Goose Foot Bursitis of the Knee
Table of Contents
What is a Goose Foot Bursitis of the Knee?
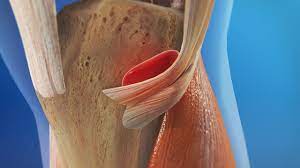
Goosefoot bursitis, also known as pes anserine bursitis, is a condition that involves inflammation of the bursa located on the inner side of the knee, just below the knee joint. The bursa acts as a cushion between the tendons of the hamstring muscles and the shinbone (tibia).
The condition is commonly seen in people who participate in activities that require repetitive knee bending, such as running or cycling, or those who are overweight. Symptoms of goosefoot bursitis may include pain and tenderness on the inner side of the knee, swelling, and stiffness.
Treatment for goosefoot bursitis usually involves resting the affected knee and avoiding activities that aggravate the symptoms. Ice packs and anti-inflammatory medications may be helpful in reducing pain and swelling. Physical therapy and exercises to strengthen the muscles around the knee may also be recommended.
In severe cases, a doctor may recommend a corticosteroid injection into the bursa to reduce inflammation. However, this treatment option is not typically used as a first-line treatment due to potential side effects. If conservative treatments are not effective, surgery may be considered to remove the bursa.
Introduction
Goose Foot Bursitis is a fluid-filled cyst. It secretes synovial fluid to decrease friction between tissues and also works as a cushion for bones, tendons, and muscles. The inflammation of the bursa doesn’t occur unexpectedly but rather advances over some time. Bursitis can also happen in the shoulder, knee, hip, elbow, and big toe. The Goose Foot also documented the ‘Pes Anserine bursitis’ as the insertion of the muscles of sartorius, gracilis, and semitendinosus, which are connected on the medial side of the proximal tibia
The 3 tendons are located superficial to the medial collateral ligament (MCL) of the knee. The sartorius and gracilis muscles are adductors of the leg (that is they draw the leg towards the median axis of the body). The semitendinosus muscle is part of the hamstrings muscle group situated at the back of your upper leg. Together, these three muscles are mainly flexors of the knee and internal rotators.
Cause of Goose Foot Bursitis of the Knee
Goose Foot bursitis usually happens when the associated muscles are repeatedly used, by doing activities for example flexion and adduction. This causes friction and also enhanced the pressure on the bursa. Bursitis may also be due to trauma, for example, a direct hit in the Pes Anserine region. The bursa then becomes inflamed and tendered or hurts and underlying Osteoarthritis of the knee.
Reports suggest that anserine bursitis is more typical in overweight middle-aged females. We can explain this by the fact that females have a wider pelvis, resulting in angulation of the knee in the frontal plane, which shows more pressure in the region of insertion of the pes anserinus by the genu valgum.
We can tell that an inflamed bursa is not a direct pathology, but instead a result of a before intricacy.
Symptoms of Goose Foot Bursitis of the Knee
Goose Foot bursitis induces pain and discomfort on the interior of the knee (mostly during running or climbing stairs). The individual can experience reflexive anteromedial aspect of knee pain on climbing or downstairs and tenderness at the PA. As well, the area around the bursa will be swollen or tender to the touch.
Other symptoms may include:
- Decreased muscle strength
- Gait deviations
- Decreased function
- Decreased ROM
- Postural dysfunction/impaired lower extremity biomechanics
Aggravating factors contain activities that require movements like flexion and end rotation, as well as rotation and adduction. Shifting, kicking, squatting, or quick movements from side to side, for example in the sports mentioned above, can also cause further irritation.
Differential Diagnosis
Goose Foot bursitis is frequently mistaken with other reasons for the medial knee pain
- Stress fracture of the shin bone on the proximal portion will induce pain in the region of the Pes Anserine.
- Patellofemoral pain syndrome.
- Medial meniscus lesion and osteoarthritis.
- Panniculitis happens in obese people and causes painful inflammation of subcutaneous fat at night.
- Semimembranosus tendinitis will frequently happen as a running injury.
- Medial Plica Syndrome, which may induce pain and tenderness on the medial aspect of the knee.
- Extra-articular cystic lesions: synovial cyst, ganglionic cyst, para meniscal cyst, pigmented villonodular synovitis, synovial sarcoma.
In addition to the conditions listed above, other situations to be considered contain the following:
- Atypical medial meniscal cysts
- Juxta-articular bone cysts
- Semimembranosus bursitis
- Tibial collateral ligament bursitis
Diagnostic Procedures
Lateral X-ray views of the patient’s knee are very helpful for ruling out a stress fracture, arthritis, or even Osteochondritis Dissecans. An MRI is required to clarify damage caused to other areas of the medial side of the knee. An MRI could avert unwarranted arthroscopy. MRI findings must correspond with those of a physical assessment.
