Dancer’s Heel
Table of Contents
What is a Dancer’s Heel?
“Dancer’s heel,” also known as “dancer’s tendinitis,” is a condition that primarily affects individuals who engage in activities requiring repetitive or excessive use of the foot and ankle muscles, such as dancers and athletes.
This condition is characterized by pain and discomfort in the back of the heel, particularly around the Achilles tendon and the surrounding tissues.
Description
The ankle is an essential joint to understand in the context of a dance injury due to it is the relationship between the lower leg and the foot that helps select lower limb stability. This is one of the most often injured sites of the body when dancing. The prevalence of ankle complex damages varies from 27% to 49% of all damages in ballet, modern, flamenco, and tap dancers.
Dancer’s tendinitis also known as Flexor Hallucis Longus tendonitis (FHL) is an overuse injury in which the plantar joints are repeatedly bent and Dorsal flexion (pointing and flexion) of the foot leads to FHL tendinitis.
In dancers, FHL injuries are often caused by repetitive motion caused by changing posture from a crouched to a raised position. (Plié is a French term meaning to bend over, and relieve is a ballet term meaning “to let loose.” The term relieve explains the action when a dancer stands on tiptoe.) This move creates a force ten times the dancer’s body weight.
Flexor Hallucis Longus (FHL) is also known as the “Achilles of the foot” because of its unique role in controlling pronation and supination between the feet, as well as due to its mechanical and physiological characteristics, which enable it to function as a strong transducer from the rear of the foot to the big toe. Because of its amazing anatomical arrangement and activity, it is a generally injured muscle-tendon unit in the athlete population.
This is often referred to as “dancers’ tendinitis” because it is so common in classical ballet dancers. Nevertheless, it will impact all sports that need repetitious push-ups and extreme foot flexions like
swimmers, sprinters, soccer players, and athletes, gymnastics athletes.
Anatomy and related biomechanics
Flexor Hallucis Longus (FHL)
- FHL arises from the posterior and distal two-thirds of the fibula, the interosseous membrane of the limb, and the intermuscular wall.
- It is located distal and lateral to the ventral side of the flexor long finger (FDL) and deep within the soleus and leg muscles. It is pennant-shaped, so the muscle fibers elongate and converge toward its tendon as it passes through the back of the lower tibia.
- The FHL tendon then passes posterior to the talus and penetrates the medial retinal structures at the medial posterior ankle level.
- It is surrounded by a synovial capsule and passes through a fibromuscular tunnel between the medial retina and hence the lateral talus nodules.
- Because it rotates toward the arch, it lies beneath the calcaneus muscle, forming a transverse cortical bone above the calcaneus.
- Therefore, the FHL is part of the tarsal tunnel and within the tunnel, it is located behind the vascular bundle. The Flexor Hallucis Longus tendon moves through the arch of the foot.
- This is called “Henry’s Knot”. At this level, the FHL is located dorsally on the medial edge of the plantar fascia.
- This tendon resumes to extend in the middle of the two sesamoid bones of the first metatarsal joint (MTP) and is protected by the interphalangeal ligament and inserted into the distal phalangeal base of the big toe.
- Thus, the FHL binds to three retinal structures (at the level of the tarsal tunnel, Henry’s node, and the intervertebral ligament) and this is meant to create abnormal compression and stress on the tendon that can lead to injury.
- FHL injuries occur when dancers fail to meet the joint’s natural movement requirements.
- For example, when performing the relief, the forefoot is not strong enough and the external rotation of the limb and the muscular support of the hip joint are out of sync with the heel lift, resulting in a sickle and unstable foot position.
- In contrast, poor control of weakened leg muscles when performing the plie is due to stress on passive support structures such as the plantar ligament, ankle capsule, and plantar fascia.
- This can lead to bone misalignment, increased bone loading, and increased risk of overuse syndrome. different organizations.
