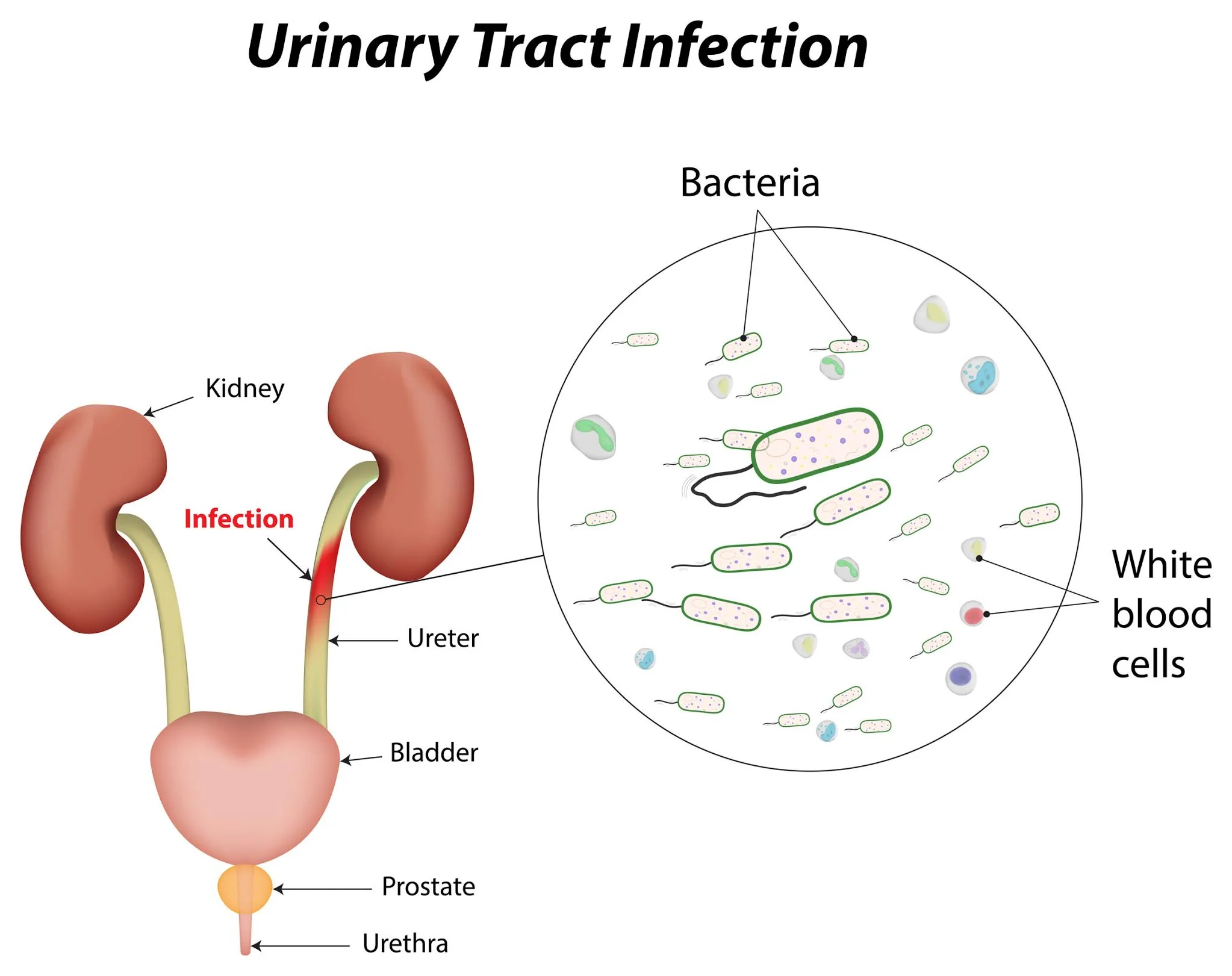
Urinary Tract Infection
- A urinary tract infection (UTI) is a very usual type of infection in your urinary system. A urinary tract infection (UTI) can involve any part of your urinary system, including the urethra, ureters, bladder, and kidneys. Symptoms typically involve needing to urinate often, having pain when urinating, and feeling pain in your side or lower back. Most urinary tract infections (UTIs) can be cured with an antibiotic.
- A urinary tract infection (UTI) is an infection from microbes (microorganisms). These are organisms that are too tiny to be seen without a microscope.
