Digestive System
Table of Contents
Introduction
The human digestive system consists of the gastrointestinal tract including the accessory organs of digestion (the tongue, salivary glands, pancreas, liver, and gallbladder). Digestion involves the breakdown of food into smaller and smaller components until they can be absorbed & assimilated into the body.
The process of digestion is classified into three stages:
1. The cephalic phase
2. The gastric phase,
3. The intestinal phase.
- The cephalic phase: The cephalic phase of digestion, begins with secretions from gastric glands in response to the sight & smell of food. This stage includes the mechanical breakdown of food by chewing & the chemical breakdown by digestive enzymes, that takes place in the mouth. Saliva contains the digestive enzymes amylase & lingual lipase, secreted by the salivary & serous glands on the tongue. Chewing in which the food is mixed with saliva starts the mechanical digestion process. This produces a bolus which is swallowed down to the esophagus then the bolus enters the stomach.
2) The gastric phase: This stage of digestion begins in the stomach with the gastric phase. The food is then broken down by mixing with gastric acid until it passes into the duodenum.
3) The intestine phase: This stage of digestion begins in the duodenum with the intestinal phase, where partially digested food is mixed with several enzymes produced by the pancreas. Digestion is helped by chewing food by the muscles of mastication, the tongue, the teeth, the contractions of peristalsis, & segmentation. Gastric acid & mucus production in the stomach are essential for the continuation of the digestion of food.
Peristalsis is the rhythmic contraction of the muscles that begins in the esophagus & continues along the wall of the stomach and the rest of the gastrointestinal tract. This initially results in the production of chyme which when fully breakdown in the small intestine is absorbed as chyle into the lymphatic system. Most of the digestion of food takes place in the small intestine then Water & many minerals are reabsorbed back into the blood in the colon of the large intestine. The waste products of digestion are defecated from the rectum via the anus.
Components of Digestive system
Adult digestive system:
There are several organs & other components involved in digestion. The organs called accessory digestive organs are the liver, gall bladder & pancreas. Other components are the mouth, salivary glands, tongue, teeth & epiglottis.
The largest structure of the human digestive system is the GI tract. This begins at the mouth & ends at the anus, covering a distance of about 9 meters.
A major digestive organ is a stomach. Within its mucosa are millions of embedded gastric glands which produce gastric acids. Their secretions are important to the functioning of the organ.
Most of the metabolism of food occurs in the small intestine which is the longest part of the gastrointestinal tract.
The largest part is the colon or large intestine GI tract. Water is absorbed here & the remaining waste matter is stored before defecation.
There are many specialized cells in the GI tract. These include the different cells of the gastric glands, taste cells, pancreatic duct cells, enterocytes & microfold cells.
Some parts of the digestive system are also part of the excretory system such as the large intestine.
Mouth
The mouth is the first part of the upper gastrointestinal tract & is equipped with several structures that start the first processes of digestion. These include salivary glands, teeth & the tongue.
The mouth consists of two parts; the vestibule & the oral cavity proper.
The vestibule: it is the area between the teeth, lips & cheeks & the rest is the oral cavity proper. Most of the oral cavity is lined by the oral mucosa, a mucous membrane that produces lubricating mucus in small amounts. Mucous membranes vary in structure in the different regions of the body but they all produce lubricating mucus, which is either secreted by surface cells or more usually by underlying glands.
The mucous membrane in the mouth continues as the thin mucosa it lining the base of teeth. The main component of mucus is a glycoprotein known as mucin & the type secreted varies according to the region involved. Mucin is viscous, clear, & clinging. Underlying the mucous membrane is a thin layer of smooth muscle tissue & the loose connection to the membrane provides its great elasticity.
The roof of the mouth is termed the palate it separates the oral cavity from the nasal cavity. The hard palate is lie at the front of the mouth since the overlying mucosa is covering a plate of bone; it is softer & more pliable at the back which is made of muscle & connective tissue, and it can move to swallow food & liquids. The soft palate ends at the uvula. The opening between the lips is termed the oral fissure, & the opening into the throat is known as the fauces.
At either side of the soft palate is the palatoglossus muscles that also reach into regions of the tongue. These muscles raise the back of the tongue & also close both sides of the fauces to enable food to be swallowed. The mucus helps in the mastication of food in its ability to soften food & collect the food in the formation of the bolus.
