Low Blood Sugar (Hypoglycemia)
- Hypoglycemia (low blood sugar) is usual in people who have diabetes. Yet it can also sometimes affect people without diabetes. You require to treat hypoglycemia as soon as possible by consuming carbohydrates. If it is left untreated, severely low blood sugar can be life-threatening.
Table of Contents
What is hypoglycemia (low blood sugar)?
- Hypoglycemia happens when the level of sugar (glucose) in your blood drops under the range that is healthy for you. It is called low blood sugar or low blood glucose. Hypoglycemia is usual in people with diabetes, especially Type 1 diabetes.
- For most people with diabetes, hypoglycemia is when your blood sugar level is under 70 milligrams per deciliter (mg/dL) or 3.9 millimoles per liter (mmol/L).
- For most people without diabetes, hypoglycemia is when their blood sugar level is under 55 mg/dL or 3.1 mmol/L.
- Hypoglycemia requires instant treatment by eating or drinking sugar or carbohydrates. Serious hypoglycemia can be life-threatening and requires treatment with emergency glucagon and/or medical intervention.
What is blood sugar?
- Glucose (sugar) mostly comes from carbohydrates in the food and drinks you consume. It is your body’s main source of energy. Your blood carries glucose to all of your body’s cells to utilize for energy. Glucose is very important because it is the primary source of energy for your brain.
- If you do not have diabetes, several bodily processes naturally help keep your blood glucose in a healthy range. Insulin, a hormone your pancreas creates, is the most significant contributor to maintaining healthy blood sugar. Glucagon is another main hormone in this process.
- People who have diabetes must use medication, such as oral diabetes medications or synthetic insulin, and/or lifestyle changes to help keep their blood sugar levels in range.
- Low blood sugar often occurs due to excess insulin — whether your body naturally makes too much or you inject too much synthetic insulin. Other hormonal and metabolic issues can also conduct to low blood sugar.
- If your blood sugar drops below the healthy range, it causes certain symptoms such as shakiness and a faster heartbeat and can be life-threatening if it goes too low. This is because your brain requires a continuous supply of glucose to function properly. Without enough glucose, your brain can not function.
How common is hypoglycemia?
- Hypoglycemia is usual in people with diabetes, especially people who take insulin to manage the condition.
- One study found that 4 in 5 people with Type 1 diabetes and close to half of all people with Type 2 diabetes who take insulin reported a decrease in blood sugar episodes more than once over a four-week period.
- People with Type 2 diabetes who take meglitinide or sulfonylurea oral diabetes medications are also at an increased risk for decreased blood sugar.
- You can experience hypoglycemia without having diabetes, but it is uncommon.
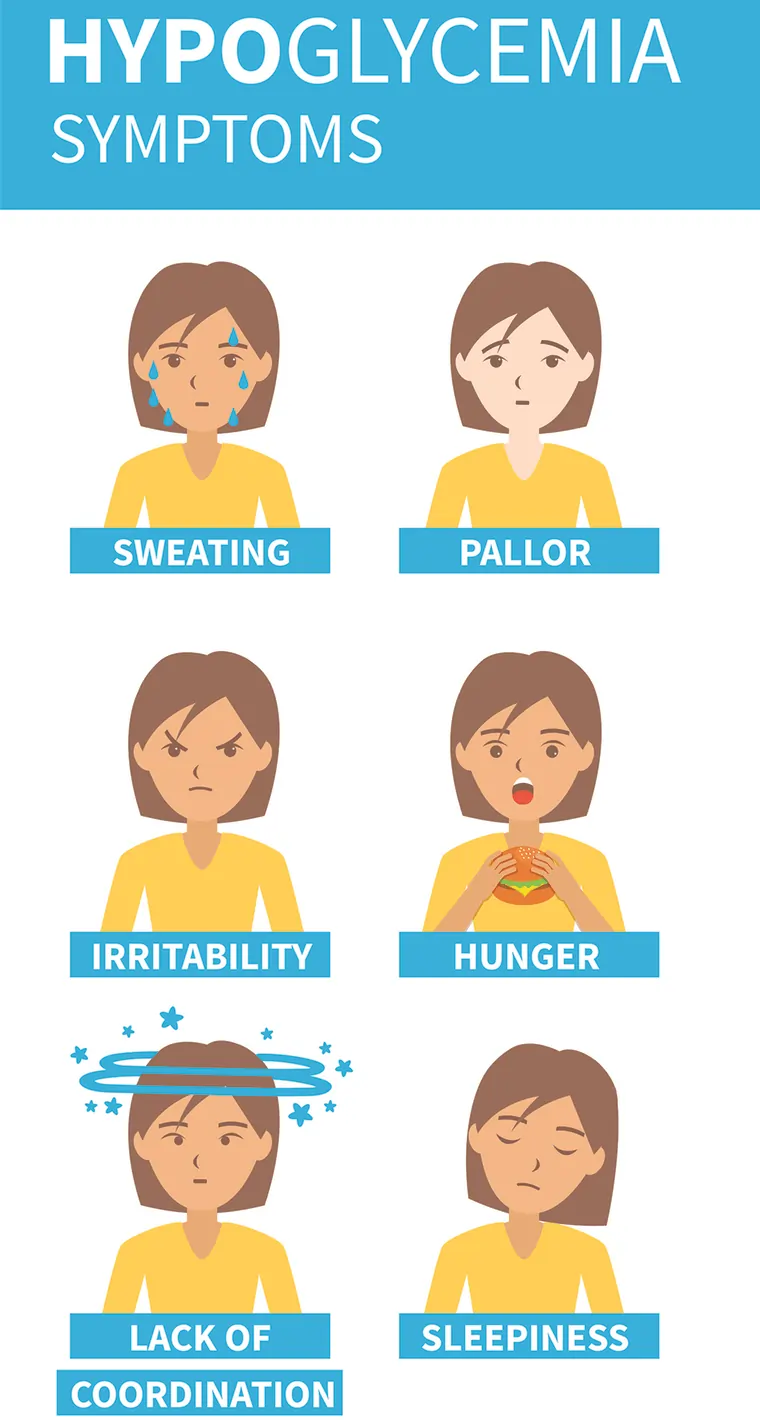
What are the signs and symptoms of hypoglycemia (decrease blood sugar)?