- Both maneuvers place a great deal of stress on the ankle and foot as the bones carry weight and the soft tissue must compress them sufficiently to control their position and minimize injury increase.
Heel bone (calcaneus):
The large bone at the back of the foot forms the base of the heel.
Growth plate (epiphysis):
This is the cartilaginous area at the end of the bone that is involved in bone growth. In dancer’s disease, the growth plate of the heel bone is affected.
Achilles tendon:
This is a strong tendon that connects the calf muscle to the back of the heel bone.
plantar fascia:
A thick band of fabric that extends from the heel bone to the base of the toe provides arch support.
- During periods of rapid growth, the Achilles tendon and calf muscles can become tense, putting more stress on the growth plate behind the heel.
- This may cause inflammation and pain in the region.
- Adequate rest, stretching, and proper footwear are often recommended to manage the condition and reduce symptoms.
- If you are concerned, it is important to consult your doctor for an accurate diagnosis and treatment advice.
Epidemiology of dancer’s heel
Dancer tendonitis, or heel epiphysitis, is a relatively common condition in young athletes and active adolescents. It primarily affects children between the ages of 8 and 14, and it occurs most frequently during the adolescent growth spurt. Here it is some important points about the epidemiology of tendonitis in dancers:
Age:
Dancer tendonitis usually occurs in children aged 8-14, most commonly in girls aged 10-12 and boys aged 12-14. This corresponds to the period of growth plate activity and rapid bone growth.
Gender:
This is more common in boys than girls, perhaps because boys tend to experience their growth spurt a little later than girls.
Activity level:
The condition is common in young athletes and active people who participate in running and jumping sports such as soccer, basketball, gymnastics, and dancing.
Risk factor:
Common risk factors include rapid growth, tight calf muscles, and strenuous exercise that strains the heel bone and growth plate.
Prevalence:
Although the exact prevalence of tendonitis in dancers varies, it is considered one of the most common causes of heel pain in children and adolescents. It is estimated that up to 15% of active young people may be affected.
Seasonal difference:
There is evidence that this condition is more prevalent during sports seasons when these activities are more intense.
Self-limitation:
Dancer tendonitis is a condition that usually heals on its own. As growth slows and growth plates close, symptoms tend to improve and eventually disappear.
It’s important to note that while dancers’ tendonitis can be uncomfortable and painful, it’s not a severe or long-term condition. Proper management, including rest, proper footwear, stretching, and sometimes physical therapy, can help relieve symptoms and ensure a smooth recovery. If your child has persistent or severe heel pain, a doctor should be consulted for an accurate diagnosis and advice.
Causes of Dancer’s Heel
Severe disease, also known as calcaneal spondylitis, is primarily caused by repetitive stress and pressure placed on the growth plate of the heel bone (calcaneus) during a period of rapid growth. Several factors contribute to the development of dancer’s tendonitis
Rapid growth :
During the growth phase, bones tend to grow faster than muscles and tendons, causing these soft tissues to tighten. An imbalance between bone growth and soft tissue flexibility can lead to increased pressure on the growth plate.
Muscle and tendon strains:
Tight calf muscles and Achilles’ tendons can exacerbate pressure on the growth plate. This tightness can be caused by the bone growing quickly or not stretching it long enough.
High-impact activities:
Running, jumping, and other high-impact movements can put extra pressure on the growth plate. Sports such as football, basketball, gymnastics, and dance are often associated with tendonitis in dancers due to these movements.
Unsuitable footwear:
Inappropriate or unsupportive shoes can contribute to the development of a dancer’s tendonitis. Shoes that don’t provide arch support or adequate cushioning can add stress to the heel area.
Biomechanical factors:
Abnormal foot mechanics, such as overspending (the foot rolls inward excessively) or high arches of the foot, can place stress on the heel and Achilles tendon, increasing the risk of dancer’s disease.
Excessive activity:
Strenuous physical activity without proper rest can contribute to this condition. Overtraining and insufficient recovery time does not allow the soft tissues to adapt and recover adequately.
