Psoriasis
- Psoriasis is an autoimmune skin disease that causes itchiness and discomfort. Plaque psoriasis is the most common type. It causes thick, scaly areas of skin. While there is no cure, psoriasis treatment can help manage symptoms. Your provider (doctor) may prescribe special creams or ointments for psoriasis.
Table of Contents
What is psoriasis?
- Psoriasis is an autoimmune disease that causes inflammation in your skin. Symptoms of psoriasis involve thick areas of discolored skin covered with scales. These thick, scaly parts are known as plaques.
- Psoriasis is a chronic skin condition, which means it can flare up unexpectedly and there is no prevention.
- Psoriasis is a chronic autoimmune disease that causes the rapid creation of skin cells. This creation of cells causes scaling on your skin’s surface.
- Inflammation and redness around the scales are fairly usual. Typical psoriatic scales are whitish-silver and grow in thick, red patches. However, on darker skin tones, they can appear more purplish, dark brown with gray scales. Often, these patches will crack and bleed.
- Psoriasis is the outcome of a sped-up skin production of process. Commonly, skin cells grow deep in your skin and steadily rise to the surface. Eventually, they fall off. The usual life cycle of skin cells is one month.
- In people with psoriasis, this production process may happen on just a certain day. Because of this, skin cells do not have time to down off. This rapid overproduction conducts to the creation of skin cells.
- Scales commonly develop on joints, like elbows and knees.
However, they may create anywhere on your body, involving the:
- hands
- feet
- neck
- scalp
- face.
Less usual types of psoriasis affect the:
- nails
- mouth
- the area around the genitals.
Maintain to one study trusted Source published in 2021, around 7.5 million American (US) adults ages 20 and older have psoriasis — a 3 (three) percent prevalence rate (occurrence of a condition). By race and ethnicity, the generality rates are:
- 3.6 percent of white people
- 3.1 percent of non-Hispanic people, involving multiracial people
- 2.5 percent of Asian people
- 1.9 percent of Hispanic people, involving Mexican American people
- 1.5 percent of Black people.
It is commonly associated with several other conditions, involving:
- type 2 diabetes
- inflammatory bowel disease
- heart disease
- psoriatic arthritis
- anxiety
- depression.
What are the types of psoriasis?
There are so many types of psoriasis, including:
Plaque psoriasis
- Plaque psoriasis is the most usual type of psoriasis. About 80% to 90% of people with psoriasis have plaque psoriasis.
- The American Academy of Dermatology (AAD) estimates that about 80 to 90 percent of people with the disease have plaque psoriasis. It causes red, inflamed patches on light skin tones and purple or grayish color or darker brown patches on the skin of color — making it harder to diagnose in people of color.
- These patches are often covered with whitish-silver scales or plaques and are often more severe on the skin of colorTrusted Source. These plaques are typically found on the elbows, knees, and scalp.
Inverse psoriasis
- This type looks in your skin folds. It causes small plaques without scales.
- Inverse psoriasis causes bright parts of red, shiny, inflamed skin. Patches of inverse psoriasis create under your armpits or breasts, in your groin, or around skinfolds in your genitals.
Guttate psoriasis
- Guttate psoriasis may appear later as a sore throat caused by a streptococcal infection. It looks such as small, red, drop-shaped scaly spots and often affects children and young adults.
- Guttate psoriasis commonly happens in childhood. This type of psoriasis causes little pink or violet spots. The most common sites for guttate psoriasis involve your torso, arms, and legs. These spots are rarely thick or raised such as plaque psoriasis.
Pustular psoriasis
- Pustular psoriasis has little, pus-filled bumps on top of plaques.
- Pustular psoriasis is more usual in adults. It causes white, pus-filled blisters and broad parts of red or violet —depending on skin tone — inflamed skin. It can look like a more intense violet color on darker skin tones. Pustular psoriasis is typically localized to smaller parts of your body, such as the hands or feet, but it can be widespread.
Erythrodermic psoriasis
- This is a severe type of psoriasis that harms a large area (more than 90%) of your skin. It causes general skin discoloration and skin shedding.
- Erythrodermic psoriasis is a serious and very rare type of psoriasis, according to the National Psoriasis Foundation.