- Symptoms of hypoglycemia can begin quickly, and they can vary from person to person. One person can also experience various symptoms for each episode.
- The signs of hypoglycemia are troublesome. Yet they provide good warnings that you should get action before your blood sugar drops more.
The signs involve:
- Shaking or trembling,
- Weakness,
- Sweating and chills,
- Extreme hunger (polyphagia),
- Faster heart rate,
- Dizziness or lightheadedness,
- Confusion or trouble concentrating,
- Anxiety or irritability,
- Color draining from your skin (pallor),
- Tingling/numbness in your lips, tongue, or cheeks.
Signs of severe hypoglycemia involve:
- Blurred or double vision
- Slurred speech
- Clumsiness or difficulty with coordination
- Being disoriented
- Seizures
- Loss of consciousness.
- Serious hypoglycemia is life-threatening. It requires immediate medical treatment. In rare cases, severe hypoglycemia that is not treated can result in a coma and/or death.
- You can also experience decrease blood sugar while sleeping (nocturnal hypoglycemia).
Symptoms may involve:
- Restless sleep
- Sweating through your pajamas or sheets
- Crying out during sleep
- Having nightmares
- Feeling tired, disoriented, and confused after waking up.
When do hypoglycemia symptoms appear?
- The glucose level at which symptoms begin differs from person to person for people who have diabetes.
- In general, symptoms sometimes start for people with diabetes when their blood glucose is around 70 mg/dL or lower. If your blood sugar is falling rapidly, you may experience symptoms previous to this point.
- Some people with diabetes can have symptoms of hypoglycemia at relatively greater glucose levels. This is because, when you have chronic hyperglycemia (high blood sugar), your body gets utilized to that as its “normal” level. It alters the set point at which decrease blood sugar symptoms become apparent.
- Some people who have low blood sugar episodes do not have symptoms or do not notice them. Healthcare providers (doctors) call this hypoglycemia unawareness. People with hypoglycemia unawareness are more likely to have severe episodes and need medical assistance.
- Hypoglycemia unknowing can occur in people with diabetes who live with chronically low blood sugar (hypoglycemia) levels. Their body stops having symptoms when low blood sugar happens.
- If you have hypoglycemia unawareness, it is important to let your friends and family know so that they know how to help you if you experience a severe low blood sugar episode.
You may benefit from the following:
- Using a continuous glucose monitoring (CGM) device can aware you when you have hypoglycemia.
- More constant manual blood sugar checks.
- A service dog known as a diabetes alert dog is specially trained to alert you when you have low blood sugar.
What are the complications of low blood sugar?
Prolonged severe hypoglycemia is life-threatening and can conduct to the following complications:
- Multiple organ failure
- Cardiac arrhythmias
- Cardiac arrest
- Permanent brain damage
- Coma
- Death.