- Most urinary tract infections (UTIs) are caused by bacteria, but some are caused by fungi and, in rare cases, by viruses. urinary tract infections (UTIs) are among the most common infections in humans.
Table of Contents
What is a Urinary tract infection (UTI)?
- A urinary tract infection (UTI) is a disease of the urinary system (US). This type of infection can include your urethra (a condition called urethritis), kidneys (a condition called pyelonephritis), or bladder, (a condition called cystitis).
- Your urine typically does not contain bacteria (germs). Urine is an outgrowth of our filtration system—the kidneys. When waste products and excess water is separated from your blood by the kidneys, urine is made. Commonly, the urine goes through your urinary system without any contamination. However, bacteria can acquire into the urinary system (US) from outside of the body, causing problems such as infection and inflammation. These are urinary tract infections (UTIs).
What is the urinary tract?
Your urinary tract is created up of your:
- kidneys
- ureters
- bladder
- urethra.
Most urinary tract infections (UTIs) only involve the urethra and bladder, in the lower tract. But urinary tract infections (UTIs) can involve the ureters and kidneys, in the upper tract. Although upper tract urinary tract infections (UTIs) are rarer than lower tract UTIs, they’re also usually more severe.
The urinary tract stores urine, from the body’s liquid waste products. The urinary tract involves the following parts:
- Kidneys: These tiny organs are located on the back of your body, just above the hips. They are the filters of your body — removing excess water from your blood. This excess becomes urine.
- Ureters: The ureters are thin tubes that move urine from the kidneys to your bladder.
- Bladder: A sac-like container, the bladder stores your urine previous it leaves the body.
- Urethra: This tube moves the urine from your bladder to the outside of the body.
How common are urinary tract infections (UTIs)?
- Urinary tract infections are very usual, occurring in 1 out of 5 women sometime in their lifetime. Though Urinary tract infections (UTIs) are common in women, they can also happen to men, older adults, and children. One to 2% of children develop urinary tract infections (UTIs). Each year, eight million to 10 million visits to doctors are for urinary tract infections (UTIs).
Who gets urinary tract infections (UTIs)?
- Anyone can get a urinary tract infection, yet they are more common in women. This causes the urethra (the tube that carries urine out of the body) in females to be shorter and closer to the anus, where E. coli bacteria are common. Older adults are at higher risk for developing cystitis. This improved risk may be caused to incomplete emptying of the bladder. There are several medical conditions that can be related to this, involving an enlarged prostate or a bladder prolapse (a condition where the bladder falls or slips out of its usual position).
- If you get frequent urinary tract infections (UTIs), your healthcare provider may do tests to check for other health issues — such as diabetes or an abnormal urinary system — that may be contributing to your infections. People with sometime Urinary tract infections (UTIs) are occasionally given low-dose antibiotics for a period of time to prevent the infection from coming back. This cautious approach to treating frequent Urinary tract infections (UTIs) is because your body can develop a resistance to the antibiotic and you can get other types of infections, like C. diff colitis. This practice is used very infrequently.
What is the difference between a urinary tract infection (UTI) and a bladder infection (cystitis)?
- A urinary tract infection is a more common type of infection. There are many areas of your urinary tract. Urinary tract infections (UTIs) are a term for an infection that takes place throughout the urinary tract. A bladder infection, also known as cystitis, is a specific infection. In this infection, bacteria make their way into the bladder and cause inflammation.
- Not all urinary tract infections (UTIs) become bladder infections. Preventing the spread of the infection is one of the most important reasons to treat Urinary tract infections (UTIs) quickly when you have symptoms. The infection can spread not only to the bladder but also into your kidneys, which is a more complicated type of infection than Urinary tract infections (UTIs).
What causes a urinary tract infection (UTI)?
- Urinary tract infections (UTIs) are caused by microorganisms — usually bacteria — that enter the urethra and bladder, causing inflammation and infection. Though a Urinary tract infection (UTI) most commonly happens in the urethra and bladder, bacteria can also travel up the ureters and infect your kidneys.
- More than 90% of bladder infection (cystitis) cases are caused by E. coli, a bacterium commonly establish in the intestines.
- Pathogenic bacteria ascend from the perineum, causing urinary tract infections (UTIs).
- Women have shorter urethras than men and therefore are far more susceptible to urinary tract infections (UTIs).
