Bankart Lesion
Table of Contents
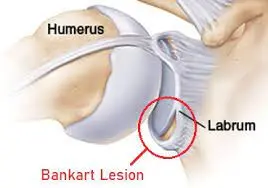
What is Bankart lesion?
Bankart lesions are injuries of the anteroinferior part of the glenoid labral complex and are often seen in connection with a Hill-Sachs lesion. This injury is an ordinary complication of anterior shoulder dislocation and/or repeated anterior shoulder subluxations. The connective tissue band close to the glenoid labrum in the shoulder joint may be harmed by the anterior joint dislocation. It can also lead to damage to the connection between the labrum and capsule. Usually, it is associated with poor construction of the medial glenohumeral ligament on the medial side. This injury is standard for athletes practicing volleyball, tennis, and handball, and those all doing overhead activities.
The glenoid labrum is a structure encircling a joint and is a fibrocartilaginous ring related circumferentially to the glenoid rim donating to the strength of the shoulder joint. The glenoid labrum expands the glenoid surface vertically by 75% and horizontally by 57%. Bankart’s lesion represents an anterior and inferior labral separation from the glenoid with an associated capsuloligamentous injury below the equator of the glenoid.
This consequence in anterior instability of the shoulder joint is due to the loss of the subsequent standard mechanisms, such as the Choke block development of the labrum, the concavity compression mechanism of the rotator cuff in the shoulder, and the function of the inferior glenohumeral ligament. Traumatic subluxations or shoulder joint dislocation causes injury to the glenoid labrum. Almost 87-100% of the index anterior shoulder dislocations are connected with Bankart lesions.
Pathology:
Bankart lesions occur when the humerus is squeezed against the labrum as occurs in anterior shoulder dislocations or subluxations. There is the separation of the anteroinferior labrum from the underlying glenoid cavity. Impaction fracture of the anteroinferior glenoid margin repeatedly occurs simultaneously
There are two types of Bankart lesions:
- Soft-bankart lesion: The glenoid labrum rips from the glenoid, and the injury affects only the soft tissue. It is the most common lesion.
- Bony Bankart lesion: The glenoid labrum gets torn and a part of the bony glenoid fractures or splits off. This may lead to considerable bone loss in the glenoid, which is a cause of chronic instability.
Patients with anterior dislocation of the shoulder may have a Bankart lesion in many cases. A reverse Bankart lesion may occur in case of a posterior shoulder dislocation.
Causes of Bankart Lesion:
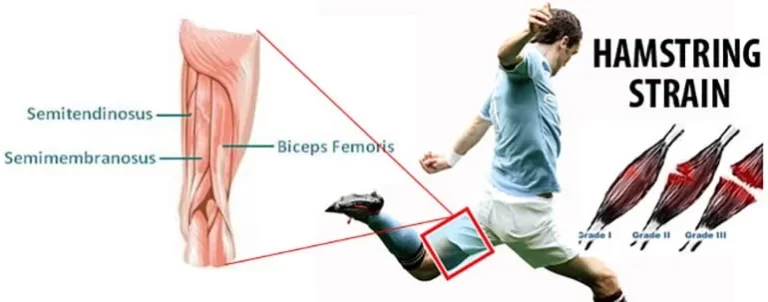
The exact mechanisms that can cause a shoulder dislocation are among the reasons leading to the Bankart lesion. Bankart lesion is a specific sports injury among all athletes who are playing games like volleyball, football, handball, basketball, tennis, wrestling, etc. It is common among people who do repeated overhead movements, like construction workers. Collisions and accidents can even cause Bankart lesions. Another cause of Bankart lesions is trauma, which causes violent movement of the shoulder. Though any person can cause this injury, it generally occurs in elderly people, particularly women, over 60, due to falls, and young men in their twenties. Bankart lesions are frequently caused by a shoulder dislocation, either partial or complete.
Bankart lesions occur from high-force trauma and sports injuries (either acute injuries or overuse injuries from repetitive arm movements).
Possible causes of shoulder dislocations and lesions:
- Car accidents: An impulsive blow to the shoulder can knock the humerus ball from its socket, tearing the labrum.
- Sports collisions: Smashing into another person with speed and force. For example, while playing football or hockey tackle, can push the shoulder out of alignment or drag the arm forward or backwards, leading to shoulder dislocations.