- Operating heavy equipment, such as driving a vehicle, while having decreased blood sugar can also be dangerous. You may be more likely to acquire in an accident. If you have diabetes, always create sure your blood sugar is in range before operating heavy equipment.
What causes hypoglycemia (decrease blood sugar) in people with diabetes?
- Hypoglycemia happens when your blood sugar drops under a healthy range. So many factors can contribute to this for people with diabetes. Hypoglycemia can develop if things such as food, exercise, and diabetes medications are out of balance.
Common situations that can lead to hypoglycemia for people with diabetes involve:
- Taking too much insulin, the wrong insulin, or injecting it into your muscle rather than in your fat tissue.
- Not timing insulin & grump input correctly (for example, waiting to extend to eat a meal & later taking care of insulin for the meal).
- Taking too much or too great of a dose of oral diabetes medications.
- Being more active than common.
- Drinking alcohol without eating.
- Eating meals after than usual or skipping meals.
- Not balancing meals by involving fat, protein, and fiber.
- People who are pregnant and have Type 1 diabetes are also more likely to experience low blood sugar during the 1st trimester due to hormone changes.
What causes hypoglycemia in people without diabetes?
- There are 2 main types of non-diabetes-related hypoglycemia: reactive hypoglycemia and fasting hypoglycemia.
Reactive hypoglycemia
- Reactive hypoglycemia happens when you experience low blood sugar later after a meal. It typically occurs about two to four hours later a meal.
- Researchers do not yet know the exact cause. But they think it occurs due to a sudden spike and then a fall in blood sugar after eating certain foods, especially simple carbohydrate foods such as white rice, potatoes, white bread, cake, and pastries.
- Bariatric surgery can also outcome in reactive hypoglycemia. Later certain types of bariatric surgery, such as gastric bypass surgery, your body absorbs sugars very quickly, which stimulates excess insulin production. This can then be because of hypoglycemia.
- Your body usually corrects reactive hypoglycemia on its own, yet consuming carbohydrates may help your symptoms go away more quickly.
Fasting hypoglycemia
- For the majority of people without diabetes, not eating food for a long time (fasting) does not lead to hypoglycemia. This is because your body utilizes hormones and stored glucose to manage your blood sugar.
However, certain conditions and situations can lead to fasting hypoglycemia in people without diabetes, involving:
- Excessive alcohol consumption: Alcohol cures your body from forming new glucose cells (gluconeogenesis). If you drink excessive amounts of alcohol over several days and do not eat much, your body can run out of stored glucose (glycogen). This can lead to hypoglycemia because your body can not properly regulate your blood sugar.
- Critical illness: You can experience hypoglycemia in serious illness states, such as end-stage liver disease, sepsis, starvation, or kidney failure. This is because your body is utilizing stored glucose for energy faster than your body can create new glucose cells from the food you eat.
- Adrenal insufficiency: Adrenal insufficiency causes decreased-than-normal cortisol levels. As cortisol (a hormone) assists regulate your blood sugar by increasing it, having low levels of cortisol can conduct in hypoglycemia episodes.
- Non-islet cell tumor hypoglycemia (NICTH): This is a rare yet serious syndrome in which a tumor releases excess insulin such as growth factor 2 (IGF-2). This is a hormone that has the same effects as insulin. Excess IGF-2 causes hypoglycemia. A broad variety of benign (noncancerous) and malignant (cancerous) tumors can cause NICTH.
- Insulinoma: An insulinoma is an infrequent tumor in your pancreas that produces excess insulin. It conducts to hypoglycemia episodes — most commonly in the early morning.
- In rare cases, non-diabetes-related medications can conduct to hypoglycemia, such as beta-blockers and certain antibiotics.
- If you are experiencing hypoglycemia and do not have diabetes, talk to your healthcare provider.
How is hypoglycemia diagnosed in people with diabetes?
- The only way to know if you have hypoglycemia is to detect your blood sugar with a blood glucose meter (glucometer). Most of these devices utilize a tiny blood sample from a finger prick with a lancet (small needle).
- A CGM could be an assist tool in identifying and preventing low blood sugar because you can program it to alert you to low blood sugar. CGM alerts can be especially utilized during times when it could be dangerous to have a lump of low blood sugar, such as while you are sleeping or driving.
- If you are experiencing symptoms of hypoglycemia (low blood sugar) and are unable to check your blood sugar, treat the hypoglycemia.
How is hypoglycemia diagnosed in people without diabetes?
