Pseudarthrosis of Spine
Table of Contents
What is Pseudarthrosis of the Spine?
Pseudarthrosis, also known as a nonunion, refers to the failure of a bone to heal after a fracture or surgical fusion. When it occurs in the spine, it is referred to as pseudarthrosis of the spine or spinal nonunion.
When two bones do not properly fuse together, it is known as pseudoarthrosis. This could happen after an accident or after a procedure to fuse bones.
For instance, to address issues with the vertebrae or spine’s bones, physicians may perform spinal fusion surgery. It includes joining the vertebrae together to form one solid bone, which might relieve scoliosis, fix fractures, or boost stability. If the fusion of the bones is unsuccessful, the person develops pseudoarthrosis.
The cost per QALY (quality-adjusted life year) obtained through pseudoarthrosis, also known as non-union, after spinal fusion surgery is projected to be around US$118,945. Rate estimates fluctuate significantly among research using various surgical procedures and patient demographics.
Pseudarthrosis is often described as the inability of two vertebrae to osseously unite within a year following surgery.3 Regardless of the initial rationale for the fusion surgery, the surgeon should not assume that their patient has met a surgical goal until strong bone fusion is accomplished.
Both diagnosis and treatment of pseudoarthrosis can be challenging. The patient’s risk variables, which are sometimes impractical to change in the short term, might contribute to the challenge of prevention. Surgeons are urged to be aware of these risk factors and adjust their surgical procedures to reduce the risks as much as possible. Occasionally, this can entail postponing or even forgoing surgical operations if the risk of pseudarthrosis and the bad outcome it brings surpasses any anticipated advantages.
Pseudarthrosis most frequently manifests as pain, which generally has a central source and may not appear for several months after the procedure. The most frequent method of investigation and diagnosis is fine-cut CT scanning, and concurrent infection should always be taken into account. The most common form of treatment includes revision surgery using a variety of methods.
According to an older study from 2016, up to 50% of spinal fusion surgery fail, and surgeons are executing more of these procedures every year.
Causes of Pseudarthrosis of Spine
Pseudarthrosis can result from several sources. They consist of:
- Moving after surgery: Pseudarthrosis can happen if someone moves too soon after fusion surgery before their bones have had a chance to fuse.
- Health issues: Pseudarthrosis may be brought on by specific medical disorders. Ankylosing spondylitis, for instance, is an inflammatory disorder that causes the spine’s bones to join. Potential complications include pseudoarthrosis, which happens when bones nearly join but do not.
- Birth defects: In a few rare instances according to a reliable source, congenital pseudoarthrosis can affect a person from birth. Congenital pseudoarthrosis of the clavicle, or collarbone, is one example. It is also possible to have congenital pseudoarthrosis of the tibia in the lower leg.
- Methods in surgery: According to research from 2021, pseudarthrosis frequently happens in individuals after spinal fusion due to the dangers of several surgical methods surgeons employ.
Techniques that had a higher incidence of pseudarthrosis among the surgical methods the researchers evaluated included:
- Long fusions, which fuse the spine above the upper-end vertebra, osteotomies, which entail chopping or reshaping bone, and pelvic fixation, which involves utilizing rods and screws to immobilize the spine’s base.
- Contrarily, treatments that included entering through the front of the body saw a 30% decrease in pseudoarthrosis rates.
Risk factors for Pseudarthrosis of the Spine
A person’s likelihood of developing pseudoarthrosis is increased by specific lifestyle choices, medical conditions, and drugs. They consist of Reliable Sources:
- older age
- osteoporosis
- metabolic disorders
- smoking
- diabetes
- obesity
- malnutrition
- long-term steroid usage
- vitamin D insufficiency
A 2019 research also examined patient data from those who experienced spine surgery site infections. The number of levels of the spine that were fused, according to the study’s findings, was the primary indicator of whether someone will get pseudoarthrosis.
Pseudarthrosis risk is significantly influenced by patient-related variables. One of the risk variables with the most research is smoking. 100 patients had two-level uninstrumented fusion from the L4 to the sacrum in randomized research by Brown et al. The prevalence of pseudoarthrosis was 8% among nonsmokers compared to 40% among frequent smokers. In a more recent investigation, smoking’s effects were investigated with and without interbody devices and pedicle screw instrumentation. There was no difference in the fusion rates for single-level fusions, but for two-level fusions, pseudoarthrosis was three times more common (29% vs. 11%).