It’s important to note that the dancer’s tendonitis is not caused by the dance itself, despite the name. Instead, it occurs during growth spurts and is more common in active children and adolescents participating in high-impact sports. If your child has persistent heel pain, a medical professional should be seen for proper diagnosis and treatment.
Symptoms of Dancer’s Heel
Severe disease, or calcaneal apophysitis, is characterized by a variety of symptoms, mainly involving pain and discomfort in the heel. Common symptoms of dancer’s tendonitis include:
Heel pain:
The most prominent symptom is a pain in the back of the heel, often felt where the Achilles tendon attaches to the heel bone. The pain can be described as a dull ache or a throbbing sensation.
Limping:
The child may limp slightly or change the way he walks to avoid putting pressure on the painful heel.
Discomfort during activity:
The pain is often more pronounced during or after physical activities that involve running, jumping, or impact, such as playing sports or active play.
Morning stiffness:
Some children may experience stiffness and discomfort in their heels when they wake up in the morning or after a period of rest.
Redness and swelling:
In some cases, there may be slight redness and swelling around the heel area.
Tenderness to touch:
The back of the heel can be sensitive to touch or pressure.
Heel warmth:
The affected heel may feel warm to the touch due to inflammation in this area.
- It’s important to note that a dancer’s tendonitis is a temporary condition that usually resolves on its own after the growth plate closes and a child’s bones stop growing rapidly.
- However, proper management is important to reduce discomfort and prevent it from getting worse.
- If your child has symptoms suggestive of Sever’s disease, they should see a health care professional, such as a pediatrician or sports medicine specialist, to confirm the diagnosis and receive appropriate advice for treatment and symptom relief.
Differential diagnosis
Several conditions can present with symptoms similar to a dancer’s tendonitis, so it is important to consider this potential differential diagnosis when evaluating a youngster with heel pain. Some conditions that can be confused with a dancer’s tendonitis include:
Plantar fasciitis:
This condition involves inflammation of the plantar fascia, the tissue that runs along the sole. It can cause heel pain, especially in the morning or after periods of rest.
Achilles tendonitis:
Achilles tendonitis can cause pain in the back of the heel, similar to Sever’s disease. This condition is more common in adults but can occur in active adolescents.
Stress fracture:
A stress fracture of the heel or other metatarsal bone can cause localized pain, which is worse with activity and improves with rest.
Tarsal Coalition:
It is a congenital condition in which two or more bones in the foot join together abnormally, causing pain and stiffness in the foot.
Achilles tendonitis:
This is another term for dancer’s tendonitis, so it’s important to distinguish it from other causes of heel pain.
Calcaneal bursitis:
Bursitis (fluid-filled sac) located at the back of the heel can cause pain and swelling in this area.
Bone cysts or tumors:
Although rare, bone cysts or tumors in the heel area have the potential to cause localized pain.
Inflammatory conditions:
Conditions like juvenile idiopathic arthritis can cause joint pain and inflammation in various parts of the body, including the heels.
Nerve Entrapment:
Rarely, compression or irritation of a nerve in the foot can lead to heel pain.
Proper evaluation by a medical professional, such as a pediatrician, orthopedist, or sports medicine specialist, is crucial for an accurate diagnosis and appropriate treatment. History, physical examination, and sometimes imaging studies (such as X-rays) can be used to distinguish a dancer’s disease from other possible causes of heel pain.
Diagnosing a dancer’s heel
The diagnosis of dancer’s tendinitis, or Achilles tendonitis, usually involves a combination of medical history, physical examination, and sometimes imaging studies. Here’s how the diagnosis is usually made:
Medical background:
The healthcare provider will begin by asking about the child’s symptoms, including how the pain started, activities that worsen or ease the pain, and any relevant medical history.
Physical examination:
The healthcare provider will perform a thorough physical examination of the affected foot. They will evaluate the heel area for pain, swelling, and warmth. They may also evaluate the person’s gait and foot mechanics to identify contributing factors.