Salivary glands
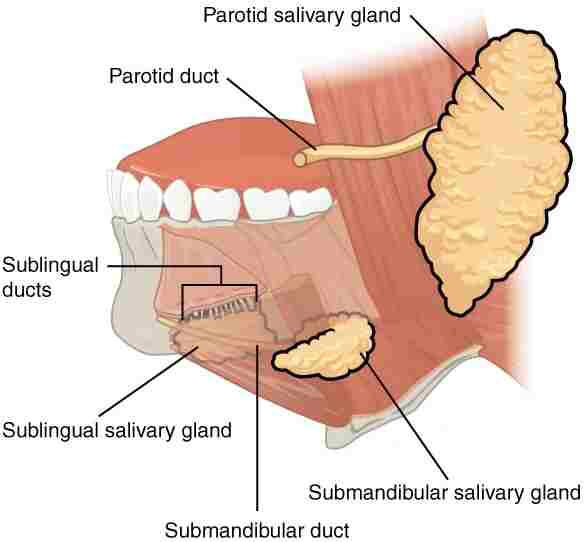
The main salivary glands:
there are 3 pairs of main salivary glands & between 800 and 1,000 minor salivary glands all of which mainly serve the digestive process. it also plays an important role in the maintenance of dental health & mouth lubrication without that speech would be impossible. The main glands are all exocrine glands, secreting through ducts. All glands terminate in the mouth. The largest of these is the parotid gland: their secretion is mainly serous. The next pair are underneath the jaw, called the submandibular glands, these produce both serous fluid & mucus. The serous fluid is produced by serous glands & which also produce lingual lipase. The third pair is known as sublingual glands situated underneath the tongue & their secretion is mainly mucous with a small percentage of saliva.
Within the oral mucosa, & also on the tongue, palates, and floor of the mouth, are the minor salivary glands their secretions are mainly mucous & they are innervated by the 7th cranial nerve. The glands also secrete amylase the first stage in the breakdown of food acting on the carbohydrate in the food to transform the starch into maltose. Other serous glands on the tongue’s surface encircle taste buds on the back side of the tongue in the mouth & these also produce lingual lipase. The Lipase enzyme is a digestive enzyme that catalyzes the hydrolysis of lipids. Sensory information can activate the secretion of saliva providing the necessary fluid for the tongue to work with & also to ease the swallowing of food.
Saliva
Saliva provides moisture & softness to the food, along with the chewing action of the teeth, transforming the food into a smooth bolus. it’s helped by the lubrication given by the saliva in the passage from the mouth into the esophagus. there is present in the saliva of digestive enzymes such as amylase & lipase. Amylase starts to work on the starch in carbohydrates, breakdown into the simple sugars of maltose & dextrose that can be further broken down in the small intestine. The saliva can account for 30% of this initial starch metabolism. Lipase starts to work on the breakdown of fats. Lipase enzyme is further produced in the pancreas for the digestion of fats.
It also has an immunologically important role in supplying antibodies to the system, such as immunoglobulin A. This prevents infections of the salivary glands, and importantly parotitis.
Saliva also contains a glycoprotein known as haptocorrin which is a binding protein to vitamin B12. It binds with the vitamin to carry it safely via the acidic content of the stomach. When it reaches the duodenum, pancreatic enzymes break down the glycoprotein & free the vitamin which then binds with intrinsic factors.
Taste
Taste is a form of chemoreceptors that takes place in the specialized taste receptors, contained in structures known as taste buds in the mouth.
Taste buds are mainly on the dorsum surface of the tongue.
The function: taste perception is vital to help prevent harmful foods from being consumed. There are taste buds on the epiglottis & upper part of the esophagus. The taste buds are innervated by a branch of the 7th cranial nerve the chorda tympani, & the glossopharyngeal nerve. The brain can differentiate between the chemical qualities of food. The five basic tastes are called saltiness, sourness, bitterness, sweetness, & umami.
The detection of saltiness & sourness enables the control of salt & acid balance. The detection of bitterness warns of poisons & many of a plant’s defenses are of poisonous compounds that are bitter. Sweetness guides those foods that will give energy & the initial breakdown of the energy-giving carbohydrates by salivary amylase create the taste of sweetness since simple sugars are the first result. umami is thought to signal protein-rich food. Sour tastes are acidic compounds that are often found in bad food.
The brain has to decide quickly whether the food should be eaten or not.