An orthopedic surgeon should not be surprised by the other patient characteristics that affect the union rate because they are comparable to those for general non-unions. Age, steroid and NSAID usage, diabetes, malnutrition, and previous surgeries are a few of them. When treating patients with malignancies, it is important to take into account the fact that perioperative radiation lowers fusion rates as well.
From a surgical perspective, both the number of levels and the use of non-rigid fixation raise the risk of pseudoarthrosis. Any type of instrumentation speeds up fusion compared to uninstrumented fusions. Circumferential fusion sites (interbody and posterolateral) yield the greatest fusion rates, followed by posterior interbody, anterior interbody, and finally posterolateral. There is proof that PEEK interbody devices don’t fuse as quickly or often as titanium ones do.
Symptoms of Pseudarthrosis of the Spine
Pseudarthrosis can occur in patients who show no symptoms. Some people may go through one or more of the following:
- decreased mobility
- ongoing discomfort
- fever
- Aching joints
Osteotomy using Pedicle Subtraction
Pedicle subtraction osteotomy (PSO) procedures are being carried out more often as a result of both our aging population and a clearer understanding of sagittal malalignment. Pseudarthrosis, which affects 10% of individuals, is one of the significant side effects. Risk factors for pseudarthrosis at the osteotomy level include preoperative radiation, performing the procedure to treat an existing pseudarthrosis, having a neurological or inflammatory disorder, and not having an interbody fusion directly above the osteotomy. Cadaveric research corroborates this final statement. Interbody cages appear to increase the stiffness of the structure, which appears to improve fusion rates. It is also for this reason that the authors decide to use side-to-side connections and a chrome-cobalt rod, a method similar to that reported by Hyun et al., to add a third rod to PSO constructions, from a level above to a level below the osteotomy site.
Surgery for Spinal Deformity
The risk of pseudoarthrosis was shown to be 24% in one analysis of deformity procedures involving the sacrum.20 All pseudoarthroses, which either formed at the thoracolumbar junction or the lumbosacral junction, were discovered before four years had passed since the surgery, on average 27 months later. For thoracolumbar pseudoarthrosis, the risk variables were thoracolumbar kyphosis and a thoracoabdominal approach, for lumbosacral pseudoarthrosis, osteoarthritis of the hips and a positive sagittal balance of 5 cm, and age > 55. Scoliosis Research Society (SRS) ratings for patients with pseudoarthrosis were lower than those with solid fusions, as one might predict (71 vs. 90/120).
PRESENTATION
There are three ways that pseudoarthrosis might manifest. The patient might have a pseudoarthrosis linked to another clinical condition, such as an infection, or they could be asymptomatic and functioning well.
Scores for Functional Outcomes
It is still unknown why so many people with pseudoarthrosis get positive functional results and don’t experience any symptoms. The results of patients with solids fusion vs pseudarthrosis were examined in a short research from 1968, and there were few differences. Since the fusion is described as either Hibbs- or “H”-type, it may be assumed that the authors were working with uninstrumented fusions. According to more recent research on uninstrumented fusions, only 56% of patients with pseudoarthrosis had satisfactory outcomes, compared to 86% of patients with solid fusions.
There is conflicting information about the relationship between a strong union and a successful result when examining trials of instrumented fusions. According to a study conducted by Resnick et al., “the majority of Class III medical evidence does suggest that successful radiographic fusion is associated with improved clinical outcomes.” Despite being randomized, several of these trials were nonetheless categorized as Class III due to significant crossover rates.
All patients with a verified pseudoarthrosis at one year or longer failed to improve their SRS or Oswestry Disability Index (ODI) scores in an investigation of consecutive deformity patients at one institution. In fact, the absence of progress in these scores was more reliable than conventional X-rays at identifying pseudoarthrosis. This was also mentioned in the earlier scoliosis research. The authors draw the following conclusion as a result of this finding: functional outcome scoring is crucial for postoperative deformity patient monitoring and should act as a catalyst for more pseudarthrosis research.