Palpation:
The provider may gently press the back of the heel to assess tenderness in the growth plate and surrounding areas.
Range of Motion:
The provider may test the ankle and foot range of motion to assess for any limitations or abnormalities.
Image studies:
In most cases, imaging studies such as X-rays are not needed to diagnose a dancer’s tendonitis because it is a clinical diagnosis. However, an X-ray may be ordered if the healthcare provider wants to rule out other possible causes of heel pain, such as stress fractures or structural problems.
Positive Tomasen test:
- This test evaluates the effect of the first motion MTP.
- This test was performed by assessing the first MTP motion in both positions, i.e. maximal arch flexion and moderate dorsal ankle flexion.
- To conduct the test correctly, the first tarsal head must be stabilized in order to avoid compensatory flexion of the first tarsal head.
- A positive test is discomfort or decreased extensibility of the first MTP joint 20 degrees with ankle reflex.
- When a therapist allows the person to release the foot and directly flex the sole and point the foot out, they will have a better big-toe range of motion.
- This happens because when flexing the instep, it stretches that tendon.
The healthcare provider will look at other potential causes of heel pain and rule out conditions that mimic the symptoms of Dancer’s tendonitis.
Based on information gathered from the medical history, physical examination, and any necessary imaging studies, the healthcare provider will diagnose the dancer’s disease if the clinical findings are consistent with the clinical features. disease score.
Medical treatment for Dancer’s Heel
Medical treatment for dancer’s tendonitis (heel tendonitis) focuses primarily on managing symptoms, relieving pain, and healing the child’s body. Below given are some common approaches to medical treatment:
Rest:
Resting the affected foot is essential to give the inflamed growth plate time to heal. Reducing or avoiding activities that make pain worse, such as running or jumping, can help with recovery.
Ice:
Applying ice to the painful area for about 15 to 20 minutes every few hours can help reduce inflammation and relieve pain.
Anti-inflammatory drugs:
Over-the-counter NSAIDs such as ibuprofen can help decrease pain and inflammation. However, their use should be under the guidance of a healthcare professional, especially in children.
Heel pads or orthotics:
Heel pads or special orthopedic pads that provide arch support and cushioning can help reduce pressure on the heel and improve foot mechanics.
Stretching exercises:
Gentle calf stretches can help improve flexibility and reduce stress in the Achilles tendon and calf muscles. A healthcare provider or physical therapist can recommend appropriate stretches.
Physical therapy:
In some cases, a physical therapist can provide exercises and techniques to address muscle imbalances, improve flexibility, and promote proper foot mechanics.
Activity modification:
Adjusting a child’s activity level or changing their exercise routine to avoid high-impact activities can prevent further stimulation of the growth plate.
Suitable footwear:
Choosing supportive cushioning shoes with good arch support can help reduce stress on the heel area. It is important to avoid shoes with minimal cushioning or inadequate support.
Gradual Return of activity:
Once the pain subsides and healing progresses, physical activities should be gradually resumed under the guidance of a medical professional.
Monitoring Growth:
As the growth plates close and the child’s bones mature, the symptoms of the dancer’s tendinitis usually go away. Regular check-ups with a healthcare provider can ensure that the condition is progressing as expected.
It is important to note that each child’s condition is unique and treatments may vary. You should consult a medical professional, such as a pediatrician or sports medicine specialist, for an accurate diagnosis and to recommend an individualized treatment.
Physiotherapy treatment of dancer’s heel
Physical therapy can play a valuable role in managing a dancer’s tendonitis by treating muscle imbalances, improving flexibility, and promoting table mechanics. suitable foot. A physical therapist can design a treatment plan that is tailored to the needs of each child. Here are some common physical therapy treatments for Dancer’s disease:
Conservative care for dancer’s tendonitis
Protocol of peace and love
- Following the Peace and Love protocol, especially with anti-inflammatory medications and regular ice application, can help reduce inflammation significantly in the early stages of this disease.
