This is a handy exercise for exotropia. Draw three barrels of progressive size in red lengthwise on 1 side of a card.
- Do the same thing in green on the other side.
- Grasp the card lengthwise and vertically opposed to the nose so that the largest barrel is furthest away.
- Glare at the far barrel until it becomes one image with both colors and the other two barrel images have doubled.
- Stabilize the gaze for about five seconds.
- Then do it again with the middle and smallest barrel images. Coloring within the lines
- Many babies love to color. Motivating the child to color in a coloring book is an excellent way to sneak in an eye exercise.
- The goal here is to have the child color within the lines, not just on the page.
- Prior to starting this exercise, make the child has sharpened coloring pencils or crayons without dull points.
- To perform this exercise: Select a coloring book with simple pictures that have strongly delineated lines.
- Put an eye patch over the child’s stronger eye.
- Suggest them to carefully color the objects on the page and stay within the lines.
- Be sure to supervise the child so that they do not remove the eye patch.
Brock string exercise
This exercise helps the eyes learn how to work combine to focus on an object. This exercise requires a Brock string or a homemade string. A Brock string is a white string that is approximately fifteen feet long. It has colorful wooden beads on it, which may be moved around. Do not use an eye patch when performing this exercise. Shop for a Brock string online.
To perform the Brock string exercise:

- Hitech a loop on both ends of the Brock string.
- Use one loop to attach the string to a door or other fixed object.
- Position the beads along the string so that one is close to the doorknob (far fixation), one is around three feet away from the person (middle fixation), and one is six inches from the nose (near fixation).
- Stand directly in front of the doorknob.
- Use the other string loop to put the Brock string around the finger.
- Hold the string flush along the upper lip, right under the nose.
- The cord should be stretched tight. If it is not tight, take a moment to adjust and shorten it by making the loops larger.
- Look at the bead closest to a person, and make sure a person sees one bead, not two.
- If a person sees two beads, move the bead until a person sees one.
- A person should see two strings as if one is coming from each eye.
- The strings should form an X shape.
- As a person moves the bead closer to the nose, the strings should meet exactly at the bead, and take on a V shape.
- Repeat by shifting the focus to the middle fixation bead and then the far fixation bead.
- As the weak eye becomes stronger, the bead should be able to be moved closer to the eyes, until it is only 1 inch away.
Video games
- Specially designed video games that are played while wearing goggles have shown a pledge for lazy eyes.
- These games are played dichoptically, meaning every eye views something various through the goggles, like high or low-contrast images.
- For adults, a dichoptic version of Tetris has been shown by scientists at the Health Centre to be effective for strengthening the weaker eye.
- Playing video games with an eye patch can also have a beneficial effect. Small research
- indicated that both action and non-action video games had benefits for adults with lazy eyes.
Dot card
For this exercise, a patient will work to maintain a single picture of a dot on a card with both eyes. To use a dot card:

- Draw dots on a paper card made out of cardboard or another type of stiff paper.
- Grasp the card lengthwise and touch the nose so that the line of dots is directly in front of the face.
- Tilt the card down slightly.
- Focus on the dot farthest away from a person. If the eyes are converging correctly, the pattern of dots should look like they are in an A shape. The dot a person is focusing on should be singular and not blurry.
- Focus on the next dot in the line, and then the next, holding each dot in focus for a count of five.
- If the eyes are continuing to converge correctly, an X shape will form.
- When a person reaches the dot that is closest to her, the dots in the back will double and form a V shape.
Barrel convergence cards

- This exercise is used initially to treat exotropia, a form of strabismus.
- A person may buy these cards or make them themselves.
- To make barrel convergence cards, draw 3 red barrels on one side of the card in a lengthwise pattern.
- The barrels should be larger in size toward the bottom of the card.
- Draw corresponding barrels on the opposite side of the card in green.
To use barrel convergence cards:
- Grasp the card lengthwise touching the nose so that the three barrels appear in a vertical line, pointing away from the face.
- The largest barrel should be farthest from the nose.
- Stare at the largest barrel until a person sees one image with both colors.
- The other 2 barrels should appear doubled.
- Hold the gaze for the count of five, then move on to each smaller barrel, repeating the exercise.
Puzzles
- Putting together jigsaw puzzles with an eye patch may help strengthen the weaker eye.
- There is a very biggest range of jigsaw puzzle types. Be sure to opt for age-appropriate puzzles that won’t frustrate the child with their complexity.
Reading
- If the child may read, have them read an age-appropriate book they enjoy for at least thirty minutes daily with a patch over their stronger eye.
FAQ
Most children with strabismus have been diagnosed between the ages of 1 and 4 years old. Rarely, a child might develop strabismus after age six. If this happens, it is necessary for the child to see a doctor right away to find out other conditions.
Most strabismus is the result of an abnormality of the poorly understood neuromuscular (including the brain) control of eye movement. Less usually, a problem with the actual eye muscle causes strabismus.
Atropine drops are medicated eye drops that work fundamentally as chemical ocular patching. The aim of atropine drops is to cause temporary blurred vision in the unaffected eye, thus muting the visual input from the eye to the brain, forcing the deviated eye to focus and therefore align.
Strabismus surgery may be done in children as young as four months of age and is a crucial option for older children and adults as well. It is better to perform surgery as early as possible because the brain circuits for binocular vision (using the two eyes together) are most adaptable at a young age.
Our team strategically places contoured prisms within the lenses of the glasses to tell the eyes where they need to focus. In turn, the weak muscles of the eyes strengthen over time, which corrects strabismus. In addition, prism-correction lenses may drastically improve the symptoms of CVS.


8 Comments