- A major risk factor for urinary tract infections (UTIs) is catheter use. Sexual intercourse and the use of spermicides and diaphragms are risk factors for urinary tract infections (UTIs). Frequent pelvic exams and the presence of anatomical abnormalities of the urinary tract can predispose one to a urinary tract infection (UTI).
- Urinary tract infections (UTIs) are very common after a kidney transplant. The 2 triggers include the use of immunosuppressive drugs and vesicoureteral reflux. Other risk factors involve the use of antibiotics and diabetes mellitus.
Epidemiology
An estimated 150 million urinary tract infections (UTIs) occur every year worldwide, adding to $6 billion in healthcare costs.
- Urinary tract infections (UTIs) are very frequent bacterial infections in women.
- Usually occurring between the ages of 16 and 35 years, with 10% of women getting an infection yearly and more than 40% to 60% having an infection at least once in their lives.
- Recurrences are usual, with nearly half getting a second infection within a year.
- Urinary tract infections (UTIs) occur at least four times more frequently in females than males.
What are the symptoms of urinary tract infections (UTIs)?
A urinary tract infection (UTI) causes the lining of the urinary tract to become red and irritated (inflammation), which may produce some of the following symptoms:
- Pain in the side (flank), abdomen area, or pelvic area,
- Pressure in the below pelvis
- Frequent requirement to urinate (frequency), urgent need to urinate (urgency), and Incontinence (urine leakage)
- Painful urination (dysuria) and blood in the urine
- They require to urinate at night
- Abnormal urine color (cloudy urine) and powerful or foul-smelling urine.
Some of the symptoms of urinary tract infections (UTIs) include:
- Wanting to urinate more sometimes and urgently, if only a few drops
- Sometimes burning pain or a ‘scalding’ sensation when urinating
- Feeling that the bladder is still full later urinating
- Pain over the pubic bone
- Cloudy, bloody, or very bad smelly urine.
If the infection reaches the kidneys, prompt medical attention is required. In addition to the general symptoms of urinary tract infections (UTIs), a person with a kidney infection can also experience:
- Chills
- Fever
- Loin (lower abdominal) pain
- Pain in the back
- Vomiting.
Urinary Tract infections ((UTIs) that are left untreated may lead to many complications, including urosepsis, systemic inflammatory response syndrome (SIRS), and chronic kidney infections. Sepsis associated with urinary tract infections (UTIs) often requires hospitalization.
Other symptoms that may be associated with a urinary tract infection involve:
- Pain during sex
- Penis pain
- Flank (side of the body) pain or low back pain
- Fatigue
- Fever (temperature above 100 degrees Fahrenheit) & chills
- Vomiting
- Mental changes or confusion.
Lower tract urinary tract infection (UTI) symptoms
Lower tract urinary tract infections (UTIs) affect the urethra and bladder. Symptoms of a lower tract urinary tract infection (UTI) include:
- burning with urination
- increased frequency of urination without passing much urine
- increased urgency of urination
- bloody urine
- cloudy urine
- urine that looks like cola or tea
- urine that has a strong odor
- pelvic pain in women
- rectal pain in men.
Upper tract UTI symptoms
Upper tract urinary tract infections (UTIs) affect the kidneys. These can be potentially life-threatening if bacteria go from the infected kidney into the blood. This condition, also known as urosepsis, can cause dangerously low blood pressure, shock, and death.
Symptoms of an upper tract urinary tract infection (UTI) include:
- pain and tenderness in the upper back and sides
- chills
- fever
- nausea
- vomiting.
Urinary tract infection (UTI) symptoms in men
Symptoms of an upper tract urinary infection in men are the same as those in women. But men with a lower tract urinary tract infection (UTI) may sometimes also experience rectal pain.
Urinary tract infection (UTI) symptoms in women
Women with a below-tract urinary infection may experience pelvic pain. This is in addition to the other usual symptoms.
Variation in Symptom Presentation
- Post-menopausal women present with constitutional symptoms, like abdominal pain, back pain, chills, and constipation.
- Nursing home patients present with nonspecific symptoms, like confusion and a decline in functional status.
- A urinary infection in a child requires to be investigated as it may indicate a more serious condition. The most usual urinary system condition is urinary reflux. With this condition, the bladder valve is not working properly and allows urine to flow back to the kidneys, increasing the risk of a kidney infection.
What are the risk factors for urinary tract infections (UTIs)?