- Falls from sports: Falling and landing on another person’s shoulder can direct to shoulder dislocations in athletes, particularly in sports where falling with height or speed is expected, like gymnastics, skating, rollerblading, or skiing. Sliding into bases during softball or baseball can also damage the shoulder.
- Falls do not result from sports: Falling from a ladder or slipping on a crack in the sidewalk can produce sufficient power to dislocate the shoulder.
- Overuse injuries: In some athletes, overuse of the shoulder can direct in loose ligaments and instability. Athletes including Swimmers, Tennis players, Volleyball players, baseball pitchers, gymnasts, and weight lifters are predisposed to this problem. Additionally, even if a person is not athletic, repeated arm movements aloft can cause instability. (for example, swinging a hammer).
- Loose ligaments: Some people are genetically predisposed to lose ligaments throughout the body (e.g., double-jointed individuals). They may notice that their shoulders can pop out of normal alignment easily. Treatment for patients is often more
Signs and Symptoms of Bankart Lesion:
This type of labrum tear shows many symptoms with other shoulder injuries. A complete physical examination is necessary to properly diagnose the underlying condition of the shoulder. Moderate to severe shoulder pain. Weakness and instability of the shoulder. Popping and clicking sensations feel when the shoulder is pushed. There is a loss of range of motion(ROM) in the shoulder. Repeated episodes of shoulder dislocation.
Symptoms of a lesion can include:
Pain: When reaching the hand overhead, at night, or with daily activities pain occurs. Pain that does not ease with rest, or by doing a change in activity, OTC medications, or ice, warrants consultation with the doctor.
Instability and weakness: The shoulder may feel ‘loose’. Patients may report apprehension about moving the shoulder into particular positions away from the body. Low-energy movements like rolling around in bed or fastening a seat belt in a vehicle can also be used by patients to detect recurrent instability, subluxation, or dislocation.
Limited range of motion: Due to the pain patient may have limited movement in the shoulder. Discussing a range of motion, moving the shoulder itself may be difficult. There is a limited range of motion. While moving the shoulder in any direction, triggering pain is a sign of a Bankart lesion.
Atypical sounds or feelings in the shoulder joint: A Bankart lesion may cause a popping, grinding, or catching feeling with shoulder subluxation.
Mechanical symptoms: Grinding, catching (not moving fluidly), locking in place, or popping may all be symptoms of torn connective tissue getting caught in the joint.
Diagnosis:
Diagnosis starts with the evaluation of the past medical history of the patient. Physical examination feeds a good clinical indication for a Bankart lesion. One or more of the following techniques are used by an orthopaedic or shoulder joint expert to evaluate a bankart injury:
Physical Examination:
- X-rays
- MRI
- Arthroscopy
- MR arthrography
Radiographs (particularly for bony bankart lesions)
Radiographs – It is required to obtain plain radiographs as part of the initial workup to lead out associated fractures and frank osseous defects such as bony Bankart, Hill-Sachs, glenoid fractures, coracoid fractures, and greater tuberosity fractures.
X-ray views :
- Anteroposterior view (AP view)
- True AP view
- Axillary view
- Scapular Y view
- Acromial outlet view
Special views:
- West point axillary view- Bony Bankart’s lesion
- Stryker’s notch view – Hill-Sachs lesion
Magnetic Resonance Imaging (MRI):
MRI with or without contrast is the gold standard examination for finding soft tissue injuries such as glenoid labrum and capsuloligamentous injury. It also assists in scheduling the management of shoulder instability. MRI results show Hemorrhagic effusion and Capsulolabral elevation from the anterior and inferior glenoid rim in an acute Bankart injury. MRI in the abduction and External rotation has enhanced sensitivity (94%) and specificity (82%) for detecting Bankart lesions than the traditional neutral position. Presence of associated lesions such as Perthe’s disease, Anterior Labral Periosteal Sleeve Avulsion (ALPSA), Gleno-Labral Articular Disruption (GLAD), and Superior Labral tear from Anterior to Posterior (SLAP), and Humeral Avulsion of Glenohumeral Ligament (HAGL) can be interpreted on MRI.
An MR-arthrogram is more specific and sensitive than MRI for seeing labral tears. The specificity is 96% and the sensitivity is 93%.
NCCT: The glenoid bone loss, the orientation of the articular surface, the humeral bone loss, and the glenoid cavity can all be quantified using non-contrast computed tomography (NCCT) with 3D modelling.
