What is a Physical Therapy Evaluation?
A systematic physical therapy evaluation starts with a clinical examination that includes a patient history, system review, and objective data collection. The physical therapist then communicates their findings in an evaluation, which is followed by a prescribed plan of care (POC).
Remember that an evaluation cannot be completed unless the patient is thoroughly examined.
Table of Contents
Preliminary Evaluation Steps
Before sitting on your stool and interviewing your patient, go over their prescriptions, demographics, pain chart, past medical history, and current medications. With tools like digital patient intake forms, these can be collected ahead of time and transferred directly to the patient chart.
At this point, you should also consider administering a patient-related outcome measure (PROM). Technically, this can be done before, during, or after the evaluation—you’ll need to determine what works best for your workflows. However, if you are short on time or prefer to review scores ahead of time, tracking PROMs through an application designed to manage this data can provide valuable insight into your patient’s needs and ultimately improve outcomes.
Subjective Evaluation
The subjective examination is frequently overlooked, but it is likely the most important part of the evaluation. It starts the clinical reasoning process, from which you will develop your diagnosis and point of contact. Medical history provides sufficient information in about 75% of patient encounters to make the diagnosis without performing a physical examination and additional tests.
It takes practice to know where, when, and how to start interviewing your patient. Therapists can gather this data reliably and effectively by adopting a funnel-down method and open-ended guided inquiries as a starting point. Among the topics to be covered during the subjective examination are, but are not limited to:
- The most common patient complaints;
- the previous level of function;
- the mechanism of injury (MOI);
- Employment and work history;
- and a medical and surgical history
- SINSS is an acronym for severity, irritability, nature, stage, and stability of the patient.
Gathering information using the SINSS model will provide you with a clear picture of why the patient has come to you and where you can start working towards their recovery.
History
When you arrive at the clinic for your appointment, you may be asked to fill out some paperwork, such as your medical history and a general health questionnaire. Some clinics allow you to fill them out online ahead of time, which may be a great way to save time. If you have a referral from your doctor, the clinic may already have it, but bring a copy just in case.
Your therapist will go over any paperwork you have submitted before meeting with you. When your therapist enters the room, they will ask you questions about your medical history, current problem, and how it affects your daily life.
Then you can talk about your goals and what you want to achieve during and after therapy.
Before your first physical therapy appointment, make a list of the key facts about your problem’s history. You are less likely to forget or overlook important information if you write it down. Try to answer the following questions:
- When and how did your issue start?
- What was your level of functional mobility before your injury?
- How frequently do the symptoms reoccur?
- How is the situation changing?
- What causes things to improve or deteriorate?
Our physical therapist will most likely ask you some questions about your injury or illness. Bring a list of your medications as well as any previous surgeries or procedures.
Patient Examination Objective Measures
With all of the subjective examination data collected, you can now apply all of the skills you learned in PT school to gather the relevant data about your patient’s primary complaint, as well as any related deficits that will need to be addressed in the future. These elements are as follows:
- Screening of neighbouring joints and systems;
- Collection of active and passive range of motion;
- Muscle length measurement;
- Muscle testing by hand;
- Neurodynamic evaluation;
- Palpation and testing for joint accessory motion;
- Special tests;
- Analysis of gait;
Anything else that can be measured.
The special tests, as you can see, are completed near the end of the objective data collection. This is done on purpose to remind PTs that special tests are used to confirm or rule out a diagnosis based on other data. Reliance on special tests for clinical decision-making has been a pitfall for many therapists in the past, so trust in your clinical reasoning skills before depending too heavily on some eponymously named special tests.
Physical Examination
Following the initial evaluation, your physical therapist will conduct a physical assessment to determine the impairment causing your problem. The assessment includes some points:
- Palpation
- Range of motion (ROM)
- Functional mobility
- Strength assessment
- Balance
- Posture
- Coordination
- Skin integrity
- Muscle function
Your physical therapist should be guiding you and giving you clear instructions on what to do during the physical examination.