It was the find in 1991, describing the first olfactory receptors that help in to prompt the research into taste. The olfactory receptors are located at cell surfaces in the nose which bind to chemicals enabling the detection of smells. It is assumed that signals from all taste receptors work together with those from the nose, to make an idea of complex food flavors.
Teeth
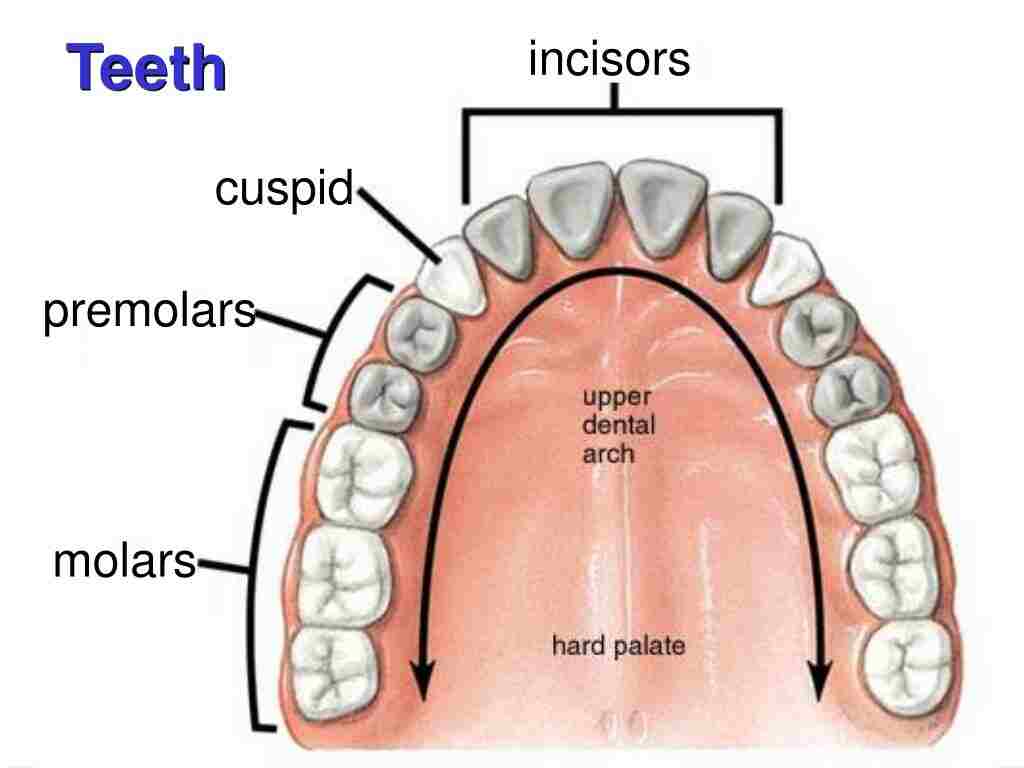
Human Teeth are complex structures made of materials specific to them. They are made of a bone-like material known as dentin, which is covered by the hardest tissue in the body called enamel. human teeth have different shapes to deal with different aspects of mastication employed in tearing & chewing pieces of food into smaller and smaller pieces. The teeth are named after their particular function in the process of mastication:
1) incisors: These are used for cutting or biting off pieces of food;
2) canines: These are used for tearing,
3) premolars & molars: it is used for chewing & grinding.
Mastication of the food with the help of saliva & mucus secretion results in the formation of a soft bolus which can then be swallowed to make its way down to the upper gastrointestinal tract to the stomach. The digestive enzymes in saliva also help in keeping the teeth clean by breakdown any lodged food particles.
Pharynx
The oral cavity leads into the next part of the digestive system known as the pharynx. It is a common passage for food & air for breathing. The region of the pharynx is classified into three regions:
1) Nasopharynx: This region of the pharynx is present at the junction of the nasal chamber.
2) Oropharynx/Glossopharynx: This region of the pharynx is present at the junction of the epiglottis.
3) Laryngopharynx/ Hypopharynx: This region of the pharynx is present at the junction of the larynx.
