Phrenic Nerve Palsy
Table of Contents
What is Phrenic Nerve Palsy?
The phrenic nerve, which extends from the neck to penetrate the diaphragm next to the pericardium, can suffer lesions anywhere along its journey, which is what causes phrenic nerve palsy, also known as paralysis or paresis of the phrenic nerve.
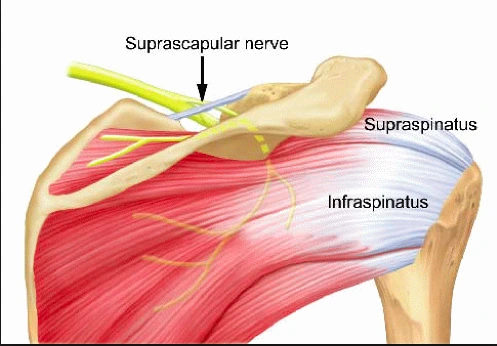
What is the phrenic nerve?
Your diaphragm, a sizable dome-shaped muscle situated between your chest and abdomen, is controlled by the phrenic nerve. On it, breathing depends. Your diaphragm contracts as a result of your nerve, flattening and thinning it. Your lungs will have greater room to expand and take in air as a result of this motion. Once your diaphragm relaxes as a result of less phrenic nerve stimulation, your lungs contract and you exhale air.
The phrenic nerve, which extends from the neck to penetrate the diaphragm next to the pericardium, can suffer lesions anywhere along its journey, which is what causes phrenic nerve palsy, also known as paralysis or paresis of the phrenic nerve.
Epidemiology
Since phrenic nerve palsy can have many different causes, no one demographic is impacted. As a result, the epidemiology will be consistent with the underlying cause.
Causes of Phrenic Nerve Palsy
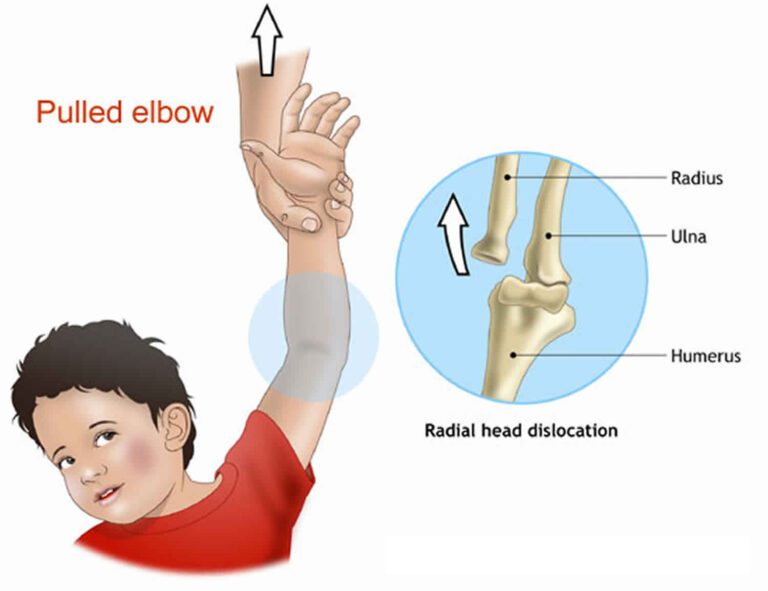
Phrenic Nerve Paralysis can happen at birth, after trauma, or as a result of radiation, a tumour, or a virus. Depending on the circumstances, the nerve may sustain injury directly or be stretched, ruptured, avulsed, or avulsed. In stretch-type injuries, the nerve’s outer covering and blood supply are pushed apart, but the nerve’s interior portion is kept intact.
When a nerve is totally severed, two free ends are left that can no longer communicate with one another. In avulsion-type injuries, the nerve is physically severed from the spinal cord, which serves as its electrical supply. The nerve suffers indirect harm when it is exposed to radiation, a tumour, or when a virus turns it off.
Many instances are postviral, idiopathic, or both. Typical reasons include:
- Malignancy
- Bronchogenic carcinoma
- Pulmonary metastases
- Mediastinal tumors or neck malignancy
- Trauma and iatrogenic
- Penetrating injury
- Chiropractic manipulation
- Postoperative: especially cardiac: up to 10% of cases
- Central venous catheters
- Direct trauma
- Compression by hematoma
- Local anesthetic infiltration
- Intrascalene brachial plexus nerve blocks
- With ultrasound guidance and the use of less local anesthetic, the incidence was decreased.