Types of Pseudarthrosis
1. Asymptomatic Pseudarthrosis
The discovery of pseudoarthrosis in an asymptomatic patient typically results from the surgeon’s observation and raises an intriguing question. Is there any benefit to subjecting a patient with pseudarthrosis who is otherwise asymptomatic and in good health to radiation in order to detect an aberration that is most likely not going to require surgical intervention? When will the surgeon’s treatment of an asymptomatic patient alter as a result of the discovery of pseudoarthrosis? After any multilevel operation or osteotomy, it would be logical to assume that early identification and treatment of an asymptomatic pseudoarthrosis may prevent serious problems in the future, making monitoring prudent. Standard scoring systems are a reliable and efficient way to do this. Radiological screening may be less crucial after a single-level treatment because it is unlikely that there would be any serious complications down the road, even if it does not unite.
2. Symptomatic Pseudarthrosis
Pseudarthrosis that is symptomatic typically manifests as worsening axial back pain. The pain may be a fresh beginning or a worsening of the initial discomfort from the procedure (“never got better”). Although it is uncommon, persons with scoliosis may complain of their deformity getting worse. Patients with ankylosing spondylitis could be sensitive to changes in their visual horizon. Unless there is a significant segmental malformation, neurological symptoms are uncommon.
3. Concomitant Pseudarthrosis
Infection is the most probable coexisting diagnosis. Strong indicators of infection include a history of fevers, an unanticipated return to the operating room, long-term antibiotic use, and a lesion that is discharging. The presentation could also be accompanied by weight loss and ill health. You should look for any further infection entry points.
Investigation
Investigating a suspected case of pseudoarthrosis should consider any concurrent or differential diseases that are plausible. Although first challenging to interpret, CRP and ESR should be checked, along with any other types of blood that might indicate an infection. Any swelling or accumulation of soft tissue in the incision should be examined and recorded. Any fluid collection should have a sample taken, which should then be sent for sensitivity testing, culture, and microscopy. The surgeon must be ready in case purulent fluid is found during revision since preoperative examinations sometimes miss low-grade infections.
- Imaging Studies
Statistical Analysis
An understanding of sensitivity, specificity, and kappa values must be included in any discussion of imaging studies—or any other diagnostic test, for that matter. These concepts, as well as how they might be applied to inform our decision-making, must be understood by any surgeon. The tests are seen as attempts to find a fusion for the sake of understanding the material that follows. Therefore, specificity relates to the likelihood of properly recognizing a pseudoarthrosis whereas sensitivity refers to the likelihood of correctly detecting a fusion.
Low sensitivity testing might “miss” a solid fusion and lead the surgeon to undergo extraneous treatments in an effort to correct an ostensible pseudoarthrosis that is solid. On the other hand, a test with limited specificity may “miss” a pseudoarthrosis and mislead the patient and surgeon about the necessity of the fusion.
A measure of the degree of agreement between observers, the kappa value, or Cohen’s kappa coefficient, ranges from 0 (no agreement, or agreement only by chance), to 1 (perfect agreement). Moderate agreement is defined as a number between 0.41 and 0.60, and considerable agreement is a value between 0.61 and 0.80. In the biomedical areas, values exceeding 0.81 are considered to be “almost perfect” agreements. A low kappa value should alert the surgeon that the result may be highly observer-dependent, even if a test has excellent sensitivity and specificity. Obtaining consensus through the presentation of the findings to several professionals may be a technique to get past the issue.
X-rays
Plain X-rays
The studies by Brodsky and Kant that examine plain radiographs are two of the best. Their outcomes were comparatively comparable. With a sensitivity of 85-89% but a poor specificity of 60-62%, the correlation between plain static X-rays and surgical exploration was 64-68%. In other words, if an X-ray shows a solid fusion, it is probably solid; yet, if it shows pseudarthrosis, it cannot be trusted. A mean of 3.5 years passes from surgery to the first X-ray showing a pseudoarthrosis.
Another problem is the wide range of X-ray interpretation between and within observers. In one investigation, where X-rays were evaluated by two radiologists and two surgeons, the correlation was weak ( = 0.4–0.7). Because of this, the authors do not suggest plain X-rays for the evaluation of solid fusion despite their availability and relative affordability.
Bending or Dynamic X-rays
When examining pseudarthrosis, bending or dynamic films—also known as flexion-extension studies—perform similarly to standard X-rays. Although the absence of motion in these experiments is associated strongly with solid fusion, according to the same research by Brodsky et al., movement does not always denote pseudoarthrosis.