Esophagus
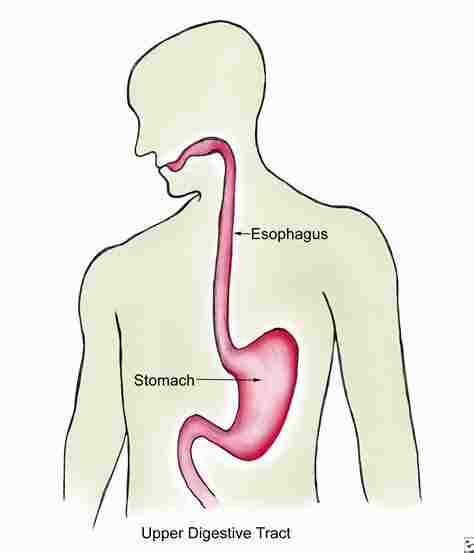
It is commonly known as the food pipe. it is made up of a muscular tube through which food passes from the pharynx and then into the stomach. The esophagus is then continuous with the laryngopharynx. It passes through the posterior mediastinum in the thorax & then enters the stomach via a hole in the thoracic diaphragm—the esophageal hiatus, at the level of the 10th thoracic vertebra (T10). Its length averages 25 centimeters, varying with an individual’s height. The pharynx joins to the esophagus at the esophageal inlet which is behind the cricoid cartilage.
The esophagus has closed at both ends, by the upper & lower esophageal sphincters. The opening of the upper sphincter has triggered by the swallowing reflex so that food is allowed through. The sphincter also serves to prevent the backflow of food from the esophagus into the pharynx. During swallowing, food is transferred from the mouth through the pharynx into the esophagus. The epiglottis folds down to a more horizontal position to direct the food into the esophagus & away from the trachea.
Once in the esophagus, the bolus goes down to the stomach via rhythmic contraction & relaxation of muscles called peristalsis. The lower esophageal sphincter is a muscular sphincter located at the lower part of the esophagus. The gastroesophageal junction between the esophagus & the stomach is controlled by the lower esophageal sphincter, which remains always constricted other than during swallowing & vomiting to prevent the contents of the stomach which entering into the esophagus.
Diaphragm
It is the most important part of the body’s digestive system & the respiration system. The diaphragm muscle divides the thoracic cavity from the abdominal cavity where most of the digestive organs are lies. The suspensory muscle attaches the ascending duodenum & then the diaphragm muscle.
Stomach
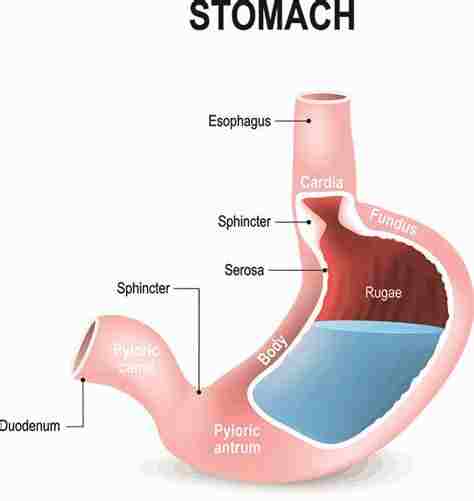
It is a major organ of the gastrointestinal tract & human digestive system. It is a J-shaped organ joined to the esophagus at its upper end & to the duodenum at its lower end. Gastric juice produced in the stomach plays a vital role in the digestive process, & mainly contains hydrochloric acid (HCL) and sodium chloride(NaCl). A peptide hormone, gastrin, produced by the G cells in the gastric glands, stimulates the production of gastric juice which activates the digestive enzymes. Pepsinogen is a precursor enzyme produced by the gastric chief cells, & gastric acid activates this to the enzyme pepsin which starts the digestion of proteins.
As these two chemicals would damage the wall of the stomach. the mucus is secreted by gastric glands in the stomach, to provide a slimy protective layer against the damaging effects of acidic chemicals on the inner layers of the stomach.
At the same time that protein is being digested, mechanical churning occurs via the action of peristalsis, waves of muscular contractions that move along the stomach wall. Gastric lipase is secreted by the main cells of the fundic glands in the gastric mucosa of the stomach. it is an acidic lipase. in contrast with the alkaline pancreatic lipase enzyme.
The pylorus is the lowest part of the stomach which attaches to the duodenum via the pyloric canal & contains countless glands which secrete digestive enzymes including gastrin. After one hour or two, a thick semi-liquid known as chyme is produced.
When the pyloric sphincter, or valve opens, chyme enters into the duodenum where it mixes further with digestive enzymes from the pancreas & then passes through the small intestine, where digestion continues.
