Femoral Neuropathy
Table of Contents
Definition
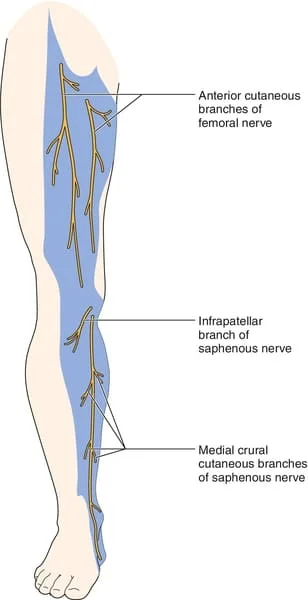
Femoral neuropathy, a condition affecting the femoral nerve, is characterized by dysfunction or damage to the nerve, resulting in a range of motor and sensory deficits. The femoral nerve is one of the major nerves in the lower extremities, originating from the lumbar spine and running through the thigh. It plays a crucial role in the movement and sensation of the leg muscles and skin.
Femoral neuropathy can arise from various causes, such as trauma, compression, inflammation, metabolic disorders, infections, or underlying medical conditions. The symptoms may include weakness or paralysis of the thigh muscles, decreased sensation in the front of the thigh and lower leg, as well as pain or discomfort in the hip or groin area.
Early diagnosis and appropriate management are essential to prevent further complications and promote optimal recovery. Treatment approaches may involve addressing the underlying cause, physical therapy, pain management, and, in some cases, surgical interventions. A thorough understanding of femoral neuropathy is crucial for healthcare professionals to accurately diagnose and manage this condition effectively.
Causes Of Femoral Neuropathy
Hip Surgery or Injury: Surgical procedures or injuries around the hip joint can damage the femoral nerve, leading to neuropathy.
Compression or Entrapment: Prolonged compression or entrapment of the femoral nerve due to tight clothing, belts, or certain positions can cause neuropathy.
Infections and Inflammatory Conditions: Infections like shingles (herpes zoster) or inflammatory conditions like Guillain-Barré syndrome can affect the femoral nerve.
Tumors or Growths: Tumors, cysts, or other growths in the pelvic region can put pressure on the femoral nerve, causing damage.
Vascular Issues: Reduced blood flow to the femoral nerve due to conditions like vasculitis or atherosclerosis can lead to neuropathy.
Radiation Therapy: Radiation treatment for cancer in the pelvic region can sometimes damage the femoral nerve.
Metabolic Disorders: Disorders like hypothyroidism or kidney disease can contribute to nerve damage, including in the femoral nerve.
Symptoms Of Femoral Neuropathy
Muscle Weakness: You might experience weakness in the muscles of the thigh and sometimes the lower leg, which could affect your ability to walk, climb stairs, or perform everyday activities.
Tingling or Pins and Needles Sensation: You might feel tingling, pins and needles, or a sensation of “electric shocks” in the thigh or leg.
Difficulty Extending the Leg: It could become challenging to fully extend the leg at the knee joint.
Difficulty Standing Up from a Chair: Rising from a seated position might become more difficult due to weakness and pain.
Pain in the Hip, Groin, or Lower Back: Pain can radiate from the thigh to the hip, groin, or lower back areas.
Numbness: There might be areas of reduced sensation or numbness in the front of the thigh or inner leg.
Inability to Straighten the Leg: You might have trouble fully straightening the leg at the knee joint.
Impaired Reflexes: Reduced or absent knee reflexes might be noticeable during a medical examination.
Remember, symptoms can vary from person to person and can also be caused by other conditions. If you’re experiencing any of these symptoms, it’s important to consult a medical professional for proper evaluation and diagnosis.
Diagnosis Of Femoral Neuropathy
Medical History: Your doctor will ask about your symptoms, their onset, duration, and any factors that might contribute to your condition, such as recent injuries, surgeries, or medical conditions like diabetes.
Physical Examination: During the exam, the doctor will assess your muscle strength, reflexes, and sensation in the affected leg. They might also look for any signs of muscle wasting or weakness.
Nerve Conduction Studies (NCS): NCS involves placing electrodes on the skin to stimulate the affected nerve and measure how quickly the nerve signals travel. Slowed or disrupted nerve signals can indicate nerve damage or compression.
