Gate control theory of pain
Table of Contents
What is pain?
Pain is a complex and subjective experience that can be caused by a variety of stimuli, such as physical injury, disease, or emotional distress. Pain perception involves a series of processes that occur in the nervous system, including the transmission of signals from peripheral nerves to the spinal cord and brain, where the sensation of pain is ultimately perceived.
The gate control theory of pain, first proposed by Ronald Melzack and Patrick Wall in 1965, suggests that pain perception is influenced by a gating mechanism in the spinal cord that can either allow or block the transmission of pain signals to the brain. This theory has been influential in the development of pain management strategies and has helped to shape our understanding of how pain works in the body.
The anatomy of pain
To understand the gate control theory of pain, it is helpful to have a basic understanding of the anatomy of pain perception. Pain signals originate in peripheral nerves, which detect noxious stimuli such as temperature extremes, pressure, and tissue damage. These signals are transmitted to the spinal cord via sensory neurons, which enter the spinal cord through the dorsal root. Once in the spinal cord, the pain signals are processed by a series of neurons, which transmit the signals to the brain for interpretation and perception of pain.
The gate control theory of pain
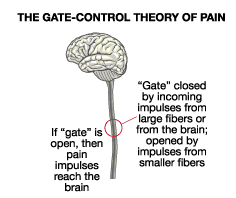
The Gate Control Theory of Pain proposes that pain perception is not a simple linear process, but it is modulated by a complex interplay of factors that occur at various levels of the nervous system. The central idea of the Gate Control Theory of Pain is that there is a neural “gate” located in the spinal cord that can either allow or block nociceptive signals from reaching the brain.
This gate is modulated by two types of nerve fibers: small-diameter unmyelinated C fibers and large-diameter myelinated A fibers. The C fibers transmit information about pain and other unpleasant sensations, while the A fibers transmit information about non-painful sensations, such as touch and pressure.
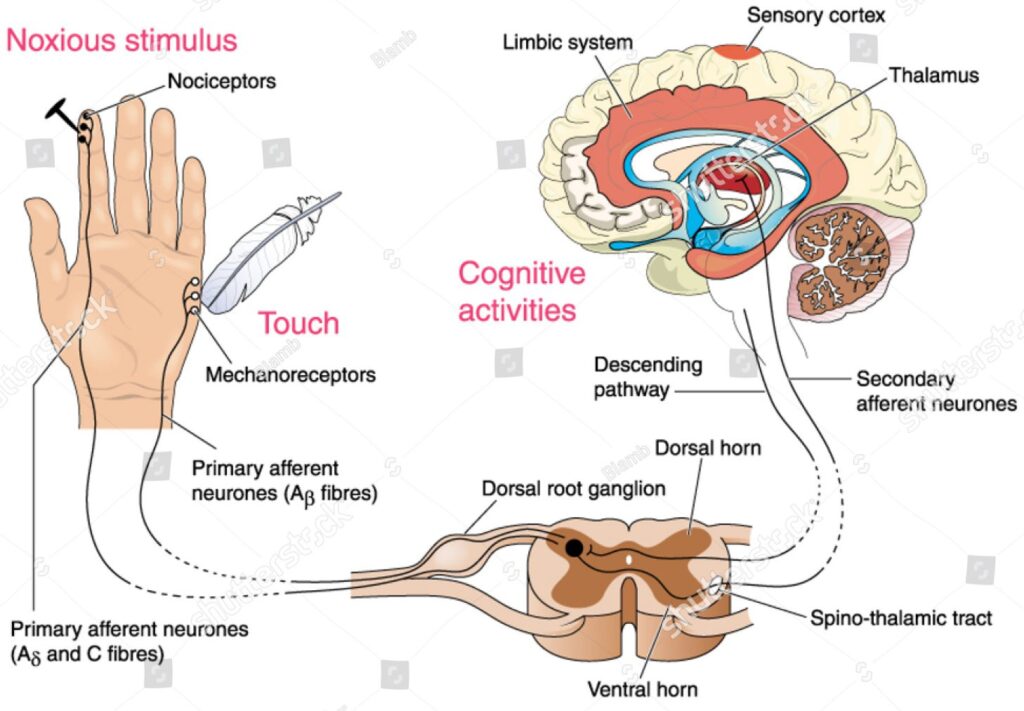
The gate is controlled by a network of neurons located in the dorsal horn of the spinal cord. When the C fibers are stimulated, they release a neurotransmitter called substance P, which activates these neurons and opens the gate, allowing nociceptive signals to pass through to the brain. However, when the A fibers are stimulated, they release a different neurotransmitter called glutamate, which activates a different set of neurons that close the gate, preventing nociceptive signals from passing through.
In addition to these primary fibers, several other factors can modulate the opening and closing of the gate, including descending pathways from the brainstem and higher centers in the brain, as well as other sensory information from the body and the environment. For example, emotional and cognitive factors, such as anxiety and attention, can influence the perception of pain by activating descending pathways that either enhance or inhibit the activity of the dorsal horn neurons.