Computed Tomography (CT)
CT scanning was only shown to have a sensitivity of 63%, specificity of 86%, positive predictive value of 72%, and negative predictive value of 81% in the research by Brodsky et al. that was previously mentioned. However, it is important to bear in mind that this study and many others like it were carried out in the late 1980s. Consequently, these results were not significantly different from conventional X-rays. Therefore, it should not be surprising that more recent investigations, using more recent helical multi-slice scanners, have shown substantially superior findings. Sadly, not many people have contrasted imaging with the surgical investigation.
Roentgen Stereophotogrammetric Analysis (RSA)
Tantalum markers are inserted during surgery using the RSA method into the bony vertebrae. Following surgery, the beads are imaged consistently so that movement may be precisely recorded. Similar to dynamic X-rays, this method has the drawback that motion—or a lack thereof—does not always indicate pseudarthrosis. For instance, in accordance with RSA, there could not be any mobility across a segment right away following surgery, even if plainly no fusion has yet developed. It is solely utilized for study, and considerable consideration should be given to the clinical connection to fusion.
Nuclear Medicine
To evaluate the activity of the bone surrounding a fusion mass, technetium-99m bone scanning is frequently employed. The “cold” scan is supposed to correlate to fusion. Although it was more specific (93%) than surgical exploration, it lacked sensitivity (50%) and had a lower positive predictive value (40%) for pseudarthrosis. When examining individuals with scoliosis, similar findings were made. The technique’s inability to distinguish between mature fusion masses and established pseudarthrosis is regarded as the main issue.
Ultrasound
One modest study that compared the appearance of the posterior structures to surgical exploration examined the use of ultrasonography. Although it seemed promising, its capacity to evaluate the anterior fusion mass is constrained. No more research has been done.
Classification Of Fusion
Posterolateral Fusion
The first classification of physically distinct kinds of pseudoarthrosis of posterolateral fusions was made by Heggeness and Esses They also discussed the “shingle sign,” which is a bone fragment that seems to be floating beyond the posterior components on an axial CT slice and is frequently found in the shingle type of pseudoarthrosis. This categorization is advantageous since it hints at the origin of pseudoarthrosis. Two further current research compared the results of CT scans to the surgical investigation. Three spine surgeons were asked to evaluate 1 mm axial slice CT images recorded on film for Carreon et al.’s 2007 paper28. It’s interesting to note that they recorded both fusions in the posterolateral gutters and fusion across the facet joint. When fusion was seen in all facets and both posterolateral gutters, there was a 96% likelihood that the fusion would be strong upon examination. The likelihood of finding a solid fusion at exploration decreased to 74% if it was only observed in the posterolateral gutters and to 89% if it was only observed across the facet joints.
Interbody Fusion
Through their carbon fiber cage, Brantigan and Steffee initially proposed a categorization of interbody fusion. It is frequently referred to as the BSF (Brantigan, Steffee, Fraser) classification since Fraser updated it later. When a pseudoarthrosis is detected by a CT scan, it is categorized as BSF-1 or BSF-2, depending on whether there is obvious evidence of movement. The latter is typically referred to as a “locked pseudarthrosis”. Even if the second PLIF cage had lucency across it, they considered the fusion solid if bone could be seen growing through one of the cages.
- Anterior Lumbar Interbody Fusions (ALIF)
Similar procedures were applied in Carreon et al.’s second publication, which examined anterior lumbar interbody fusions utilizing iron cages. Despite the significant interobserver variation, the CT scan demonstrated a 93% sensitivity and a 46% specificity for fusion when agreement was reached. In contrast to the posterior sentinel sign, which had a higher sensitivity and specificity of 67% and 79%, the anterior sentinel sign (30) had just 20% sensitivity and 92% specificity for identifying a fusion. Pseudarthrosis can be diagnosed by looking for the lack of an anterior sentinel sign.
- Posterior/Transforaminal Lumbar Interbody Fusions (PLIF/TLIF)
Evaluation of interbody fusion is frequently difficult. Tantalum markers enclosed in PEEK or carbon fiber cages can frequently leave a significant artifact that might interfere with CT imaging, especially when carried out on outdated equipment. The work has become considerably simpler because of modern multi-slice helical machines and powerful artifact removal techniques, and coronal plane reconstructions are good at showing the interbody fusion mass.
Conclusion
When an iliac crest graft is available, it should always come from this source because there is no synthetic alternative for it in the treatment of pseudoarthrosis. While rhBMP-2 has been demonstrated in two significant systematic studies to be comparable to autologous bone grafts, it is not without expense or problems. Biologically inert “fillers” like these should be avoided when a surgeon is treating pseudoarthrosis since allografts and ceramics like tricalcium phosphate lack osteoinductive characteristics.