Electromyography (EMG): EMG involves inserting a thin needle electrode into the muscles to assess their electrical activity. This can help determine if muscle weakness is due to nerve damage.
Imaging: An MRI (Magnetic Resonance Imaging) scan can provide detailed images of the affected area, helping to identify any structural issues or compression of the femoral nerve.
Blood Tests: Blood tests may be conducted to check for underlying conditions such as diabetes or inflammatory disorders that could contribute to nerve damage.
Diagnostic Blocks: In some cases, your doctor might use diagnostic nerve blocks to help pinpoint the source of pain. An anesthetic is injected near the nerve to temporarily numb it. If the pain diminishes after the injection, it can indicate that the nerve is the source of the problem.
Other Tests: Depending on the suspected cause, additional tests like X-rays or ultrasounds may be used to identify any specific issues that could be affecting the femoral nerve.
Keep in mind that only a qualified medical professional can diagnose femoral neuropathy accurately. If you’re experiencing symptoms or have concerns, it’s important to consult a doctor for a proper evaluation and diagnosis.
Differential Diagnosis of Femoral Neuropathy
Iliopsoas Hematoma: This occurs when blood accumulates in the iliopsoas muscle, often due to trauma or anticoagulant use, leading to pressure on the femoral nerve.
Iliacus Muscle Strain: Straining or injuring the iliacus muscle, which is close to the femoral nerve, could cause similar symptoms.
Inguinal Hernia: A hernia in the inguinal region can press on the femoral nerve, leading to symptoms resembling femoral neuropathy.
Nerve Entrapment: The femoral nerve can become entrapped or compressed as it passes through tight anatomical structures, like the inguinal ligament.
Pelvic Tumor or Mass: Tumors or growths in the pelvic region can apply pressure on the femoral nerve and cause neuropathy.
Nerve Compression from Pregnancy: Pressure on the femoral nerve due to the growing uterus during pregnancy can result in femoral neuropathy.
Infections: Infections like herpes zoster (shingles) or abscesses in the pelvic area can affect the nerve and lead to neuropathy symptoms.
Vasculitis: Inflammatory conditions affecting blood vessels can lead to nerve damage, including the femoral nerve.
Nerve Ischemia: Reduced blood flow to the nerve can cause ischemic damage and result in neuropathy.
Idiopathic Neuropathy: In some cases, the exact cause of femoral neuropathy may not be determined, leading to an idiopathic diagnosis.
Prevention Of Femoral Neuropathy
Stretching and Flexibility: Incorporate regular stretching exercises to improve flexibility and reduce muscle tightness that might contribute to nerve compression.
Proper Lifting Technique: When lifting heavy objects, use your legs and not your back to avoid strain on the lower spine and femoral nerve.
Avoid Prolonged Pressure: Avoid sitting or lying in positions that put prolonged pressure on the groin area. Change positions frequently and take breaks if needed.
Avoid Crossing Legs: Crossing your legs for extended periods can exert pressure on the femoral nerve. Try to sit with your legs uncrossed whenever possible.
Balanced Diet: A healthy diet can help maintain weight and manage conditions like diabetes that can contribute to nerve damage.
Stay Hydrated: Proper hydration supports overall nerve health and can help prevent nerve compression due to muscle cramps or spasms.
Regular Check-ups: If you have underlying health conditions like diabetes or vascular issues, regular check-ups and following medical advice can help prevent complications that might affect the femoral nerve.
Proper Footwear: Wear shoes that provide proper support and cushioning to prevent gait abnormalities that might lead to nerve compression.
Avoid Tight Clothing: Tight clothing around the waist and thigh area can compress nerves. Opt for loose-fitting clothing whenever possible.
Manage Chronic Conditions: If you have existing conditions like obesity, diabetes, or peripheral artery disease, proper management and treatment can help prevent nerve damage.
Risk Factors in Femoral Neuropathy
Injury or Trauma: Direct injuries to the thigh or pelvic area, such as from accidents or falls, can damage the femoral nerve and increase the risk of neuropathy.
Surgery: Surgical procedures around the pelvic region or lower abdomen, such as hip replacement surgery, hernia repair, or certain gynecological surgeries, can potentially damage the femoral nerve and lead to neuropathy.