- It is also important to follow the appropriate nutritional, dietary, and possibly pharmaceutical recommendations.
Stretching exercises:
A physical therapist can guide children through specific stretches to improve flexibility in the calf muscles and Achilles tendon. Gentle, consistent stretching can help relieve tightness and reduce stress on the growth plate. Stretching exercises can help manage a dancer’s tendonitis by helping to relieve tension in the calf muscles and Achilles tendon, which can contribute to heel pain. Here are some stretching exercises that may be recommended:
Calf stretching against the wall:

- Start with standing facing the wall with the hands resting on the wall at shoulder height.
- Step back with one foot and keep it straight, heel touching the ground.
- Bend the front knee while keeping the back leg straight and the heel touching the ground.
- Hold the stretch for about 20 to 30 seconds, then switch sides.
On Stairs calf stretch:
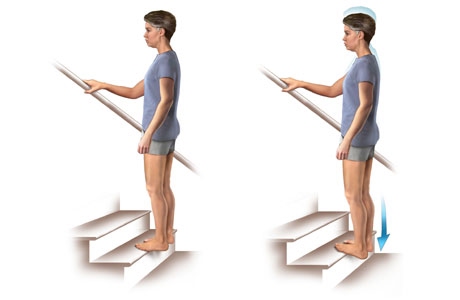
- Start with standing on stairs or sturdy raised surfaces with the soles of the feet resting on the step and heels hanging over the edge.
- Gently lower the heels to the bottom of the ladder to feel the stretch in your calf muscles.
- Maintain the stretch for about 10 to 20 seconds.
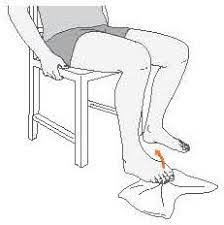
Achilles stretch while sitting:
- Begin with sitting on the floor with your legs stretched out in front of you.
- Muffle a towel or resistance band around the soles of the feet.
- Gently pull on the towel or bandage while flexing the ankle to bring the toes toward you.
- Maintain the stretch for about 10 to 20 seconds, then change sides.
Toes raise on one step:
- Start with standing at the edge of a ladder with the heels hanging over the edge.
- Gradually lower the heels below step level, feeling the stretch in the calves.
- Lift the heels back to the initial position.
- Do several repetitions of this movement.
Ankle circles:
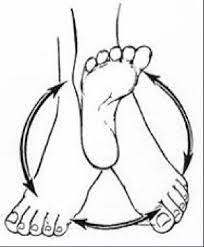
- Begin with sitting in a chair or on the floor.
- Lift one foot off the floor and gently rotate the ankle in clockwise and counterclockwise circles.
- Make several circles in each direction.
- Remember that stretching should be done gently and painlessly. Maintain each stretch for about 10 to 20 seconds and repeat several times on each leg.
It is important to consult a health care professional or physical therapist before starting any new exercise routine, especially if your child is experiencing pain. They can advise on proper stretches and make sure they are safe and effective for your child’s specific condition.
Strengthening exercises:
Strength exercises can target the appropriate mechanical support muscles of the foot. This includes exercises for the calf muscles, as well as other leg muscles, to promote stability and balance. Strength exercises can help improve muscle balance and support proper foot mechanics, which can be beneficial in managing a dancer’s tendonitis. Here are some strength exercises that may be recommended:
Toe raises:
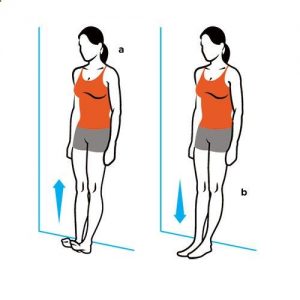
- Start with standing straight with your feet flat on the floor.
- Slowly lift your heels off the ground, placing your weight on your toes.
- Lower your heel to the floor.
- Do several repetitions of this movement.