Any fusion patient who does not behave as normal should alert the surgeon to the risk that pseudoarthrosis is taking hold. When a surgeon “blames” a patient, they are not doing their patient or themselves any favors. X-rays and CT scans are relevant examinations, and it’s important to keep track of any slight changes over time.
Once the diagnosis has been made, a detailed and honest conversation discussing the advantages and disadvantages of surgical intervention should take place because this choice is not always obvious. The surgeon must consider the mode of failure and the measures required to accomplish fusion in a suitable alignment after surgical intervention is chosen. Unfortunately, one cannot anticipate a regular surgical and postoperative course, and one must warn patients that they may never have the desired outcome from their initial procedure.
Pearls and Pitfalls
Plan and get ready to do surgery that will reduce hazards for individuals who have a high risk of developing pseudoarthrosis. Instrumentation and 360° fusions by two different techniques or with interbody and bilateral posterolateral grafts both increase the fusion rate.
If a patient’s functional outcome scores do not rise as anticipated, you should be concerned that they are developing pseudoarthrosis.
The research of choice to identify a pseudoarthrosis, and in particular, a “locked pseudoarthrosis,” is a reconstruction of a coronal plane CT scan.
However, lucency around an interbody cage is likely to be the first sign of an eventual pseudoarthrosis. Loosening around screws should resolve with time and should be closely monitored.
The preferred grafting substance should be an autologous bone transplant.
Treatment of Pseudarthrosis of the Spine
Treatment options for pseudarthrosis of the spine depend on various factors, including the location and severity of the condition. Non-surgical approaches may include bracing or immobilization to restrict movement and promote healing. Physical therapy and other conservative measures can be used to strengthen the surrounding muscles and support the spine. In cases where non-surgical methods fail, revision surgery may be necessary. The surgeon may use additional bone grafts, implants, or different techniques to promote successful fusion.
A second attempt at fusion is necessary for the patient with symptomatic pseudoarthrosis to receive treatment. Recent surgical innovations have reduced the incidence of pseudoarthrosis following spine fusion surgery, including the use of spinal instrumentation, bone graft alternatives, and genetic engineering (bone morphogenetic protein).
Most frequently, surgery is used to treat pseudoarthrosis. Surgery focuses on trying to mend the bone again when bone fusion procedures have already failed.
When pseudoarthrosis affects the spine, surgeons can:
- Interbody fusion, which entails removing the spongy disc between the vertebrae, is the process of replacing loosened implants or devices with stronger tissue substitutes.
- Congenital pseudoarthrosis of the clavicle should also be treated surgically, according to the authors of a 2021 study. This entails resecting the clavicle while employing a bone transplant from the pelvic iliac crest.
Treatment for congenital pseudarthrosis of the tibia might be difficult. According to a study from 2021, just 50% of surgical operations for the illness led to healing without refracturing on average.
But using a surgical procedure called deliberate cross-union between the tibia and fibula, the success rate was enhanced to 100% recovery without refracture.
Another potential therapeutic option is electrical stimulation therapy. Electrical stimulation devices may considerably accelerate the rate of bone fusion in patients having spinal fusion, according to a study from 2020.
Physical therapy, anti-inflammatory drugs, injections, and/or radiofrequency ablation are examples of non-surgical therapies.
Surgical Strategies
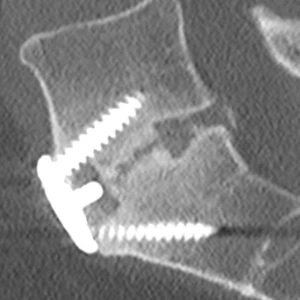
A balance between risks and benefits must always be used to decide whether to perform surgical intervention. Although a patient with a lengthy fusion, even if asymptomatic, may need investigation to prevent making future surgery significantly more challenging, an asymptomatic patient with a single-level pseudoarthrosis may not need intervention. It should be highlighted that even after a successful fusion, patients who had pseudarthrosis performed worse than those who did after their original surgery and a successful fusion.