Following are the manifestation of NCCT with 3D reconstruction:
Mid-range instability on clinical examination.
- Glenoid bone loss suspicion on the radiograph.
- Large Hill-Sachs.
- A very large number of shoulder dislocations.
- Identification of “On Track” and “Off Track” Hill-Sachs lesions in the shoulder joint
Examination:
Clinical analysis is committed to interpreting the presence of shoulder instability and associated injuries.
Signs of Anterior Instability:
- Apprehension test
- Jobe’s relocation test
- Anterior drawer test
- Bony apprehension test
Signs of Posterior Instability:
- Posterior apprehension
- Jerk test
- Porcellini test
- Kim test
Signs of Mid-range Instability
- Sulcus sign rules out multidirectional instability.
- Generalized Ligamentous Laxity
Treatment of Bankart Lesion:
Nonsurgical Treatment:
Rest and anti-inflammatory medicines are usually the first lines of treatment. A doctor may be given steroid medicine shots (injections). Physical therapy may also be recommended to strengthen the muscles and stabilize the shoulder joint. If these treatments aren’t adequate, the doctor may recommend surgery to repair the labrum.
Surgical Treatment:
Indications for operative management:-
- Young athletes aged less than 30 years with acute, primary, and traumatic anterior shoulder dislocations who desire to continue playing sports are the best candidates for surgical intervention. Other indications are as follows:-
- Post-traumatic recurrent shoulder instability which limits all daily activities
- Post-traumatic anterior shoulder dislocation an associated with a large Rotator cuff tear, a Bony defect in the glenoid cavity or the humerus head (Hill Sachs lesion).
- Persistent subluxation or dislocation and pain even after sufficient nonoperative management.
- Patients with a tendency for recurrent instability include athletes with overhead activities, construction workers, and climbers.
- Relative Contraindications for Operative Management
- Uncooperative/ medically unstable patients
- Seizure condition
- Primary collagen disorders. For E.g., Ehlers-Danlos or Marfan syndrome
- Atraumatic Shoulder instability
- Neurologic damage such as paralysis of the axillary nerve or suprascapular nerve.
- Recurrent instability with post-traumatic arthritis
Dependence of surgery:
Surgery depends on the patient’s expectations, age, and level of sport played (contact vs. non-contact). These are the most important factors to consider when treating a labral injury. Young patients who play contact sports (high demand) will be given surgical consideration.. In all of these cases, the glenoid bone loss and engaging (off track) or non-engaging (on track) Hill Sachs lesions are taken into account.
Isolated arthroscopic or open Bankart’s repair with suture anchors will be adequate if the glenoid bone loss is less than 13.5%. This non-significant bone loss will not confront in almost all cases. When glenoid bone loss ranges from 13.5% to 17.3%, it is considered subcritical. High-risk patients, such as young athletes who participate in contact sports and those who have an active Hill-Sachs lesion, will receive arthroscopic or open Bankart’s surgery with remplissage.
When glenoid bone loss is 13.5% to 17.3% with a descending risk of recurrence and is non-engaging, Hill Sachs patients are treated by lone arthroscopic or open Bankart’s repair. Patients with 17.4% to 30% of glenoid bone loss will require an open latarjet procedure. About 30% or more, glenoid bone loss requires glenoid bone grafting (autograft- iliac crest or allograft-distal tibia
BANKART LESION REPAIR (SURGERY):
If the shoulder persists to dislocate or feels unstable, then visit a doctor for another evaluation. The doctor may use X-rays, an MRI, and/or a thorough physical exam to help make a diagnosis.
Depending on the cause and severity of the shoulder instability, the doctor may prescribe an exercise program and/or surgery to stabilize the shoulder joint.
- Shoulder arthroscopy:
Most frequently, minimally invasive procedures can be used to repair the labrum. The doctor can use a scope and small surgical tools to find and examine the tear, remove damaged fragments, and repair them. The doctor will place anchors in the bone near the tear in joint. Sutures connected to these anchors are drawn tight, reattaching the torn piece of the labrum to the bone.
- Open surgery:
In some cases, doctors may choose to use open surgery for this method. Which method the doctor selects relies on variables like the type and location of the injury, the condition of the tissue, and how much additional damage the person may have sustained.