- Forceps delivery (newborn)
- Neuromuscular diseases
- Parsonage-Turner syndrome
- Chronic inflammatory demyelinating polyradiculoneuropathy (CIDP)
- Inflammation
- Pneumonia
- Empyema
- Pleurisy
- Herpes zoster infection
- Direct compression
- Aortic aneurysm
- Cervical osteophytes
Symptoms of a Paralyzed Diaphragm
Electrical signals in the phrenic nerve stop moving from the brain to the diaphragm muscle when it is damaged. The diaphragm muscle shuts down, and the patient can experience breathing problems. The patient may be able to breathe properly on the opposite side if the phrenic nerve is solely paralyzed on one side (the right or left). The patient cannot breathe on their own when both sides of the phrenic nerve are paralyzed (on the right and left, respectively). The patient may need a ventilator machine to assist them breathe in the event of a medical emergency.
The presentation will, without a doubt, rely on the underlying reason. Patients are frequently asymptomatic in many cases of unilateral (the majority of cases) phrenic nerve paralysis. Patients frequently describe dyspnea and orthopnea when phrenic nerve palsy is the cause of the presentation. Tests of respiratory function frequently follow a constrictive trend.
The symptoms of bilateral phrenic nerve paralysis are not only more severe but also worsen when the patient is lying down.
Risk Factors
Despite being an uncommon ailment, there are several circumstances or medical problems that increase a person’s risk, such as:
- After a heart or neck operation, surgical trauma
- Interscalene nerve blocks that cause harm
- A neck injury caused by chiropractic manipulation
- Phrenic nerve damage caused by birth trauma in neonates and young children
- Neurological diseases such as Guillain-Barre syndrome, multiple sclerosis, muscular dystrophy, and amyotrophic lateral sclerosis (ALS)
- Radiation
- Lung or lymph node cancer that pushes the phrenic nerve
- Abnormalities of the spinal cord and quadriplegia
- Phrenic nerve surgery, which involves cutting or removing the nerve to treat a tumour,
- Heart arrhythmias, persistent bronchitis, or pneumonia
- Autoimmune and thyroid conditions are examples of neuropathic diseases.
Diagnosis:
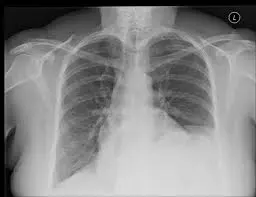
Typically, a history and physical exam searching for evidence of breathing trouble can identify phrenic nerve paralysis. A nerve conduction and muscle test might be requested when the diagnosis is ambiguous to learn more about the condition of the diaphragm muscle, the right and left phrenic nerves, or both. The position and state of the diaphragm may be seen on a typical X-ray. An even more in-depth X-ray technique is called chest fluoroscopy, which may display the diaphragm’s right and left sides moving as the patient breathes in and out.
Radiographic features:
Simple radiograph
Sometimes the diagnosis is quite clear. Understanding the normal level of the diaphragms is crucial, though, as their position is not symmetrical (see the normal position of the diaphragms on chest radiography). One of the various reasons for diaphragmatic elevation should be looked for if the left hemidiaphragm is higher than the right or if the right is higher than the left by more than 2 millimetres. Of course, this also applies to phrenic nerve palsy
Fluoroscopy
Fluoroscopic examination of the diaphragm (sometimes known as the “sniff test”) includes rapid inhalation while the hemidiaphragm’s are being seen.
With inspiration, both hemidiaphragms in healthy people fall. Paralysis of the phrenic nerve causes paradoxical upward movement on the side that is affected
CT scan:
Since supine posture and varied inspiratory effort can considerably modify diaphragmatic height, CT CT has limited use in the diagnosis of a raised hemidiaphragm ref. Despite this, it is excellent at detecting various phrenic nerve palsy causes and can gather volumetric data from the base of the head to the upper belly.
MRI
MRI is especially well-suited for evaluating Pancoast tumors and is more effective in identifying tumor extension in these circumstances.
Conduction and electromyography research
Phrenic nerve conduction studies may be carried out with the placement of an esophageal electrode to record diaphragmatic contractions and stimulation of the neck nerve using either surface stimulation or an electrode with a monopolar needle at the cricoid cartilage level.
An alternative test is diaphragmatic electromyography. The two tests complement one another
Conduction investigations may also make use of fluoroscopy to verify diaphragmatic movement.