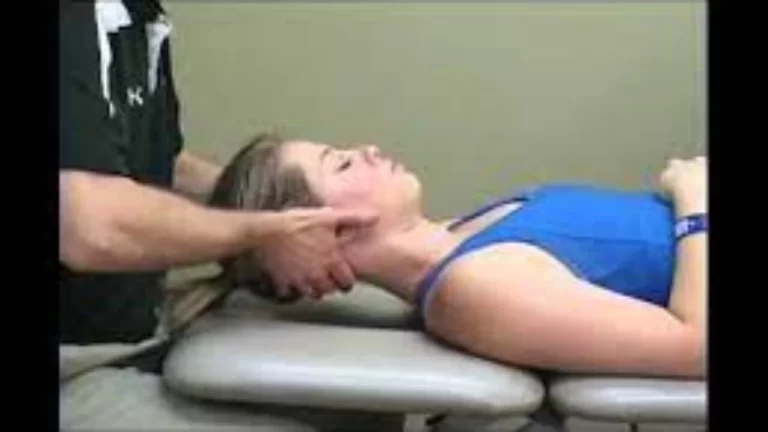
They may place their hands on the area of your body where you are experiencing symptoms to determine what types of movements or pressure cause pain. They will ask you to rate the level of pain in various scenarios.
A physical therapist may also conduct assessments for a specific purpose. A functional capacity evaluation in physical therapy, for example, helps determine whether an individual can work after an injury or qualifies for disability benefits. The tests performed during an initial evaluation differ depending on the needs of the patient.
Physical Therapy Diagnosis
Your PT will assist in determining a diagnosis and then, as a member of your healthcare team, will collaborate with your doctor.
You can set goals with your PT for your physical therapy appointments. Many physical therapists will focus on helping you regain your quality of life. You should concentrate on:
- Pain relief
- Returning to mobility
- maintaining daily activities
Your PT will assist you in understanding what is happening with your condition and how it will interact with your treatment plan. You should understand what you need to do to achieve your objectives with their assistance.
Physical therapy treatment
Your therapist will go over the results of your evaluation near the end of your time together. They will go over a treatment plan with you and suggest some exercises that you can do at home. Their initial plan will most likely change as you progress; mobility is an important part of any good treatment plan as your condition improves.
The evaluation concludes with a discussion and planning of future sessions where your treatment plan will be carried out. However, your evaluation does not end with this first session; your therapist will continue to assess you to ensure that you are progressing as planned.
Which therapies could be included in the plan of care?
After the test is over and you have a plan for recovery in place, it’s time to get to work. Your therapist has the option to use a variety of activities during your session.
Therapeutic Techniques
Therapeutic modalities include a variety of techniques that can assist you in achieving comfort, strength, and mobility. Your physical therapist may need to improve blood flow, provide flexibility, reduce swelling, promote relaxation, or manage your pain.
- Heat
- Ice
- Water
- Laser
- Electrical stimulation
- Dry needling
- Ultrasound
Make sure you understand how your PT can assist you with these therapies by having a conversation with them. Ask about what you want for the results and how you will feel.
Mobilisation and massage
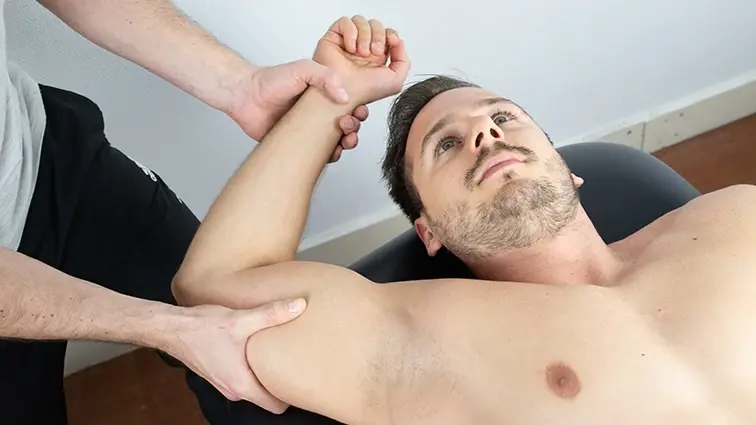
Your treatment plan may include hands-on joint and soft tissue massage and mobilisation. The therapist should knead and rub the soft tissue to relieve discomfort and stimulate blood flow. The therapist can shift your joints and muscles through various stretches to increase your range of motion and flexibility.
Exercise
The recovery plan will be built around exercise. Your PT will lead you through specific stretches and activities that will help you move better and feel stronger. You could use modern machines such as bikes and treadmills, or more basic workout equipment. Your PT will supervise all of your activities during your session. In physical therapy, you can also work with an assistant.