If an individual is healthy, the perspective for shoulder surgery of this kind is typically good, with most patients continuing gentle movement and non-contact sports within 6–12 weeks. Most patients will need to avoid heavy objects lifting and contact sports for at least 3 months while they undergo physical therapy to regain strength and range of motion in the shoulder.
Physical Therapy:
An arthroscopic Bankart repair, an open Bankart repair, or conservative treatment are all interventions.
Muscle power recovers more quickly after arthroscopic Bankart repair than after open Bankart repair, but the number of repetitions is much lower.
The recurrence rate after operative Bankart treatment is considerably reduced compared to non-operative treatment. After surgery, there is off-course rehabilitation needed, which can be slightly similar to the non-operative rehabilitation program.
The focus of the rehabilitation program is on maximizing dynamic stability, scapular positioning, proprioception, and enhancing neuromuscular control, as there are no specific exercises to improve labrum quality. After surgery, protected mobility is prioritised for the first six weeks. The focus of the second six weeks is on muscle-strengthening exercises to safeguard the shoulder as it must resume regular activities. Usually, the rehabilitation schedule is divided into 4 phases. The programs for non-operative treatment and postoperative rehabilitation are similar.
Phase 1( 1-6 weeks): Phase 1 consists of sling immobilization with a limited active range of motion for 0 to 4 weeks, this allows 20 degrees of abduction and 40 degrees of internal rotation. This provides an earlier recovery to functional activity. Immobilization in external rotation lessens the risk of recurrent shoulder dislocations. After 14 days, passive movement is started in a pain-free zone. Strengthening Exercises are started as isometric contractions to initiate muscle recruitment of the rotator cuff muscles, mostly Closed Chain Exercises, such as pushing the underarm against a wall towards external rotation. The purposes are to diminish pain and protect healing soft tissues.
Stabilisation exercise
Phase 2, (6 to 12 weeks): Progressive passive motion is important, together with an active-assisted range of motion exercises. Strengthening of Rotator cuff muscles is begun in balanced exercises. Examples of exercises include movements of the shoulder joint conducted with elastic bands or dumbbells as dynamic open-chain strengthening exercises. Rehabilitation includes both closed and open-chain exercises. An example of a closed kinetic chain exercise is a Quadruped position with scapula protraction, progressing to a tripod position. A patient can continue to phase 3 when a normal passive range of motion is accomplished.
Phase 3, (12 weeks to 4 months): Strengthening exercises which are also done in anterior shoulder instability.
Shoulder medial and lateral rotation
Phase 4( 4 to 6 months): Fully unrestrained movements focused on the rehabilitation of a full active range of motion. In this stage, progressively extending resistance in dynamic exercises is highlighted to regain full strength for ADL activities. Most important in this phase is the return to full active activity of normal life.
There are 7 essential factors that must be considered in the rehabilitation of an unstable shoulder. These are:
- The onset of the pathology (traumatic, chronic)
- Degree of instability
- Frequency of dislocation
- The direction of instability (anterior, posterior, multidirectional)
- Concomitant pathologies
- End-range neuromuscular control
- Premorbid activity level
FAQs:
Do Bankart lesions need surgery?
The most frequent treatment for a Bankart lesion is the orthopaedic reduction of the dislocation and surgical repair, with suturing to stable the labrum when the extent of the tear is important. However, the repair can result in the limit of normal functional activities of the shoulder.
How serious is a Bankart lesion?
A Bankart lesion that is not treated can lead to chronic shoulder instability, which means that the shoulder may dislocate again in the future, presumably with less force than when it was first hurt.
How long is Bankart surgery recovery?
It is usually calculated that it will take at least 4-6 months to feel as though you have completely regained the use of the arm. In some cases may take a long time 9-12 months to make a full recovery. People with computer jobs should plan to take at least 1 week off from work.
Is Bankart repair painful?
In comparison to open surgery, arthroscopic Bankart repair causes the least amount of discomfort and trauma, as well as less scarring and damage to the surrounding tissue. There is also a briefer recovery period and a shorter length of rehabilitation than with traditional open surgery.
Can Bankart tear heal on its own?
Bankart lesions will often recover on their own, but they may not heal in the right position without intervention. In many instances, especially in younger patients who plan to continue being active, surgery will be necessary to reconnect the torn labrum to the shoulder socket.

One Comment