Implications for pain management
The gate control theory of pain has important implications for the management of pain. One of the key implications is that pain perception can be modulated by non-pharmacological interventions such as physical therapy, cognitive-behavioral therapy, and relaxation techniques. These interventions can help to activate inhibitory pathways in the brain and spinal cord, which can reduce the transmission of pain signals and enhance the gating mechanism in the spinal cord.
Pharmacological interventions can also be used to modulate the gate mechanism in the spinal cord. For example, opioids such as morphine can activate inhibitory pathways in the brain and spinal cord, which can reduce the transmission of pain signals. Non-opioid medications such as gabapentin and pregabalin can also modulate the gate mechanism by reducing the activity of excitatory neurons in the spinal cord.
Conclusion
The Gate Control Theory of Pain has important implications for the treatment of pain. It provides a framework for developing non-pharmacological pain management strategies, such as physical therapy, massage, and acupuncture, which are believed to work by activating the A fibers and closing the gate, thereby reducing the transmission of nociceptive signals to the brain. The theory has also led to the development of new pharmacological treatments for pain that target the neurotransmitters and receptors involved in opening and closing the gate.
Overall, the Gate Control Theory of Pain provides a comprehensive understanding of how pain is perceived and how it can be managed. It has been widely accepted and has led to significant advancements in pain management strategies and treatments. However, it is important to note that the theory is not without its limitations, and further research is needed to fully understand the complex interplay between pain perception and the nervous system.
FAQs
What does the pain gate theory explain?
The pain gate theory is a scientific theory that explains how our nervous system processes and perceives pain. According to this theory, pain signals are regulated by a “gate” mechanism in the spinal cord that can either allow or block the transmission of pain signals to the brain. The gate is influenced by factors such as the intensity of the pain, the individual’s emotional and cognitive state, and various interventions such as medication or relaxation techniques. The theory suggests that a multidisciplinary approach that addresses both physical and psychological factors may be more effective in managing chronic pain.
What are the three pain-control theories?
There are several theories of pain control, but three of the most commonly recognized are:
The Gate Control Theory: This theory suggests that pain signals must pass through a “gate” in the spinal cord before reaching the brain. This gate can be closed or opened by various factors, such as sensory input, emotions, and attention, and can influence the perception of pain.
The descending modulation theory: This theory proposes that the brain can modulate pain signals by sending messages down the spinal cord to block or reduce pain signals. This modulation can be influenced by a variety of factors, including emotions, cognitive processes, and previous experiences.
The Neuromatrix Theory: This theory proposes that pain is a complex experience that involves not only physical sensations but also emotional, cognitive, and social factors. The brain creates a “neuromatrix,” or network of neurons, that represents the experience of pain and can be influenced by a range of factors, including past experiences, expectations, and cultural factors.What are the four steps of pain?
The four steps of pain, also known as the pain pathway, are:
Transduction: The first step is the process by which noxious stimuli (such as tissue damage) are converted into electrical signals, or nerve impulses, by specialized nerve endings called nociceptors.
Transmission: In this step, the nerve impulses generated by the nociceptors are transmitted via nerve fibers to the spinal cord and then to the brainstem and thalamus.
Perception: The third step involves the brain’s interpretation of the incoming nerve impulses as pain. This is where the conscious experience of pain is generated, as the brain processes the information and creates a subjective experience of discomfort.
Modulation: The final step involves the brain’s ability to modulate, or control, the pain experience through various mechanisms, such as the release of endorphins, the activation of descending pain pathways, or the use of analgesic drugs. This step can amplify or dampen the pain experience and also influence the body’s physiological response to pain.What is the gate theory of pain medicine?
The Gate Control Theory of Pain has been supported by numerous studies and has had a significant impact on the development of pain management techniques. Understanding the gate mechanism has led to the development of interventions that can modulate the flow of pain signals, such as transcutaneous electrical nerve stimulation (TENS) and spinal cord stimulation (SCS). These interventions are based on the principle of stimulating non-nociceptive pathways to close the gate and reduce the perception of pain.
What is the application of gate control theory?
The gate control theory has several applications in the field of pain management, including:
Treatment of acute and chronic pain: By understanding the gate control theory, clinicians can develop treatment plans that target the different components of pain perception. This may involve a combination of medication, physical therapy, and psychological interventions.
Sports medicine: The gate control theory can be applied in sports medicine to help athletes manage pain and injuries. Understanding how pain is processed and modulated by the nervous system can help athletes and trainers develop strategies to reduce pain and improve performance.
Physical therapy: Physical therapists can use the principles of gate control theory to develop treatment plans that aim to reduce pain and improve function in patients with musculoskeletal conditions. This may involve techniques such as massage, exercise, and manual therapy.
Psychological interventions: The gate control theory emphasizes the role of psychological factors in pain perception. As such, psychological interventions such as cognitive-behavioral therapy and relaxation techniques can be effective in reducing pain and improving quality of life.

One Comment