Approach
Similar to the procedures used to achieve a fusion in the first place, there are numerous different surgical options for treating pseudoarthrosis. Improved stability, fresh grafting, and restoring sagittal alignment are the main guidelines to be followed. It is obvious that loose and damaged equipment has to be replaced in order to enhance stability. Pedicle screws can frequently have their diameter “upsized” by a millimeter or two to have a good hold in a previously loose screw trajectory. It is also occasionally feasible to lengthen screws, although this requires thorough preoperative planning. One should think about extending the fixation to a neighboring segment, particularly if it is connected to adjacent segment disease, but one must remember that the newly integrated levels also need to accomplish fusion. Practically speaking, stability is frequently greatly improved by extending fixation to the ilium after a failed lumbosacral fusion.
An unsuccessful posterolateral fusion can be stabilized better and given an interbody graft to increase graft material under compression. Anterior column support is increased by swapping out a “soft” disc space for a mixture of a comparatively stronger cage and graft. This can be done using either an anterior or lateral approach, depending on the level. It is also possible to utilize a TLIF or PLIF approach, although this will almost certainly encounter scar tissue and raise the possibility of nerve damage and dural tears.
Sagittal Balance
Sagittal balance must constantly be assessed and recorded. If the patient’s alignment is not corrected, they will still have a bad prognosis with a solid fusion for their pseudoarthrosis. The surgeon must again maximize the possibility of fusion by producing adequate bone apposition, stiff and strong structures, and reducing the patient’s own risk factors. An osteotomy via pseudarthrosis may be required to accomplish the correction.
Stimulation
Both pulsed electromagnetic field stimulation and the use of DC current stimulators have been supported by certain research Unfortunately, neither approach has consistently produced positive results and has generally lost favor with the public.
Bone Graft
When an iliac crest graft is available, it should always come from this source because there is no synthetic alternative for it in the treatment of pseudoarthrosis. While rhBMP-2 has been demonstrated in two significant systematic studies to be comparable to autologous bone grafts, it is not without expense or problems. Biologically inert “fillers” like these should be avoided when a surgeon is treating pseudoarthrosis since allografts and ceramics like tricalcium phosphate lack osteoinductive characteristics.
Spinal Fusion
A fusion is a surgical procedure that involves “welding” the vertebral bones together to stop mobility between them. The bones recover into a single, solid piece by joining together. To stop unpleasant movements, correct your alignment or posture, or give stability to your spine, a fusion treatment may be advised. If you experience leg symptoms like pain and numbness, your surgeon could choose to conduct a laminectomy in addition to the fusion treatment in some circumstances. Our objective is to determine which degenerative disc is responsible for your continuous discomfort. One method to treat your symptoms is fusion surgery.
Types of Minimally Invasive Spinal Fusion Surgery
- Anterior Cervical Corpectomy
By removing one or more vertebral bodies, a corpectomy is a successful operation for relieving pressure on the spinal cord. A tiny incision is made on the front of the neck, typically in the natural crease, to perform an anterior cervical corpectomy.
- Anterior Cervical Discectomy & Fusion (ACDF)
To alleviate neck and nerve issues, an anterior cervical discectomy and fusion procedure may be used. The process of spinal fusion is performed to fix the vertebrae or spinal bones. A cervical fusion aims to build a strong bone bridge connecting two or more vertebrae. When the spine is unstable or the natural disc space has shrunk, spinal fusion may be advised. A tiny incision is made on the front of the neck, generally in the natural crease, to conduct an anterior cervical discectomy and fusion.
- Anterior Lumbar Interbody Fusion (ALIF)
A novel method to remove lumbar spine degenerative discs is anterior lumbar interbody fusion. The treatment, which uses a minimally invasive technique, is performed from the front of the spine and builds a sturdy bridge between at least two vertebrae. This surgical procedure aims to relieve discomfort, numbness, or tingling brought on by a lumbar disc that is beginning to degenerate.
- Hybrid Cervical Spine Surgery
A cutting-edge method called hybrid cervical spine surgery combines the mobility provided by a synthetic disc replacement with the stability of a typical spinal fusion. It was developed to eliminate the discomfort and tingling/numbness brought on by disc disease. The Virginia Spine Institute’s spinal surgeons were the first in the country to conduct this procedure.
- Lateral Interbody Fusion
The surgeon will divide the tissue fibers using a minimally invasive technique to reach the side of the spine. This is a fantastic method because it realigns the spine and releases pressure on the nerves without causing extensive damage to the soft tissues in the rear of the spine by making a larger incision.