You will be provided a collection of exercises to do at home These at-home exercises are used to help you recover faster. You may not see your PT regularly, but you will notice improvements as you complete the at-home exercises. Your PT will discuss how much time you can devote to at-home workouts with you.
Summary
A systematic physical therapy evaluation involves a clinical examination, patient history, system review, and objective data collection. The evaluation is crucial for determining the patient’s condition and developing a prescribed plan of care (POC).
Preliminary evaluation steps include reviewing prescriptions, demographics, pain charts, past medical history, and current medications. Digital patient intake forms can be used to collect information ahead of time and transferred directly to the patient chart. Patient-related outcome measures (PROM) can provide valuable insight into the patient’s needs and improve outcomes.
The subjective examination is essential for developing a diagnosis and point of contact. It covers topics such as common complaints, previous level of function, mechanism of injury, employment and work history, and medical and surgical history. The SINSS model helps determine the patient’s severity, irritability, nature, stage, and stability.
At the clinic, patients may be asked to fill out paperwork, such as medical history and a general health questionnaire. The therapist will ask questions about the patient’s problem, goals, and symptoms. A list of key facts about the problem’s history is also helpful.
Objective measures collected from the subjective examination include a screening of neighbouring joints and systems, collecting active and passive range of motion, muscle length measurement, muscle testing by hand, neurodynamic evaluation, palpation and testing for joint accessory motion, additional outcome indicators, special tests, gait analysis, and more.
The physical therapist conducts a physical assessment to determine the impairment causing the problem, including palpitation, range of motion (ROM), functional mobility, and strength assessment. Balancing the patient’s pain levels and focusing on pain relief, returning to mobility, and maintaining daily activities are important goals.
Treatment plans are discussed and planned for future sessions, with the therapist continuing to assess the patient’s progress. Therapeutic techniques may include heat, ice, and other techniques to help achieve comfort, strength, and mobility.
FAQs
What exactly is an initial evaluation?
Your first visit to our clinic as a patient is considered an initial evaluation. An initial evaluation does not include a free consultation. The initial evaluation is an additional visit with your physical therapist to determine the best course of treatment for your condition. This frequently includes a discussion about your condition, health history, and goals. Stretching and exercises are frequently included in these visits. Following your initial evaluation, you will work with us to schedule your next appointment so that you can get back to doing what you like.
What is the significance of evaluation in physical therapy?
After an injury, surgery, or sickness, a physical therapy assessment is a crucial first step toward recovery and regaining function and mobility.
What exactly do physical therapists do?
Physical therapists are movement specialists who help patients improve their quality of life through exercise, hands-on care, and education. Following a diagnosis, physical therapists develop personalised care plans to improve mobility, manage pain and chronic conditions, recover from an injury, and prevent future injuries and chronic conditions.
Can physical therapy help me avoid surgery?
For certain conditions, physical therapy is just as effective as surgery. Before undergoing costly and invasive surgeries, consider physical therapy.
Why need I to perform exercises?
The main objective of physical therapists is for patients to be able to maintain their independence. To do so, they will push you slightly beyond your comfort zone. In order to restore your independence, physical therapists will push you to go beyond your current limits. The majority of people only go to therapy a few times per week. Stretching and strengthening exercises must be performed almost daily to achieve the desired results. And, yes, physical therapists can tell whether or not someone is doing their home exercises.
References:
- Physical Therapy Evaluation Example. (2023, September 29). WebPT. https://www.webpt.com/blog/physical-therapy-evaluation-example
- Brandt, C. (n.d.). What Is A Physical Therapy Evaluation? https://www.ewmotiontherapy.com/blog/physical-therapy-evaluation
- Devarapalli, V. (2020, November 4). What Is Involved In A Physical Therapy Evaluation? https://paceptclinic.com/patient-information/what-is-involved-in-a-physical-therapy-evaluation/
- Physical Therapy Appointment: What happens during the first PT Evaluation? (2019, March 15). Raleigh Orthopaedic. https://www.raleighortho.com/blog/sports-medicine/physical-therapy-appointment-what-happens-during-the-first-pt-evaluation/
- F. (2023, August 22). What To Expect at a Physical Therapy Evaluation. EmergeOrtho. https://emergeortho.com/news/physical-therapy-assessment/



![Test for tight retinacular [ collateral ] ligaments](https://samarpanphysioclinic.com/wp-content/uploads/2023/06/Test-for-tight-retinacular-_-collateral-_-ligaments.webp)