- If your healthcare provider suspects you have hypoglycemia, they may check your blood sugar every certain hour during fasting lasting several days. You will need additional tests to determine the underlying cause of the hypoglycemia, such as imaging tests to see if a tumor is causing the low blood sugar episodes.
- For reactive hypoglycemia, your provider might recommend a test known as a mixed-meal tolerance test (MMTT). For the mixed-meal tolerance test (MMTT), you first have a special drink containing protein, fats, and sugar. The drink raises your blood glucose, causing your body to create more insulin. Then a provider will check your blood glucose multiple times over the next 5 hours.
How is hypoglycemia (low blood sugar) treated?
- You treat mild to moderate hypoglycemia by eating/drinking sugar (carbohydrates).
The American Diabetes Association recommends the “15 to 15 rule” to treat an episode of mild to moderate hypoglycemia:
- Eat or drink 15 grams of fast-acting carbs to increase your blood sugar.
- Later 15 minutes, check your blood sugar.
- If it is motionless below 70 mg/dL, have another 15 grams of fast-acting carbs.
- Repeat up to your blood sugar of at least 70 mg/dL.
- To realize how many carbs you are eating, read food nutrition labels.
Certain examples of foods that contain about 15 grams of fast-acting carbs involve:
- One small piece of fruit, such as half a banana,
- Four ounces (half-cup) of juice or regular soda (not diet),
- One tablespoon of sugar, honey, or syrup,
- One tube of instant glucose gel (check the instructions),
- Three to 4 glucose tablets (check the instructions),
- If you have symptoms of hypoglycemia but can not check your blood sugar, use the 15-15 rule until you feel better.
- Children may require fewer grams of carbs to treat hypoglycemia. Check with your child’s healthcare provider (doctor).
Physiotherapy Treatment
- When treating diabetic patients monitor whilst exercising. The therapist should watch the patient for symptoms of hypoglycemia and look above. A 30-minute exercise regular every day can work wonders for sugar control.
How is severe hypoglycemia treated?
- Severe hypoglycemia requires various treatments than mild or moderate hypoglycemia. If someone you know is having a hypoglycemia episode and is mucking their speech, disoriented or unconscious, do not give them food or liquid. They could block.
- Severe hypoglycemia episodes require the utilization of emergency glucagon. This is a synthetic form of glucagon that you can manage as an injection or nasal powder (dry nasal spray), turning on the type. Synthetic glucagon triggers your liver to release stored glucose, which then improves blood sugar.
- If the glucagon is injectable, inject it into their butt, arm, or thigh, following the commands in the kit. If the glucagon is a nasal powder, follow the commands on the package to administer it into their nostril.
- When the person obtains awareness (usually in 5 to 15 minutes), they may accomplish nausea. If they are laying down, roll them onto their side to cure choking in case they vomit.
How can I prevent low blood sugar?
- Unfortunately, it can be hard to totally prevent low blood sugar when you have diabetes. Yet you can adjust your diabetes management plan to try to decrease the number of hypoglycemia episodes you experience.
- It is easiest to do this when you and your healthcare provider (doctor) understand what causes your blood sugar to drop. Give your healthcare provider (doctor) as much information as possible about any decreased blood sugar episodes. Fixing the problem may be as easy as changing the times you take care of medication, eat and exercise.
The following steps can assist prevent low blood sugar:
- Take care of all your medications exactly as prescribed.
- Follow your healthcare provider’s (doctor) instructions about food and exercise.
- Utilize a continuous glucose monitor (CGM) or check your blood sugar regularly, including before and after meals, before and after exercise, and before bed.
- After you have treated a low blood sugar (hypoglycemia) episode, write down the description of the episode. Involve details such as the time, what you ate recently, whether you exercised, the symptoms, and your glucose level. This can assist you and your provider (doctor) adjust your management plan to try and prevent future lows.
What can I expect if I have hypoglycemia (low blood sugar) episodes?
- The prognosis (outlook) of non-diabetes-related hypoglycemia varies turning on the underlying cause.
- Having recurrent hypoglycemia (low blood sugar) episodes can be dangerous if you have diabetes. It can lead to hypoglycemia unawareness, which means you do not experience warning signs of low blood sugar. It is important to see a healthcare provider who helps you manage diabetes if you are having frequent lows.
How can I take care of myself?
- If you have diabetes or another condition that causes hypoglycemia, attrition a medical warning necklace or bracelet or carry a medical ID. That way, people know how to assist you in case of an emergency.