The parietal cells found in the fundus of the stomach produce a glycoprotein known as an intrinsic factor which is essential for the absorption of vitamin B12. Vitamin B12 is carried to & through the stomach bound to a glycoprotein secreted by the salivary glands – transcobalamin I have also known as haptocorrin, which also protects the acid-sensitive vitamin from the acidic stomach contents. The freed vitamin B12 then binds with the intrinsic factor which is then absorbed by the enterocytes in the ileum.
it is a distensible organ & can normally expand to hold about 1 liter of food. This expansion occurred through a series of gastric folds in the inner walls of the stomach. The stomach of a newborn baby will only be able to expand to retain only about 30 ml.
Spleen
It is the largest lymphoid organ in the human body but has other functions. Its main function is to break down both red & white blood cells that are spent. This is why it is sometimes called the ‘graveyard of red blood cells’. A product of this digestion system is the pigment bilirubin which is sent to the liver & released in the bile. Another product is iron, which is used in the forming of new blood cells in the bone marrow
Liver
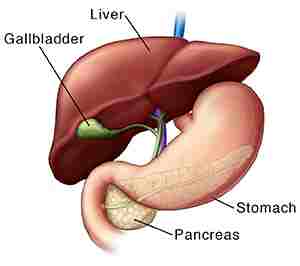
It is the second largest organ (after the skin) & is an accessory digestive gland that plays a role in the body’s metabolism. The liver has so many functions some of which are important to the digestion process. The liver can detoxify various metabolites; synthesize proteins & produce biochemicals needed for the digestion process. It also helps in regulates the storage of glycogen which can form from glucose. The liver can also play role in synthesizing glucose from certain amino acids. Its digestive functions are largely involved with the breakdown of carbohydrates. It also maintains protein metabolism in its synthesis & degradation. In lipid metabolism, it synthesizes cholesterol & lipoproteins. Fat molecules are also produced in the process of lipogenesis. It is situated in the upper right quadrant of the abdomen & below the diaphragm muscle to which it is attached at one part, the bare area of the liver. This is to the right of the stomach & it overlies the gallbladder. The liver synthesizes biles & lecithin to promote the digestion of fat.
Bile
This is produced by the liver and is made up of 97 % water, bile salts, mucus & pigments, and 1% fats & inorganic salts. Bilirubin is its major pigment. its function is to lower the surface tension between either two liquids or a solid & a liquid & it also helps to emulsify the fats in the chyme. Food fat is dispersed by the action of bile into smaller particles known as micelles. The breakdown into micelles makes a much larger surface area for the pancreatic enzyme, lipase enzyme to work on.
Lipase enzyme digests the triglycerides which are further broken down into two fatty acids & a monoglyceride. These are then absorbed by villi which are present in the intestinal walls. It helps in the absorption of Vit K. It is collected & delivered via the common hepatic duct. This duct joins with the cystic duct to connect to the common bile duct with the gallbladder. it is stored in the gallbladder for release when food is discharged into the duodenum & also after a few hours.
Gallbladder
This organ is a hollow part of the biliary tract that is situated just beneath the liver, with the body of the gallbladder resting in a small depression. the gallbladder is a small organ where the bile produced by the liver is stored, before being released into the small intestine. Bile flows from the liver via the bile ducts & goes into the gall bladder for storage. The bile is released in response to CCK a peptide hormone released from the duodenum. The production of cholecystokinin is stimulated by the presence of fat in the duodenum.
It is divided into three parts:
1) fundus
2) body
3) neck.
The neck tapers and connects to the biliary tract through the cystic duct, which then joins the common hepatic duct to form the common bile duct. At this junction is a mucosal fold known as Hartmann’s pouch, where gallstones get stuck. The muscular layer of the body of the gallbladder is made up of smooth muscle tissue that helps the gallbladder contract so that it can discharge its bile into the bile duct. it needs to preserve the bile in a natural, semi-liquid form at all times. To dilute the bile, water & electrolytes from the digestion system are added.
Also, salts attach themselves to cholesterol molecules in the bile to keep them from crystallizing. If there is too much cholesterol or bilirubin in the bile, or if the gallbladder doesn’t empty properly the system can fail. This is how gallstones form when a small piece of calcium gets coated with either cholesterol or bilirubin & the bile crystallizes and make a gallstone. The main function of the gallbladder is to store & release bile, or gall. Bile is released into the small intestine to help in the digestion of fats by breaking down larger molecules into smaller particles. After the fat is absorbed, the bile is also absorbed & transported back to the liver for reuse of bile.