- Anything that decreases your bladder emptying or irritates the urinary tract can lead to a urinary tract infection (UTI). There are many factors that can put you at an increased risk of getting a urinary tract infection (UTI).
These risk factors involve:
- age (older adults are more likely to get urinary tract infections (UTIs)),
- reduced mobility later surgery or prolonged bed rest
- kidney stones
- a previous urinary tract infection (UTI)
- urinary tract obstructions or blockages, like:
- enlarged prostate
- kidney stones
- certain forms of cancer
- prolonged use of urinary catheters, which may create it easier for bacteria to get into your bladder
- diabetes
- pregnancy
- abnormally developed urinary structures from birth
- weakened immune system.
Additional urinary tract infection (UTI) risk factors for men
- Most urinary tract infection (UTI) risk factors for men are the same as those for women. But having an enlarged prostate can also increase urinary tract infection (UTI) risk.
Additional urinary tract infection (UTI) risk factors for women
- While it is widely believed that wiping from back to front after using the bathroom increases the risk of recurring urinary tract infections (UTIs), older research showed that this is not the case.
- But there are still certain risk factors unique to female anatomy.
Shorter urethra
- In female bodies, the urethra is very near to both the vagina and the anus. This increases the likelihood of developing urinary tract infections (UTIs). Bacteria that may naturally happen around both the vagina and anus can conduct to infection in the urethra and the rest of the urinary tract.
- Urethras in women are shorter, and the bacteria have a shorter distance to move to enter the bladder.
Sex
- Pressure on the female urinary tract during penetrative sex can move bacteria from near the anus into the bladder. Oral sex can introduce bacteria into the urethra, increasing the risk of infection.
- Peeing after sex may assist reduce the risk of infection.
Spermicides
- Spermicides may increase urinary tract infection (UTI) risk because they can disrupt the vaginal microbiome.
Condom use during sex
- Non-lubricated latex condoms may increase friction and annoy the skin during sexual intercourse. This may increase the risk of a urinary tract infection (UTI).
- Yet there are many reasons to use condoms. They are mainly for reducing the spread of sexually transmitted infections (STIs) and preventing unwanted pregnancy.
- To assist cure friction and skin irritation from condoms, be sure to use enough water-based lubricant during sex.
- Avoid using condoms coated with spermicide.
Diaphragms
- Diaphragms may create pressure on the urethra. This can lower bladder emptying, which increases the risk of bacterial growth and infection.
Decrease in estrogen levels
- After menopause, a decrease in estrogen levels changes the normal bacteria in your vagina. This can increase the risk of a urinary tract infection (UTI).
Systemic Involvement
- Urinary Tract infections (UTIs) that are left untreated may lead to many complications, including urosepsis, systemic inflammatory response syndrome (SIRS), and chronic kidney infections. Sepsis associated with urinary tract infections (UTIs) often requires hospitalization.
- Urosepsis grows into the bloodstream from its origin in the urinary tract. Kidney infections progress to the bloodstream referred to as septicemia. This complication can be life-threatening. Systemic inflammatory response syndrome can become life-threatening if treatment fails.
- Systemic inflammatory response syndrome (SIRS) is usually the first incidence of multi-organ failure.
How are urinary tract infections (UTIs) diagnosed?
Your doctor will use the following tests to diagnose a urinary tract infection (UTI):
- Urinalysis: This test will examine the urine for red blood cells (RBCs), white blood cells (WBCs), and bacteria. The number of white and red blood cells (WBCs & RBCs) found in your urine can actually indicate an infection.
- Urine culture: A urine culture is used to direct the type of bacteria in your urine. This is an important test because it assists to determine the appropriate treatment.
If your infection does not respond to treatment or if you remain to get infections over and over again, your doctor may use the following tests to examine your urinary tract for disease or injury:
- Ultrasound: In this test, sound waves make an image of the internal organs. This test is done on top of your skin, is painless, and does not typically need any preparation.
- Cystoscopy: This test uses an important instrument fitted with a lens and a light source (cystoscope) to see inside the bladder from the urethra.
- CT scan: Another imaging test, a CT scan is a type of X-ray that takes cross sections of the body (such as slices). This test is much more precise than common X-rays.
Upper tract urinary tract infections (UTIs)
- If your doctor suspects that you have an upper tract urinary tract infection (UTI), they may also need to do a complete blood count (CBC) and blood cultures, in addition to the urine test.