Steps you can take to prevent severe hypoglycemia involve:
- Always have snacks available in your home and on you when you are away from home, such as fruit snacks, glucose tabs, or juice boxes.
- Educate people you spend time with about hypoglycemia and severe hypoglycemia, and how they can assist you if you experience an episode.
- Always have extreme glucagon on hand. Educate your loved ones on how and when to utilize it.
- If you have diabetes, try not to over-treat and decrease blood sugar by eating an excess amount of carbs. This can conduct to rebound in high blood sugar. It can be hard to not overeat due to your body’s “fight or flight” response. Once you have initially treated the low with 15 grams of carbs, set a timer for 15 minutes before consuming more sugar.
When should I look to my healthcare provider about hypoglycemia?
- If you have diabetes and are experiencing frequent low blood sugar (hypoglycemia) episodes, talk to a provider (doctor) who assists you manage diabetes. They can help you adjust your management plan, which may involve changes to your medication regimen, meal plans, or exercise routine.
- If you do not have diabetes and are experiencing low blood sugar (hypoglycemia), talk to your healthcare provider. They will require to order tests to affect the underlying cause. In certain cases, the underlying condition can be serious. Because of this, it is important to look at your provider.
What’s the difference between hypoglycemia and hyperglycemia?
- Hypoglycemia is a decrease in blood sugar. “Hypo-” means “below.” Hyperglycemia is an increase in blood sugar. “Hyper-” means “above” or “beyond.”
NOTE
- Hypoglycemia is quite usual in people with diabetes. If it has not resulted in time, it can be life-threatening. It is mainly to know your individual warning signs for low blood sugar (hypoglycemia) & to detect your blood sugar regularly to struggle to prevent severe low blood sugar (hypoglycemia).
- Work with your healthcare provider (doctor) to adjust your diabetes management plan if you are experiencing frequent hypoglycemia. The more you know about what is causing the episodes, the easier it will be to adjust your plan.
- If you are experiencing low blood sugar and do not have diabetes, you should see your healthcare provider. While it is rare that the underlying cause is a serious condition, it is possible. It is better to get checked out sooner rather than after.
FAQs
When this happens, you can experience symptoms such as sweating, shaking, a fast heartbeat, feelings of nervousness or anxiety, dizziness, hunger, and irritability. Certain people, particularly those with type 1 diabetes, who experience repeated episodes of hypoglycemia, may create hypoglycemia unawareness.
Your doctor may tell you to have really sugary foods or drinks (such as regular soda, orange juice, or cake frosting) or might give you glucose tablets or gel to take — all of these can assist to raise your blood sugar level fast, which is what you need to do when it’s low. Wait about ten minutes to let the sugar work.
The good news is that this condition can sometimes be reversed — allowing people to once again notice the signs of low blood glucose — if hypoglycemia is avoided for a certain week through careful monitoring of blood glucose.
In general, having problems with symptoms that are associated with mild low blood sugar does not indicate diabetes, and does not suggest there is a particularly higher risk for diabetes. However, there are cases when there might be a tie to in.
Best foods for low blood sugar
Candy. When hypoglycemia occurs, patients should follow the 15 to 15 rule.
Fresh or dried fruit. Fruits that provide the appropriate amount of carbohydrates involve half a banana, 15 grapes, two tablespoons of raisins, or a small apple or orange.
Fruit juice.
Fat-free milk.
Honey.
Foods that are not suitable for people with hypoglycemia to eat because they can cause your blood sugar levels to differ significantly involve:
White bread, white rice, & pasta.
Trans fats.
Sugar-sweetened drinks.
Fruit-flavored yogurt.
Sweetened breakfast cereals.
Honey, agave nectar, & maple syrup.
Dried fruit.
Hypoglycemia (Holistic)
Choose foods with fiber.
Eat light, & eat sometimes.
Give chromium a go.
Cut back on refined carbs.
Say no to alcohol & caffeine.
Hypoglycemia, or low blood sugar levels, can also happen in people without diabetes. Possible causes involve alcohol use, certain medications, serious infections, and serious issues affecting your organs.
This can conduct in blurred vision, difficulty concentrating, confused thinking, slurred speech, numbness, and drowsiness. If blood glucose stays low for too long, starving the brain of glucose, it may conduct to seizures, coma, and very rarely death.
Eating a healthy diet with plenty of fruit and vegetables, maintaining a healthy weight, and getting regular physical activity can all assist. Other tips include: Keeping track of your blood sugar levels to look at what makes them go up or down. Eat at routine times, and do not skip meals.




3 Comments