Pancreas
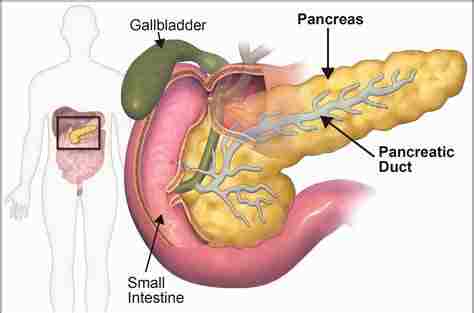
It is a primary organ functioning as an accessory digestive gland in the digestive system. the pancreas has both an endocrine gland & an exocrine gland. The endocrine part secretes insulin when the sugar in the blood becomes high; insulin moves glucose from the blood into the muscles & other tissues for use as energy. The endocrine part releases glucagon when sugar in the blood is low; glucagon allows stored sugar to be broken down into glucose by the liver to re-balance the sugar levels. The pancreas produces & secretes important digestive enzymes in the pancreatic juice that it delivers to the duodenum. it is located below & at the back of the stomach. It connects to the duodenum through the pancreatic duct, which joins near the bile duct’s connection where both the bile & pancreatic juice can act on the chyme released from the stomach and go into the duodenum. Aqueous pancreatic secretions from pancreatic duct cells contain bicarbonate ions which are alkaline & they help with the bile to neutralize the acidic chyme that is churned out by the stomach.
it also has the main source of enzymes for the digestion of fats & proteins. Some of these are released in response to the production of cholecystokinin in the duodenum. The cells are filled with secretory granules & these cells contain the precursor digestive enzymes. The proteases & the pancreatic enzymes which work on proteins are trypsinogen & chymotrypsinogen. Elastase is also produced. lipase & amylase are secreted in small amounts. it also secretes phospholipase A2, lysophospholipase, & cholesterol esterase.
Lower gastrointestinal tract
It includes the small intestine & large intestine. The intestine is also known as the bowel or the gut. The lower GI begins at the pyloric sphincter of the stomach & ends at the anus. The small intestine is further classified into the duodenum, the jejunum & the ileum. The cecum is the division between the small & large intestines. it includes the rectum and anal canal.
Small intestine
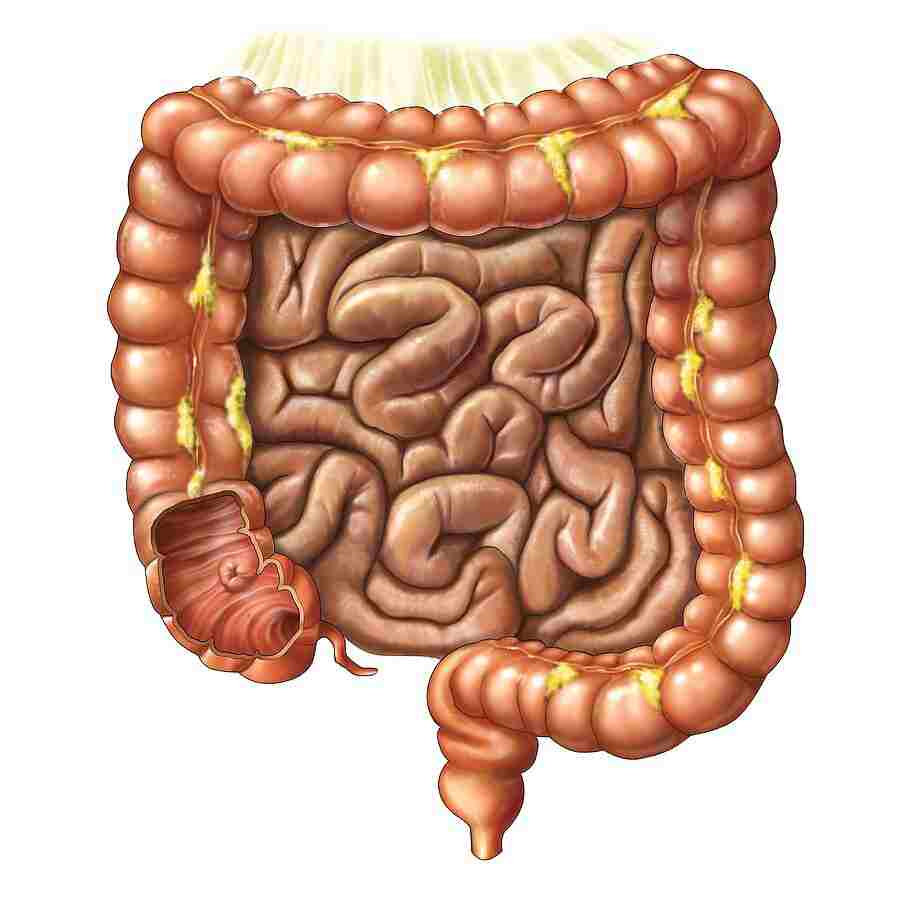
Partially digested food begins to arrive in the small intestine as semi-liquid chyme, one hour after it is eaten[citation required]. The stomach is half empty after an average of 1.2 hours of food is eaten. After four or five hours the stomach has fully emptied.