- This form sometimes covers large sections of your body at once. The skin almost appears sunburned. Scales that develop sometimes slough off in large sections or sheets. It is not uncommon for you to run a fever or become very ill with this form of psoriasis.
- This type can be life-threatening, so it is important that you make an appointment with a healthcare professional immediately.
Sebopsoriasis
- This type typically looks on your face and scalp as bumps and plaques with a greasy, yellow scale. This is a cross between middle psoriasis and seborrheic dermatitis.
Nail psoriasis
- Nail psoriasis causes skin discoloration, pitting, and changes to your fingernails and toenails.
What part of my body will psoriasis affect?
A psoriasis rash can look up anywhere on your skin. Psoriasis is usually on your:
- Elbows and knees.
- Face and inside of your mouth.
- Scalp
- Fingernails and toenails.
- Genitals.
- Lower back.
- Palms and feet.
- In most people, psoriasis covers a small part of their skin. In severe cases, the plaques connect and cover a large part of your body.
What is psoriatic arthritis?
- Psoriatic arthritis is a type of arthritis that causes joint pain and swelling. Similar to psoriasis, psoriatic arthritis is an autoimmune disease that causes your immune system to function abnormally and causes symptoms. About 1 in 3 people diagnosed with psoriasis will also create arthritis due to inflammation. Early treatment of psoriatic arthritis can decrease damage to your joints.
Whom does psoriasis affect and how common is it?
- People of any age, sex, or race can get psoriasis. Psoriasis affects millions of people. More than 3% of the U.S. (America) population has psoriasis.
Is psoriasis the same as eczema?
- Psoriasis and eczema are two various skin conditions. Both conditions cause similar symptoms such as discolored skin, a rash, and itching. Psoriasis plaques cause parts of thick skin covered in scales. Eczema causes a rash of dry and bumpy skin. Eczema also commonly causes more intense itching than psoriasis.
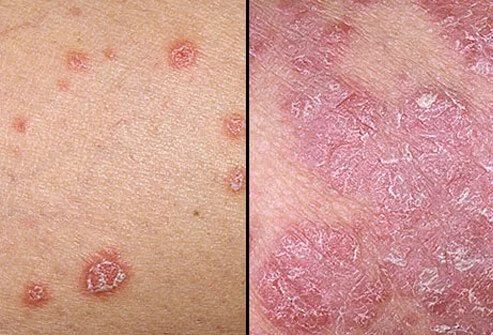
What does psoriasis look like?
Symptoms of psoriasis on your skin involve plaques. The plaques look like this:
- A rash or a raised part of thick skin.
- The skin on the plaque is discolored.
- The plaque is scaly or flaky and sheds freely.
- An early sign of psoriasis is little bumps. The bumps grow, and scales form on high. The surface of the plaque might shed, yet the scales beneath them will stick together. If you abrade you are, the scales may tear go away from your skin. This can cause bleeding. As the rash continues to grow, lesions (larger parts of skin damage) can form. Symptoms of psoriasis disease can range from mild (light) to severe (serious).
What are the symptoms of psoriasis?
- Not every person will experience all these symptoms. Certain people will experience entirely various symptoms if they have a less common type of psoriasis.
- Most people with psoriasis go through “cycles” of symptoms. The condition may cause serious symptoms for certain days or weeks, and then the symptoms may clear up and be almost unnoticeable. Then, in certain weeks or if made worse by a casual psoriasis trigger, the condition may flare up again. Often, symptoms of psoriasis disappear completely.
- When you have no active signs of the condition, you may be in “remission.” That does not mean psoriasis will not come back, yet for this period of time, you are symptom-free.
You might have symptoms that involve:
- Itchy skin.
- Cracked, dry skin.
- Skin pain.
- Nails that are pitted, cracked, or crumbly.
- Joint pain.
- If you abrade your plaque, you could break open your skin, which could conduct to an infection. Infections are serious. If you experience serious pain, swelling, and a fever, you have symptoms of an infection.
What causes psoriasis outbreaks?