Calf raises:
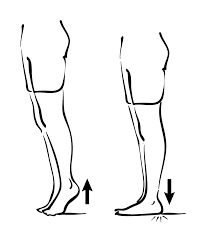
- Start with standing straight with your feet flat on the floor.
- Standing on your toes, lift your heels off the floor.
- Slowly lower your heel to the floor.
- Do several repetitions of this movement.
Heel drops on a step:
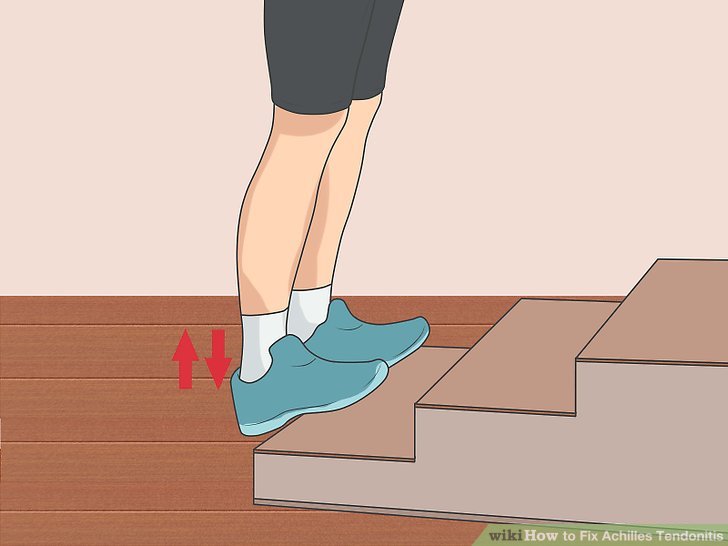
- Stand on the edge of the step with the soles of your feet resting on the step and your heels hanging over the edge. Slowly lower your heels below step level.
- Stand up on your toes.
- Do several repetitions of this movement.
Ankle planterflexion with resistance band:

- Sit in a chair with a resistance band wrapped around the ball of one foot.
- Hold the ends of the band and bend your ankles under the resistance of the band.
- Gradually release the tension and back to the starting position.
- Do several repetitions on each leg.
Single-leg balance:

- Standing on one leg maintains your balance.
- Keep your core engaged and your body steady.
- Hold this position for about 20 to 30 seconds and then switch legs.
Calf Raises on an Incline Surface:
- Stand on a slightly inclined surface (like a corner or a ramp), face up.
- Standing on your toes, lift your heels off the floor.
- Slowly lower your heel to the ground.
- Do several repetitions.
Towel scrunch with a heel lift:
- Place the towel on a smooth surface, such as tile or hardwood; put one foot on the towel.
- Actively start rubbing the big-toe ball under the toes.
- One by one, lift the heel off the towel (heel and big toe should be in flexion if done correctly).
- Place the heel back onto the towel and flex the big toe to start the sequence again.
- Do this until the towel is completely under your feet.
- This may be accomplished from a sitting or standing position.
Marble/ ball pickups:

- Using the 1st and 2nd toes, bend your back to pick up the marble/ball and drop it into the cup/box by flexing the soles of your feet.
- Must be completed in a standing position.
Edge hover:
- Standing on the edge of the step with the 1st and 2nd toes supported by the three outer toes suspended in space, actively press the first toe into the step and try to lift and keep the heel off the step.
- They can be held for 15-20 seconds.
Strengthens the gastrocnemius and soleus complex:
- From a standing position, perform a step lift by keeping one big toe on the outside of the step and pushing up into the step position.
- This exercise strengthens the gastrocnemius and soleus complex.
Remember that these exercises should be performed in a painless range of motion. Start with a controllable number of repetitions and gradually increase as your child’s strength improves. You should consult a healthcare professional or physiotherapist before starting a new exercise routine to ensure that the exercises are appropriate for your child’s condition and to prevent any serious symptoms.