In the small intestine, the pH becomes crucial; it requires to be finely balanced to activate digestive enzymes. The chyme is very acidic in PH, with a low pH, having been released from the stomach & requires to be made much more alkaline. This is achieved in the duodenum by the addition of bile from the gall bladder combined with the bicarbonate secretions from the pancreatic duct cells & also from secretions of bicarbonate-rich mucus from duodenal glands called Brunner’s glands. The chyme reaches the intestines having been released from the stomach via the opening of the pyloric sphincter. The resulting alkaline fluid mix neutralizes the gastric acid which would damage the lining of the small intestine. The mucus component lubricates the walls of the small intestine.
Parts of Small Intestine: It is a tubular structure that is 7 meters long & 2.5 centimeters wide. it is coiled & folded in the abdomen & has the following three parts, namely:
Duodenum
Jejunum
Ileum
Duodenum – it is 25 cm long
The duodenum is the shortest upper part of the small intestine. duodenum begins after the pyloric end of the stomach. It is a ‘U’ shaped & receives the semi-digested food called here ‘chyme’ from the stomach.
Jejunum – (2.5 m long)
the jejunum is a 2 meters long-coiled tube that is the middle part of the small intestine. Primarily absorption occurs here.
Ileum – (3.5 m long)
the ileum is a 3.5 m long coiled tube. It is the lower part of the small intestine where both digestion and absorption occur& complete digestion of food takes place.
Functions of Small Intestine
Digestion & absorption both occur here.
Simpler forms of food like glucose, amino acids, etc., are absorbed in the small intestine as it has numerous finger-like projections known as villi.
These projections increase the surface area of the small intestine so that more nutrients can be absorbed.
The villi are provided with some blood vessels & lymphatic vessels. These lymphatic vessels are called lacteals.
Cecum
it is a pouch marking the division between the small intestine & the large intestine. It is located below the ileocecal valve in the lower right quadrant of the abdomen. it receives chyme from the last part of the small intestine, the ileum, and joins to the ascending colon of the large intestine. the ileocecal valve which slows the passage of chyme from the ileum allowing further digestion process. the cecum is also the site of the appendix attachment.
Large intestine
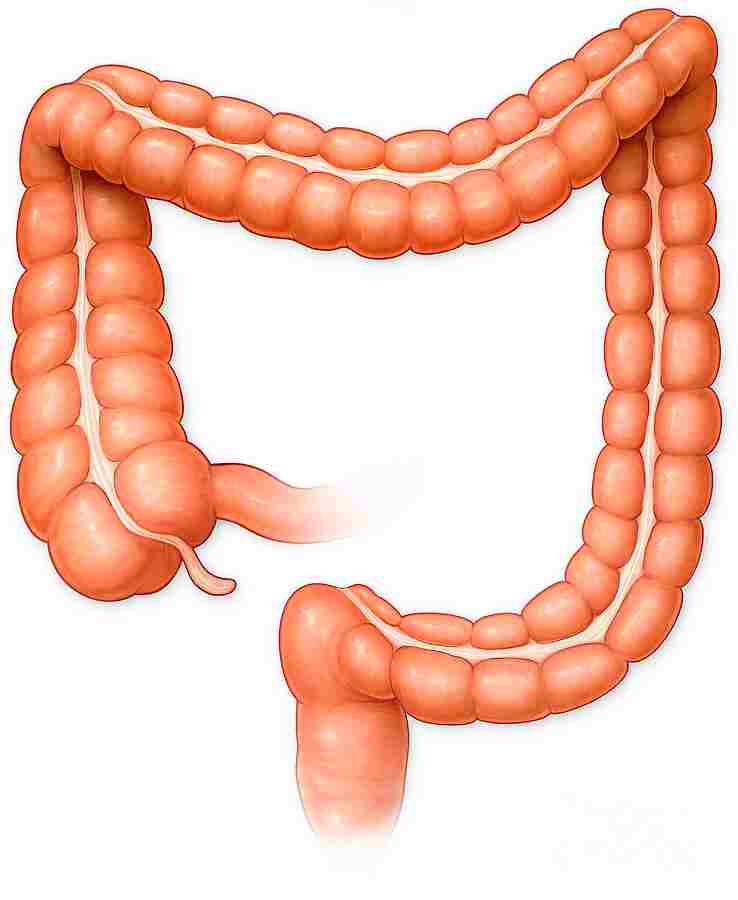
It is the passage of the digesting food in the colon is a lot slower, taking from 30 to 40 hours until it is removed by defecation. it mainly serves as a site for the fermentation of digestible matter by the gut flora. The remaining semi-solid waste is termed in feces & is exudate by the coordinated contractions of the intestinal walls, termed peristalsis, which propels the excreta forward to reach the rectum & exit through defecation from the anus. The wall has an outer layer of longitudinal muscles, the taeniae coli, & an inner layer of circular muscles. The circular muscle keeps the material moving forward side & also prevents any back flow of waste. it Also helps in the action of peristalsis is the basal electrical rhythm that determines the frequency of contractions. Most parts of the gastrointestinal tract are covered with serous membranes & have a mesentery.
Blood supply
Arteries & veins around the pancreas and spleen