An outbreak of psoriasis, or a flare-up, causes symptoms of psoriasis as an outcome of contact with a trigger, which could be an irritant or an allergen. Psoriasis outbreaks are various from person to person. Common triggers for psoriasis flare-ups involve:
- Emotional stress.
- An infection (streptococcal infection).
- A skin injury such as cuts, scrapes, or surgery.
- Certain medications, such as lithium and beta-blockers.
- Changes in body temperature because of the weather.
Is psoriasis contagious?
- No, psoriasis is not contagious. You can not acquire psoriasis by coming into contact with another person’s psoriasis skin rash.
How is psoriasis diagnosed?
A healthcare provider or a dermatologist will diagnose psoriasis later a physical exam to look at your skin and review your symptoms. They’ll ask you questions that could involve:
- Do you have a history of skin diseases in your biological family?
- When did you 1st notice symptoms?
- Have you attempted any at-home remedies to treat your skin?
- Is this the first time you have had an outbreak on your skin?
- What types of soaps or shampoos do you help with?
- The appearance of a skin plaque conducts to a psoriasis diagnosis, yet symptoms can relate to other similar skin conditions, so your provider might offer a skin biopsy test to confirm your diagnosis. During this test, your provider will remove a little sample of skin tissue from your skin plaque and examine it under a microscope.
How is psoriasis treated?
So many treatment options can relieve psoriasis symptoms. Common psoriasis treatments involve:
- Steroid creams.
- Moisturizers for dry skin.
- Medication to slow skin cell production (anthralin).
- Medicated lotions or shampoos.
- Vitamin D3 ointment.
- Vitamin A or retinoid creams.
- Creams or ointments may be enough to increase the rash in small areas of your skin. If your rash harms larger areas, or if you also have joint pain, you will need other treatments. Joint pain may be a sign that you have arthritis.
Your provider (doctor) will decide on a treatment plan based on:
- The severity of the rash.
- Where the rash is on your body.
- Your age.
- Your overall health.
Physiotherapy Treatment
- The patient should be referred to a rheumatologist suddenly if undiagnosed psoriatic arthritis is suspected. All patients with manifestations of arthritic-type diseases should be asked if they have any type of skin disease or patches of dry skin. They should also be encouraged to look for a rheumatologist that can verify the type of arthritis that they have.
- Physical therapy can play an important role in increasing the life of a person with psoriatic arthritis. Physical therapy management should focus on education, improvement of range of motion (ROM), strengthening, and general cardiovascular conditioning. Physical therapists may also provide UV therapy and modalities to reduce pain. Cryotherapy may assist to reduce swelling and tenderness in affected joints. Heat may be used to relax joint pain. Paraffin baths protect to be soothing for the hands and feet. Splinting may be of benefit to cure deformity.
- Recently studies have looked that hydrotherapy is also an effective treatment for patients with psoriatic arthritis. Hydrotherapy has been shown to increase physical function, energy, sleep and relaxation, cognitive function, work, and participation in patients with psoriatic arthritis.
What if common psoriasis treatments do not work?
If your symptoms of psoriasis do not improve after treatment, or if you have large areas of involvement (10% of your skin or more), your healthcare provider (doctor) may recommend the following treatments:
- Light therapy: LED lights at specific wavelengths can decrease skin inflammation and assist slow your skin cell production.
- PUVA: This treatment combines a medication known as psoralen with exposure to a special form of ultraviolet light.
- Retinoids: These vitamin A-related drugs can assist your psoriasis symptoms but may cause side effects, including birth defects.
- Immune therapies: Newer immune therapy medications (biologics and small molecule inhibitors) work by blocking your body’s immune system so it can not cause an autoimmune reaction.
- Methotrexate: Providers recommend this medication for serious cases of psoriasis. It may cause liver disease. If you take it, your provider (doctor) will monitor your progress with blood tests. You may require periodic liver biopsies to check your liver health.
- Cyclosporine: This medicine can assist severe psoriasis but it may cause high blood pressure and kidney damage.
- Before starting treatment, talk to your healthcare provider (doctor) about the side effects and mention any medications or supplements you currently take to avoid drug interaction.
Are there any complications of psoriasis?
For certain people diagnosed with psoriasis, the skin condition causes more than itchiness, scaling skin, and skin discoloration. It can conduct to swollen joints and arthritis. If you have psoriasis, you may be at greater risk of:
- Diabetes.