Differential diagnosis:
A phrenic nerve palsy is simply a raised hemidiaphragm, and the following common things should be taken into consideration:
- Masses/collections pushing the diaphragm up from below
- Hepatic mass
- Subphrenic collection
- Intra-abdominal fat
- Lung capacity reduction: raising the diaphragm
- Lobectomy
- Radiation induced fibrosis
- Diaphragmatic eventration
In situations of bilateral diaphragmatic paralysis, a variety of factors should be taken into account in addition to bilateral phrenic nerve palsy:
- High spinal cord injury
- Central hypoventilation syndrome (Ondine’s curse)
Treatment of Phrenic Nerve Palsy
Diaphragmatic pacing may be employed in symptomatic unilateral instances or, more frequently, bilateral involvement. Direct muscle stimulation using implanted electrodes or distal phrenic nerve stimulation are two options for doing this.
The majority of asymptomatic patients with unilateral diaphragmatic paralysis do not require treatment. When recognized, the root cause has to be addressed. If the patient still experiences symptoms after treating the underlying cause or if they have bilateral diaphragmatic paralysis, surgical alternatives may be explored. There are several therapeutic possibilities, including plication and stimulation of the phrenic nerve. Plication of the affected area is a very beneficial therapy strategy that facilitates weaning off mechanical respiration. For non-morbidly obese individuals with unilateral diaphragmatic paralysis, plication is preferred. On intact phrenic nerves that show no signs of myopathy, phrenic nerve stimulation is conducted. Patients with bilateral diaphragmatic paralysis and cervical spine injuries can have this treatment.
A physiotherapist performing resistance band therapy Regarding the patient’s shoulder and chest muscles, who is an athlete notion of physical therapy. Physical therapy is the cornerstone of treatment for phrenic nerve paralysis. Physical therapists work with patients to help them use their neck (scalene) and rib (intercostal) muscles, as well as their diaphragm, to breathe more easily. It is suggested that patients have surgical therapy if they still have respiratory problems or need to use a mechanical ventilator.
When performing surgery is advised rather than waiting for the nerve to heal naturally, this is because it is thought to increase the likelihood of subsequent healing. Patients need to be aware that there is a limited amount of time in which the nerves can be fixed. The nerve’s link to the muscle is irreversibly severed by 12–18 months. After then, the wounded nerve will no longer be able to instruct the muscle to contract, even if it is rebuilt. Surgery is available in 6 to 9 months after that, taking into account the fact that a repaired nerve heals at a rate of 1 mm per day.
The goal of surgical therapy is to repair the affected nerve(s). This might consist of some of the following:
- Nerve decompression/neurolysis involves eliminating scar tissue from the area around the nerve so that electrical signals may pass the nerve more freely.
- Removing the scar tissue that is filling the nerve gap and bridging it with a sensory nerve (nerve graft).
- Choosing a motor nerve from a healthy but less significant muscle group (spinal accessory nerve or intercostal nerves) and transferring it to the injured phrenic nerve (nerve transfer);
Prognosis
The underlying reason affects the prognosis. In cases of neoplastic involvement, nerve function typically does not return. The paralysis is caused by compressive lesions, just like other compressive neuropathies. Gradual rehabilitation is possible, although it typically takes several months or even years.
The underlying causes and the state of pulmonary function affect the mortality and morbidity of diaphragmatic paralysis or damage to the phrenic nerve. Generally speaking, unless the patient is suffering acute shortness of breath, unilateral diaphragmatic paralysis has a decent prognosis. In cases of bilateral diaphragmatic paralysis, recovery typically takes more than a year.
FAQs:
In a trial involving 213 patients who had this problem, 78.4% of them improved without medication. 40% of individuals who weren’t able to make a full recovery had a major underlying ailment. Your sixth nerve palsy’s etiology will often determine your course of treatment. Once the reason is remedied, the condition often disappears.
My areas of expertise include plastic surgery and head and neck surgery. Thoracic or otolaryngology surgeons may come across the phrenic nerve, but they should really attempt to avoid it as it is not frequently handled outside of neck or chest surgery.
Hurt or irritated nerve: Chronic hiccups can be caused by phrenic or vagus nerve damage or inflammation. These nerves supply the diaphragm muscle.
If the phrenic nerve is damaged, the diaphragm might become paralyzed. You can also have respiratory issues in addition to sleep issues. Severe phrenic nerve damage may necessitate the use of a mechanical ventilator for breathing in some patients.
When a newborn is delivered violently, lateral neck hyperextension during birth can cause a strain injury that can lead to phrenic nerve palsy. This might be an uncommon cause of abnormal breathing in the neonatal period, which causes respiratory distress.