- A blood culture can confirm that your infection has not spread to your bloodstream.
Chronic urinary tract infections (UTIs)
- Most urinary tract infections (UTIs) go away after treatment. But some people develop chronic urinary tract infections (UTIs). Chronic urinary tract infections (UTIs) either do not go away after treatment or keep recurring. Recurrent urinary tract infections (UTIs) are common among women.
- If you have chronic urinary tract infections (UTIs), your doctor may want to check for any abnormalities or obstructions in your urinary tract.
Here are certain common tests:
- An ultrasound is where a device known as a transducer is passed over your abdomen. The transducer uses ultrasound waves to make an image of your urinary tract organs that are displayed on a monitor.
- An intravenous pyelogram (IVP) involves injecting a dye into your body that moves through your urinary tract. After, an X-ray of your abdomen is taken. The dye highlights your urinary tract (UT) on the X-ray image.
- A cystoscopy uses a small camera that is inserted through your urethra and up into your bladder to see inside your bladder. During a cystoscopy, your doctor may remove a tiny piece of bladder tissue and test it to rule out bladder inflammation or cancer as a cause of your symptoms.
- A computerized tomography (CT) scan acquires more detailed images of your urinary system.
Urinary tract infections (UTIs) during pregnancy
- If you are pregnant and have symptoms of a urinary tract infection (UTI), see your doctor right away.
- Urinary tract infections (UTIs) during pregnancy can cause high blood pressure and premature delivery. Urinary tract infections (UTIs) during pregnancy are also more likely to spread to the kidneys.
How are urinary tract infections (UTIs) treated?
You will require to treat a urinary tract infection. Antibiotics are medicines that destroy bacteria and fight infection. Antibiotics are commonly used to cure urinary tract infections (UTIs). Your healthcare provider (doctor) will pick a drug that best treats the particular bacteria that is causing your infection. Some commonly used antibiotics can involve:
- Nitrofurantoin
- Sulfonamides (sulfa drugs)
- Amoxicillin
- Cephalosporins
- Trimethoprim/sulfamethoxazole (Bactrim)
- Doxycycline
- Quinolones (such as ciprofloxacin [Cipro]).
- It is very main that you follow your healthcare provider’s (doctor’s) directions for taking the medicine. Do not stop taking the antibiotic because your symptoms go away and you begin feeling better. If the infection is not treated completely with the complete course of antibiotics, it can return.
- If you have a history of frequent urinary tract infections (UTIs), you may be given a prescription for antibiotics that you would take at the 1st onset of symptoms. Other patients may be given antibiotics to take every day, every other day, or later sexual intercourse to prevent the infection. Talk to your healthcare provider (doctor) about the best treatment option for you if you have a history of frequent urinary tract infections (UTIs).
Physical Therapy Management
- Physical therapists that are trained in pelvic floor dysfunction can greatly increase a urinary tract infection (UTI) patient’s quality of life.
- A typical approach involves training pelvic floor musculature, manipulative techniques, local heat, breathing and relaxation techniques, postural education, muscle coordination reeducation, and behavioral therapy.
- Therapists are encouraged to educate the patient on drinking and voiding schedules to ensure consistency. Treatments and patient education have been found to improve the efficiency of emptying the bladder, create better bowel habits, and promote full relaxation of the pelvic floor when voiding.
- All of these factors may lead to a decreased incidence and reoccurrence of urinary tract infections (UTIs).
- For those patients in the hospital, recent studies have shown that mobilization of patients with a catheter is safe and is not associated with urinary-related adverse effects, involving urinary tract infections (UTIs).
What are the complications of urinary tract infections (UTIs)?
- Urinary tract infections (UTIs) can be easily treated with antibiotics. However, if it is not treated or if you stop the medication early, this type of infection can conduct into a more serious infection, such as a kidney infection.
Can I become immune to the antibiotics used to treat a urinary tract infection (UTI)?
- Your body can actually get used to the antibiotics commonly used to treat a urinary tract infection (UTI). This occurs in people who have very frequent infections. With each urinary tract infection (UTI) and the use of antibiotics to treat it, the infection adapts and becomes harder to fight. This is known as an antibiotic-resistant infection. Because of this, your healthcare provider (doctor) may suggest alternative treatments if you have sometimes urinary tract infections (UTIs).
These could include:
- Waiting: Your provider (doctor) may suggest that you watch your symptoms and wait. During this time, you may be encouraged to drink plenty of fluids (especially water) in an attempt to “flush out” your system.