Direct lateral interbody fusion (DLIF) and extreme lateral interbody fusion (XLIF) are two abbreviations for the same surgical procedure.
- Posterior Instrumented Fusion (PIF)
A posterior instrumented fusion includes the placement of screws and rods. With this operation, cutting-edge technology can be used, giving your surgeon the ability to see where the hardware will be placed. Less soft tissue cutting and improved screw insertion accuracy are also benefits of this.
- Posterior Lumbar Interbody Fusion (PLIF)
A lumbar fusion procedure from the back is called posterior lumbar interbody fusion (PLIF). To make a window to access the spinal canal, bone is removed. This opens up a place where disc material can be removed in order to make room for implants that will fuse the bones together. Screws and rods stabilize this fusion process.
- Sacroiliac Joint Fusion
The sacrum and pelvis are joined by the sacroiliac joint, sometimes known as the “SI joint,” which is a sturdy, weight-bearing joint in the lower back. Although there is a slight degree of flexibility, the SI joint should typically fit together like a lock and key.
While physical therapy, medications, and injections into the SI joint are frequently used to treat sacroiliac joint problems, a sacroiliac joint fusion may be suggested in order to stabilize the joints if the pain continues.
- Transforaminal Lumbar Interbody Fusion (TLIF)
The process of spinal fusion is performed to fix the vertebrae or spinal bones. In lumbar fusion, a strong bone bridge is built between two or more vertebrae. When the spine is unstable or the natural disc space has shrunk, spinal fusion may be advised. An efficient way to achieve fusion is by interbody fusion, which includes inserting fusion implants and bone grafts into the space between two vertebral bodies.
- Kyphosis Correction
Robot-guided spine surgery can be used to do minimally invasive kyphosis correction surgery. With the use of this innovative technology, our surgeons may design and arrange a patient’s operation according to their unique anatomy before entering the operating room.
Implanting screws and rods is part of the surgical procedure to rectify the spinal deformity and stabilize the spine. The spine will eventually unite into a single, solid component in a new, more typical posture. Correcting the deformity, halting the advancement of the curve, and halting the symptoms enhance the patient’s quality of life.
- Scoliosis Correction
Corrective procedures for scoliosis and deformities aid in realigning the spine in individuals with aberrant curvatures. To schedule a consultation, please call. You can better grasp your spine’s prognosis with the aid of our scoliosis specialists. For your best interests, we will work with you to design a non-operative management strategy or evaluate several surgical management options.
Benefits of Spinal Fusion
- Reduce aching motion
- Regain your posture or alignment.
- You should stabilize your spine.
Spine-Specialized Physical Therapy
Experts in Non-Operative Therapies & Spine Surgery Rehabilitation
Virginia Therapy & Fitness Center (VTFC), a division of Virginia Spine Institute, offers patients the best rehabilitation services for all kinds of orthopedic problems. This is accomplished using a distinctive and all-inclusive therapy methodology.
Types of Spine-Specialized Physical Therapy
- Manual Physical Therapy
The phrase “manual therapy” refers to the practice of physical therapists making diagnoses and treating patients using their hands. Treatments for manual therapy may include manual traction, joint mobilization, or massage. Our PTs are great because we have manual therapists with fellowship training.
- Aquatic Therapy
Aquatic treatment is frequently the initial phase of rehabilitation for people recovering from surgery or those with severe injuries. Strength, flexibility, and function may all be improved in the very weightless environment of the water, expediting the healing process. In our own facility, we are able to provide aquatic therapy using an aquatic treadmill.
- Massage Therapy
The deliberate and methodical manipulation of the skin, muscles, ligaments, and tendons of the body is known as therapeutic massage. In order to improve function, promote healing, and improve health, a variety of massage techniques are utilized to target the body’s soft tissues and muscular system. Swedish massage, neuromuscular therapy massage, cupping treatment, and deep tissue massage are some of the modalities that are most frequently employed by patients with muscle discomfort.
- Concussion Therapy
Our nationally recognized concussion rehabilitation and therapy program is run by certified ImPACT-trained physical therapists (ITPT) who specialize in concussion care. To provide a holistic approach to concussion care, this group of topic specialists has developed concussion-focused rehabilitation procedures.
- Trigger Point Dry Needling
Our whole staff of physical therapists is trained in dry needling. Some even make cross-country trips to instruct dry-needling courses for other physical therapists.