Examination
The pes anserine bursa may be located at a point barely down to the tibial tubercle and about three-four centimeter medial aspect to it (about 2 finger breadths.
Analyze hamstring length with the patient in the supine position. Flex the patient’s hip 90° and then extend the knee as far as possible. How distant the knee can be extended will tell hamstring length and tightness. If the patient’s knee may be straightened fully then the hamstrings are not tight.
With the sports-associated variant of pes anserine bursitis, the clinical presentation may be produced by norms of resisted internal rotation and resisted flexion of the knee. With the chronic variant in more aged adults, flexion or extension of the knee commonly does not provoke pain.
Medical Treatment
The initial therapy of pes anserine bursitis is rest and non-steroidal anti-inflammatory drugs(NSAID) modalities, possess local injection of a corticoid, for example, methylprednisolone, are used in a few circumstances. Intrabursal injection of regional anesthetics, corticosteroids, or both consists of another option of management.
Surgical treatment is suggested in cases with failure to conservative treatments. Simple surgical cuts and drainage of the distended bursa can sweeten symptoms in a few documented circumstances. The bursa may be withdrawn if the chronic infection cannot be cleared up with antibiotics.
After surgery, if the bursa is released, follow the identical steps of rehabilitation and recovery drafted under physical therapy management. If bursitis leads to infection and common antibiotic treatments are useless, A surgical decompression of the bursa can be key in this circumstance.
Physiotherapy Treatment
Physiotherapy is the mainstay in the therapy of the Pes Anserine syndrome. To temper, the pain driven by bursitis, the most essential thing of all is rest. avert stairs climbing, or other irritating movements to calm down the bursa and the corresponding pain. Nonsteroidal anti-inflammatory drugs (NSAID) can be brought to help the pain. Restrict movement and alternately involve ice while the inflammatory phase. An ice massage of 15 minutes every 4-7 hours will reduce inflammation.
An elastic bandage can be wrapped around the knee to decrease any swelling or to prevent swelling from occurring. Be conscious not to improve friction. Instruct the patient on muscle-conditioning exercises. These may contain leg stretching exercises for example hamstring lengthening, standing calf lengthening, hip adductor lengthening, heel slide, standing quadriceps lengthening quadriceps isometrics, and hamstrings isometrics. Advanced of these exercises may contain closed-kinetic chain exercises such as single-knee dips, squats, and leg presses. Resisted leg pulls using elastic tubing are also involved.
The closed-kinetic chain form of workouts is also suggested to prevent the development of instability in the collateral knee, which happens to be a chance factor for Pes Anserine bursitis.
Ultrasound has been useful in the decline of the inflammatory process in pes anserine bursitis. few individuals acquire an injection that consists of a solution of anesthetic and steroid. Thereafter, a physiotherapist will provide a hamstring stretching program and a contemporary closed-chain quadriceps strengthening program that has to repeat various times a day. This will result in less pain at about six-eight weeks.
Kinesiotaping is more useful than naproxen or physical therapy in the lessening of pain and swelling.
Summary
Goose Foot bursitis is typically related to osteoarthritis or overweight women. A distinctive trait is involuntary anteromedial knee pain on climbing or descending stairs. The differential diagnosis is very encompassing. It does not vanish without therapy for example rest, ice application, stretching, and ultrasound. Another frequently used therapy is the intrabursal injection of corticosteroids.
FAQ
Generally, pes anserine bursitis will heal within 6-8 weeks or shortly, relying on its severity, fair therapy, or rest. Generally, it is most suitable to retain all movements that influence the knee until the trauma has completely healed, and the bursa is no longer inflamed.
This early clinical manifestation of pes anserine bursitis or tendinopathy is commonly unnoticed by the patient, as time passes it fades fast with walking about or using heat that is a hot shower over the interior of the knee. Yet, as you continue to exercise, the tendinopathy continues and the pain within the tendon evolves more painful and more regular.
1. Rest your knee. Discontinue the activity that induced knee bursitis and prevent movements that aggravate your pain.
2. Take over-the-counter pain relievers
3. Cryotherapy
4. Apply compression
5. Elevate your knee.
Bursitis generally gets better on its own. Conservative standards, for example, rest, ice, and carrying a pain reliever, can relieve discomfort. If conservative standards do not function, you might need Drugs.
Vitamin B12 injections have been displayed to ease the clinical manifestations of acute shoulder bursitis and downsize the quantity of calcification in a few circumstances.