- Intravenous treatment: In certain very complicated cases, where the urinary tract infection (UTI) is resistant to antibiotics or the infection has moved to your kidneys, you may need to be treated in the hospital. The medicine will be given to you straight in your vein (intravenously). Once you are home, you will be prescribed antibiotics for a period of time to fully get rid of the infection.
Does cranberry juice cure a urinary tract infection (UTI)?
- Many people say that cranberry juice can assist treat, or even prevent, a urinary tract infection (UTI). Researchers are currently looking into the topic, but have not found a definitive answer yet. Healthcare providers (doctors) recommend drinking lots of fluids if you have or have a history of getting, a urinary tract infection (UTI). Adding a glass of unsweetened cranberry juice to your diet is not a proven way to prevent a urinary tract infection (UTI), but it typically who not hurt you either.
Untreated urinary tract infections (UTIs)
- It is important to treat a urinary tract infection (UTI) — the earlier, the better. Untreated urinary tract infections (UTIs) become more and more severe the further they spread.
- A urinary tract infection (UTI) is usually the easiest to treat in the lower urinary tract. An infection that spreads to the upper urinary tract is much harder to treat and is more likely to spread into your blood, causing sepsis. This is life-threatening in the end.
- If you suspect that you have a urinary tract infection (UTI), contact your doctor as soon as possible. A simple examination and urine or blood test could save you a lot of trouble in the long travel.
Can I prevent a urinary tract infection (UTI)?
You can usually cure a urinary tract infection (UTI) with lifestyle changes. These tips can involve:
- Practicing good hygiene: You can often prevent urinary tract infections (UTIs) by practicing good personal hygiene. This is especially main for women. Because the urethra in women is much shorter than it is in men, it is easier for E. coli bacteria to progress from the rectum back into the body. To avoid this, it is recommended that you always wipe from front to back later a bowel movement. Women should use good hygiene practices during their menstrual cycle to avoid infections. Changing pads and tampons frequently, as well as not using feminine deodorants can also help prevent urinary tract infections (UTIs).
- Drinking plenty of fluids: Adding extra fluids, especially water, to your daily routine can assist remove extra bacteria from your urinary tract. Drinking 6 to 8 glasses of water per day is recommended.
- Changing your urination habits: Urination can play a major role in getting rid of bacteria from the body. Your urine is a waste product and each time you empty your bladder, you are removing that waste from your body. Urinating frequently can decrease your risk of developing an infection, especially if you have a history of frequent urinary tract infections (UTIs). Drinking plenty of fluids will encourage this, yet makes sure to avoid fluids and foods that could irritate your bladder. These can involve alcohol, citrus juices, caffeinated drinks, and spicy foods. You should also try to urinate immediately previous and after sex. This could assist flush out any bacteria that may have been introduced during intercourse. You can also wash the genital area with warm water before having sex. Do not douche. This practice is not recommended by healthcare providers (doctors).
- Changing your birth control: Some women have an increased risk of developing a urinary tract infection (UTI) if they use a diaphragm for birth control. Talk to your healthcare provider (doctor) about other options for birth control.
- Using a water-based lubricant during sex: If you experience vaginal dryness and use a lubricant during sex, utilize one that is water-based. You may also need to avoid spermicide if you have frequent urinary tract infections (UTIs).
- Changing your clothing: Avoiding tight-fitting clothing can actually assist keep you dry, preventing bacteria from growing in the urinary tract. You can switch to cotton underwear. This will cure extra moisture from getting trapped around your urethra.
- In some post-menopausal women, a healthcare provider (doctor) may suggest an estrogen-containing vaginal cream. This may reduce the risk of developing a urinary tract infection (UTI) by changing the pH of the vagina. Talk to your healthcare provider (doctor) if you have recurrent urinary tract infections (UTIs) and have already gone through menopause.
- Over-the-counter supplements are also available for urinary tract infections (UTIs). These are sometimes recommended for people who have frequent urinary tract infections (UTIs) as another way to prevent them. Talk to your healthcare provider (doctor) before starting any supplements and ask if these could be a good choice for you.
Everyone can take the following steps to help prevent urinary tract infections (UTIs):
- Drink six to 8 glasses of water daily.
- Do not hold urine in for prolonged periods of time.