The human digestive system is supplied by the celiac artery. It is the first major branch of the abdominal aorta, & is the only major artery that helps in nourishing the digestive organs.
There are three main divisions –
1) the left gastric artery
2) the common hepatic artery
3) the splenic artery.
The celiac artery supplies the liver, stomach, spleen & the upper 1/3 of the duodenum & the pancreas with oxygenated blood. Most of the blood is returned to the liver through the portal venous system for further processing & detoxification before returning to systemic circulation via the hepatic veins.
The branch of the abdominal aorta is the superior mesenteric artery. the superior mesenteric artery supplies the area of the digestive tract derived from the midgut, which includes the distal 2/3 of the duodenum, jejunum, ileum, cecum, appendix, ascending colon & transverse colon.
The last branch which is important for the digestive system is called the inferior mesenteric artery. it supplies the regions of the digestive tract derived from the hindgut, which includes the distal 1/3 of the transverse colon, descending colon, sigmoid colon, rectum, & the anus above the pectinate line.
Blood flow to the human digestive tract reaches its maximum of 20–40 minutes after a meal & lasts for 1.5–2 hours.
Nerve supply
The enteric nervous system consists of some 100 million neurons which are embedded in the peritoneum the lining of the GI tract extending from the esophagus to the anus.
These neurons are collected into two plexuses:
1) the myenteric plexus that is located between the longitudinal & the smooth muscle layers.
2) the submucosal plexus that lies between the circular smooth muscle layer & the mucosa.
Parasympathetic innervation to the ascending colon is supplied by the vagus nerve & Sympathetic innervation is supplied by the splanchnic nerves that join the celiac ganglia.
Mainly the digestive tract is innervated by the 2 large celiac ganglia, with the upper part of each ganglion connected by the greater splanchnic nerve & the lower parts connect by the lesser splanchnic nerve.
FAQ
The human digestive system is essentially a very long tube that extends from the back of the mouth to the anus. When we eat, food passes down into the esophagus to the stomach, squeezed by regular contractions .this is known as peristalsis.
Food is pushed through the lumen throughout the digestive system by muscles, & that process is known as peristalsis. When you chew food & then you swallow, these are the structures in your body that the food goes through during its journey goes down to the anus. Mouth: where the food breakdown begins with chewing & the mixing of food with saliva.
The digestive system is made up of the digestive tract & other organs that help the body break down & absorb food. Your digestive tract is a long, twisting tube that starts from your mouth, & then involves your esophagus, stomach, small intestine, large intestine & anus.
The stomach produces several digestive juices & enzymes that mix with food. then, the stomach’s strong muscles act like a blender to turn food into a usable form. Carbohydrates, for example, break down food the fastest.
The stomach contains hydrochloric acid(HCL) & digestive enzymes that continue the digestion process of food that began in the mouth. Enzymes & acids mix with the food that has already begun to break down in the mouth & esophagus, and it turns into a liquid known as “chyme’.


40 Comments