- Obesity.
- High cholesterol.
- Strokes.
- Heart attacks.
If you have psoriasis, your provider (doctor) will do regular blood pressure checks and monitor the progress of your treatment to avoid complications. You can require steps to prevent potential complications by:
- Eating a well-balanced diet.
- Exercising regularly.
- Getting adequate sleep
- Not smoking.
How soon after treatment will I feel better?
- A flare-up of psoriasis symptoms can last a couple of weeks to a certain month. Your healthcare provider (doctor) can speed up your skin’s recovery with certain medications. Later your symptoms go away, your psoriasis is in remission. This means that you could have other outbreaks of symptoms in the future. Your remission timeline could last a certain month to a couple of years. If you notice your symptoms flare up when you contact certain triggers, avoiding those triggers conducts a long remission time.
How can I prevent psoriasis?
- There is no way to entirely prevent psoriasis. You can decrease your risk by following your healthcare provider’s treatment, living a healthy lifestyle, taking good care of your skin, and keeping away triggers that can cause an outbreak of symptoms.
What can I expect if I have psoriasis?
- If you have psoriasis, it is common to see symptoms show up during early adulthood, but the timeline of when symptoms begin is unique to every person. You may notice some triggers in your environment that can cause a flare-up of symptoms. Avoiding these triggers can conduct in fewer outbreaks in the future.
- Psoriasis can create you uncomfortable, itchy, and self-conscious. If these symptoms are causing you physical or emotional distress, contact your healthcare provider (doctor) for treatment.
Is there a cure for psoriasis?
- There is no cure for psoriasis. Psoriasis is a chronic condition, which means that symptoms may here and go throughout your life. Treatment can relieve symptoms so you can see and feel your best.
How do I take care of myself?
To feel good with psoriasis:
- Take medications as instructed.
- Use moisturizer regularly, especially later bathing.
- Avoid harsh soaps.
- Help medicated shampoo for scales on your scalp.
- Another step you should require to stay as healthy as possible:
Talk to your healthcare provider (doctor) about lowering your risk for related conditions, like heart disease, depression, and diabetes.
Lower your stress with meditation, exercise, or seeing a mental health professional.
When should I see my healthcare provider?
Do regular skin self-exams to notice any exchanges in your skin. If you have skin changes, a rash that is not going away, or a rash that gets worse, contact your healthcare provider (doctor).
- What questions should I ask my doctor?
- How can I prevent outbreaks and manage symptoms?
- What medication will work best for me?
- What else should I do to increase my symptoms?
- What are my options if creams do not work?
- Will psoriasis ever go away?
NOTE
- Psoriasis, an itchy skin condition, can here and go throughout your life. It is related to an overactive immune response and is not contagious. If you have skin changes that are not going away, talk to your healthcare provider.
- There is no cure for psoriasis, but psoriasis treatments can improve symptoms. Your provider (doctor) may prescribe a special cream or moisturizer or medications. Other therapies are available if creams or medicines do not work. Maintaining your overall health will also help increase symptoms.
FAQs
Rashes or patches of red, inflamed skin, are often covered with loose, silver-colored scales; in severe cases, the plaques will grow and merge into one another, covering large areas.
Itchy, painful skin that can crack or bleed.
Small areas of bleeding where the involved skin is scratched.
Although there is no cure, there are more effective treatments for psoriasis today than ever before. Treating psoriasis can help improve symptoms as well as lower the risk of developing other health conditions such as psoriatic arthritis, heart disease, obesity, diabetes, and depression.
Steroid creams or ointments (topical corticosteroids) are commonly used to treat mild to moderate psoriasis in most areas of the body. The treatment works by reducing inflammation. This slows the production of skin cells and reduces itching. Topical corticosteroids range in strength from mild to very strong.
Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition that affects their joints, called psoriatic arthritis.
an injury to your skin, such as a cut, scrape, insect bite, or sunburn – this is called the Koebner response.
drinking excessive amounts of alcohol.
smoking.
stress.
hormonal changes, particularly in women – for example, during puberty and menopause.


4 Comments