- Ask your doctor about managing any urinary incontinence or difficulties fully emptying your bladder.
- Women are 30 times trusted Source more likely than men to get urinary tract infections (UTIs). Certain steps may help prevent urinary tract infections (UTIs) in women.
- If you are perimenopausal or postmenopausal, using topical or vaginal estrogen prescribed by your doctor could make a difference in preventing urinary tract infections (UTIs). If your doctor believes that intercourse is a factor in your recurrent urinary tract infections (UTIs), they may recommend taking preventive antibiotics after sex or long-term.
- Some studies have shown that long-term preventive use of antibiotics in older adults reduced the risk for urinary tract infections (UTIs).
- Taking daily cranberry supplements or using vaginal probiotics, like lactobacillus, may also help prevent urinary tract infections (UTIs). Some studiesTrusted Source suggests that using probiotic vaginal suppositories can decrease the occurrence and recurrence of urinary tract infections (UTIs) by changing the bacteria found in the vagina.
- Be sure to discuss with your doctor what the right cure plan is for you.
What is the prognosis (outlook) for a person with a urinary tract infection (UTI)?
- Urinary tract infections (UTIs) commonly respond very well to treatment. A urinary tract infection (UTI) can be uncomfortable before you start treatment, but once your healthcare provider (doctor) identifies the type of bacteria and prescribes the right antibiotic medication, your symptoms should improve quickly.
- It is important to keep taking your medication for the entire amount of time your healthcare provider (doctor) prescribed. If you have frequent urinary tract infections (UTIs) or if your symptoms are not improving, your provider may test to see if it is an antibiotic-resistant infection. These are more complicated infections to treat and may need intravenous antibiotics (through an IV) or alternative treatments.
When should I call my healthcare provider (doctor)?
Call your healthcare provider (doctor) if you have symptoms of a urinary tract infection. If you have been diagnosed with a urinary tract infection (UTI) and your symptoms are getting worse, call your healthcare provider (doctor). You may require a different treatment. Look out for these symptoms in particular:
- Fever
- Back pain
- Vomiting.
- If you have any of these symptoms, or your other symptoms continue later in treatment, call your healthcare provider. A urinary tract infection (UTI) can spread throughout your urinary tract and into other areas of your body. However, treatment is very effective and can fastly relieve your symptoms.
FAQs
Pain or burning while urinating.
Frequent urination.
Feeling the need to urinate despite having an empty bladder.
Bloody urine.
Pressure or cramping in the groin or lower abdomen.
Lower urinary tract infections (UTIs) are common and aren’t usually a cause for major concern. Upper urinary tract infections (UTIs) can be serious if left untreated, as they could damage the kidneys or spread to the bloodstream.
Antibiotics usually are the first treatment for urinary tract infections (UTIs). Your health and the type of bacteria found in your urine determine which medicine is used and how long you need to take it.
Urologist Mark Perlmutter, M.D., says a urinary tract infection (UTI) can go away on its own, but not every type of urinary tract infection (UTI) and not every time. “Yes, a urinary tract infection (UTI) could go away on its own, but some infections are different than others,” he says. “And if left untreated, it may linger longer.”
The bottom line. Stress by itself doesn’t cause urinary tract infections (UTIs), but it can make you more susceptible to infections and other illnesses by harming your immune system. Stress can also trigger or worsen urinary tract symptoms — even if you don’t have a urinary tract infection (UTI)). Your urinary system is vital to your overall health.
Sometimes, the body can resolve minor, uncomplicated urinary tract infections (UTIs) on its own, without antibiotics. By some estimates, 25–42% of uncomplicated UTI infections clear on their own.
Bladder infections are a type of urinary tract infection (UTI), but not all urinary tract infections are bladder infections. A urinary tract infection (UTI) is defined as an infection in one or more places in the urinary tract—the ureters, kidneys, urethra, and/or bladder. A bladder infection is a urinary tract infection (UTI) that’s only located in the bladder.
Most UTIs can be cured. Bladder infection symptoms most often go away within 24 to 48 hours after treatment begins. If you have a kidney infection, it may take 1 week or longer for symptoms to go away.
Additionally, a number of common foods and drinks — artificial sweeteners, spicy foods, alcohol, coffee, acidic fruits, citrus, or caffeinated drinks — can irritate your bladder, and may worsen urinary tract infection (UTI) symptoms — so you should steer clear of them if you have signs of a bladder infection.


One Comment