Gait analysis:
A physical therapist can analyze the child’s gait (walking pattern) to identify any abnormalities or imbalances that may be contributing to the condition. Mechanically adjusting the gait can help reduce stress on the heel.
Manual therapy:
Hands-on techniques such as massage and manual manipulation can help relieve muscle tension, improve blood circulation, and promote wound healing in the affected area.
Massage techniques and manual manipulation can help relieve muscle tension, improve blood circulation, and promote the healing of a dancer’s tendonitis. Here are some methods a medical professional or trained therapist can use:
Soft tissue massage:
- A therapist uses their hands to apply gentle pressure and massage techniques to the muscles around the calves and heels.
- This helps to relax tense muscles, relieve muscle tension and improve blood flow to the affected area.
Myofascial release:
- Myofascial release techniques target the fascia, the connective tissue that surrounds the muscles, and other structures.
- The therapist uses gentle pressure to stretch and release constraints in the balance, which can contribute to muscle tension.
Active release technique (ART):
- ART is a technique that involves a combination of motion and deep pressure to treat soft tissue constraints and adhesions.
- It is commonly used to break up scar tissue and improve flexibility.
Joint mobilization:
- Joint mobility involves the therapist gently moving the joints of the foot and ankle through their natural range of motion.
- It can help improve joint mobility, reduce stiffness, and promote healing.
Trigger Point Therapy:
Trigger points are areas of muscle that are sensitive to the touch and can contribute to referred pain.
Therapists apply pressure to these points to release tension and relieve pain.
Stretching and manipulation techniques:
The therapist can instruct the child to perform passive stretching techniques to improve flexibility and release tension in the calves and Achilles tendon.
Heat therapy:
Heat can be applied to the area before or after the massage to relax muscles and improve blood circulation.
- It is important to note that these techniques must be performed by qualified medical professionals or therapists trained in these modalities.
- A healthcare provider should be consulted before starting any manual therapy technique, especially for children.
- They can help determine the right approach and ensure that treatment is appropriate for the child’s specific condition and needs.
Tape or brace:
The physiotherapist may use bandaging or splinting techniques to add extra support to the heel and relieve stress on the heel. growth plate during physical activity.
Orthotics prescription:
If needed, a physiotherapist can recommend and prescribe custom orthotics that provide the right cushioning and arch support to help relieve discomfort.
Education and Activity Modification:
A physical therapist can educate children and their parents about the condition, proper footwear, and activity modifications to prevent the worsening of symptoms.
Home Exercise Program:
A structured home exercise program tailored to a child’s needs can help maintain and improve the progress made during physical therapy sessions.
Gradual Return to Activity:
- The physical therapist will guide the child back to physical activities safely by gradually increasing the intensity and impact while watching for any signs of discomfort.
- Communicate with other healthcare providers: Physiotherapists often work with chiropractors, and other healthcare professionals to provide comprehensive, coordinated care.
Remember that each person’s condition is unique, so the physical therapy treatment plan will be individualized to their specific needs and situation. If you are considering physical therapy for a dancer’s heel, you should consult a medical professional to ensure that the treatment is appropriate for your diagnosis and medical history.
FAQ
Dancers often have bone spurs on the talus. This can lead to a posterior ankle bump at the back of the ankle. However, dancers are no more likely to have a common heel under the foot than anyone else.
Coping with heel pain in dancers
It is very common for dancers to experience more heel pain when they have a busier training or class schedule. In addition, en pointe dancers – i.e. those who start or perform more difficult sections – may experience more pain in the heel area. Now, ballet isn’t the only type of dance that causes heel pain.
Heel pain usually goes away with non-surgical treatments, but recovery takes time. You need to be patient and give your body time to repair itself. If you return to your usual activities too quickly, it can slow down your recovery. In infrequent cases, you can require surgery.
Walking on flat ground is a great way to increase your walking speed and endurance without irritating the painful Achilles tendon.




One Comment