- Laser Therapy
An effective, non-invasive approach called laser treatment delivers a therapeutic dosage of light to damaged or unhealthy tissue. For musculoskeletal problems, the class VI laser light induces a biological response that speeds up healing and reduces pain and inflammation. This safe alternative to medication and surgery has been approved by the FDA since 2003. It provides long-lasting pain relief. As a part of their care, our physical therapists can utilize this technology with their patients.
- Sports Training
Physical therapists that focus on dealing with athletes are available here. They have worked with athletes at all levels—high school, collegiate, amateur, and professional. For several sports, there exist specialist programs. To further an athlete’s conditioning and objectives, they also collaborate with a personal trainer or athletic trainer. Our facility has the capacity to build situations in which our athletes can practice.
- Personal Training
For people wishing to strengthen their bodies, correct their posture, and generally feel better, the Virginia Therapy & Fitness Center offers specialized, reasonably priced personal training. To ensure proper progression for people moving from physical therapy to the gym or for those who just need direction or accountability to get in better shape, our licensed personal trainers collaborate closely with our physical therapy staff as needed.
- Wellness & Nutrition Coaching
Our whole range of wellness services must include specialized dietary coaching. Through knowledge and coaching, nutrition coaching may assist you in making tiny lifestyle adjustments that will help you reach your weight loss, maintenance, or gain goals.
Benefits of Spine-Specialized Physical Therapy
- pain reduction
- higher blood flow
- an improved joint diet
- increased joint flexibility
Summary
Failure to effectively fuse two bones results in pseudoarthrosis. Following an injury or a bone fusion procedure, this may occur. It is a frequent side effect of such surgeries, especially those that fuse the bones in the spine.
Pseudarthrosis can manifest as a variety of symptoms, including discomfort when moving, lack of motion, and clicking noises. To treat it, surgeons could do further surgical operations.
FAQs
Failure of fusion following an index operation meant to achieve spinal arthrodesis is referred to as pseudoarthrosis.
Clinical significance for radiographic pseudoarthrosis may or may not exist. Some people require revision fusion surgery because they have discomfort at the location of a pseudoarthrosis.
When a damaged bone doesn’t mend properly after a fracture without intervention (surgery), it develops a disorder called pseudoarthrosis. The fracture is known as a false joint or pseudoarthrosis because it structurally mimics a fibrous joint.
The thoracolumbar junction was thought to be the site of the pseudoarthrosis. Pseudarthrosis was more likely to occur in individuals who were older (>55 years), had lengthier fusions (>12 vertebrae), and had thoracolumbar kyphosis (> or =20 degrees).
Once a fracture has occurred or a pseudoarthrosis has manifestly formed, the three most often utilized surgical procedures are intramedullary rod fixation, circular ring fixation, and vascularized fibular grafting.
Progressive bending, the resorption of a small bone fragment, and angulation at the location of resorbed bone are some radiological characteristics. Both a primary periosteal disease and a secondary bone disease are likely to be present.
An unhealed shattered bone is referred to as pseudoarthrosis or nonunion. Broken or injured bones often mend over time by growing new bone tissue to join the fractured fragments. ‘Nonunion’ or ‘pseudarthrosis’ is the medical term for when a broken bone does not mend.
On the other side, there might be certain drawbacks. A fusion requires substantial bone surgery, which might cause greater back discomfort and prolong the healing process. During a fusion, the lateral facet joints and transverse processes—two particular vertebral structures found on the sides of each vertebra—are frequently exposed.
Your back may probably feel tight and uncomfortable after surgery. For extended periods of time, you could find it difficult to stand or sit still. Getting back to minor tasks, including light housework, may take 4 to 6 weeks. Your back may need six months to a year to fully recover.
What pseudarthrosis signs and symptoms are there? Pseudoarthrosis symptoms overlap with those of osteoarthritis and include stiffness, ongoing pain, clicking in the joints, and in rare cases, redness and fever.
The screws and rods will inevitably get loose over time or potentially shatter if the bone doesn’t really knit together. Patients may then have either fresh back pain or repeated discomfort in their legs. The other significant category involves ongoing deterioration at a level close to a prior operation.
How Long Is a Spinal Fusion Effective? Since the outcomes of spinal fusion are irreversible, it is meant to endure a lifetime. several spinal fusion patients report reduced pain and increased mobility for several years following the procedure.



One Comment