Compression: Prolonged pressure on the femoral nerve due to factors like tight clothing, belts, or even prolonged sitting in a certain position can contribute to nerve compression and the development of neuropathy.
Obesity: Excess weight can increase pressure on nerves, including the femoral nerve, and raise the risk of neuropathy.
Diabetes: Diabetes can lead to nerve damage (neuropathy) throughout the body, including the femoral nerve. Elevated blood sugar levels over time can contribute to nerve dysfunction.
Inflammation: Inflammatory conditions such as autoimmune disorders or infections can affect nerves, potentially leading to neuropathy.
Radiation Therapy: Radiation treatment for cancer in the pelvic area can sometimes damage nerves, including the femoral nerve.
Peripheral Arterial Disease: Reduced blood flow to the legs due to peripheral arterial disease can affect nerve health and contribute to neuropathy.
Alcohol Abuse: Chronic excessive alcohol consumption can damage nerves, potentially increasing the risk of femoral neuropathy.
Medical Treatment of Femoral Neuropathy
Underlying Condition Management: Treating the underlying cause of femoral neuropathy is crucial. This might involve addressing issues such as diabetes, herniated discs, or infections. Managing these conditions can help alleviate nerve compression or damage causing neuropathy.
Pain Management: Pain relief is often a key aspect of treatment for patients. Over-the-counter pain medications or prescribed pain relievers could assess and manage discomfort. Sometimes, medications like gabapentin or pregabalin might be prescribed for neuropathic pain.
Physical Therapy: Physical therapy can be beneficial to improve muscle strength, flexibility, and posture. A physical therapist can design exercises and stretches that target the affected area to help alleviate symptoms and prevent further issues.
Corticosteroid Injections: In some cases, corticosteroid injections may be used to reduce inflammation and pain around the affected nerve.
Surgery: Surgery might be considered if conservative treatments aren’t effective. Surgical options depend on the underlying cause. For instance, if there’s a herniated disc causing compression, a surgical procedure to remove or repair the disc might be performed.
Assistive Devices: If weakness or mobility issues are present, assistive devices like braces, canes, or walkers might be recommended to help with stability and movement.
Lifestyle Modifications: Making healthy lifestyle changes can contribute to overall nerve health. Maintaining a balanced diet, managing weight, exercising regularly, and avoiding habits like smoking can support nerve recovery.
Physiotherapy Treatment Of Femoral Neuropathy
Pain Management: Over-the-counter pain-in-the-body relievers or prescribed medications could assess and manage pain and discomfort.
Bracing or Splinting: Depending on the severity of the condition, a brace or splint might be recommended to support the affected leg and reduce strain on the nerves.
Electrotherapy: Techniques like transcutaneous electrical nerve stimulation (TENS) could be used to provide pain relief and promote nerve function.
Heat and Cold Therapy: Applying heat or cold packs can help reduce pain and inflammation in the affected area.
Gait Training: Working with a physiotherapist to improve your walking pattern and balance can be beneficial.
Functional Exercises: Engaging in activities that mimic your daily tasks can help regain functional mobility.
Nerve Gliding Exercises: These exercises involve gently moving the affected limb in specific ways to promote healthy nerve movement.
Acupuncture or Massage: Some individuals find relief from neuropathic symptoms through complementary therapies like acupuncture or massage.
Lifestyle Modifications: Making changes in your daily activities, such as avoiding prolonged sitting or using ergonomic supports, can help reduce nerve compression.
Exercise for Femoral Neuropathy
- Hip Flexor Stretch: Kneel on one knee and extend the other leg forward, keeping your back straight. Gently lean forward to feel the stretch in front of your pelvis. Hold for twenty to thirty seconds and repeat on each side.
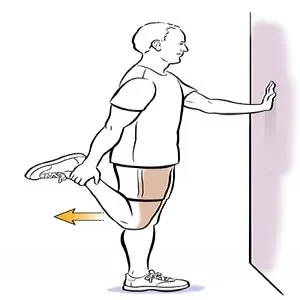
- Quadriceps Stretch: Standing, bend one leg at the knee and grab the ankle behind you. Gently pull the ankle toward the buttock to stretch the front of the thigh. Hold for twenty to thirty seconds and change legs.
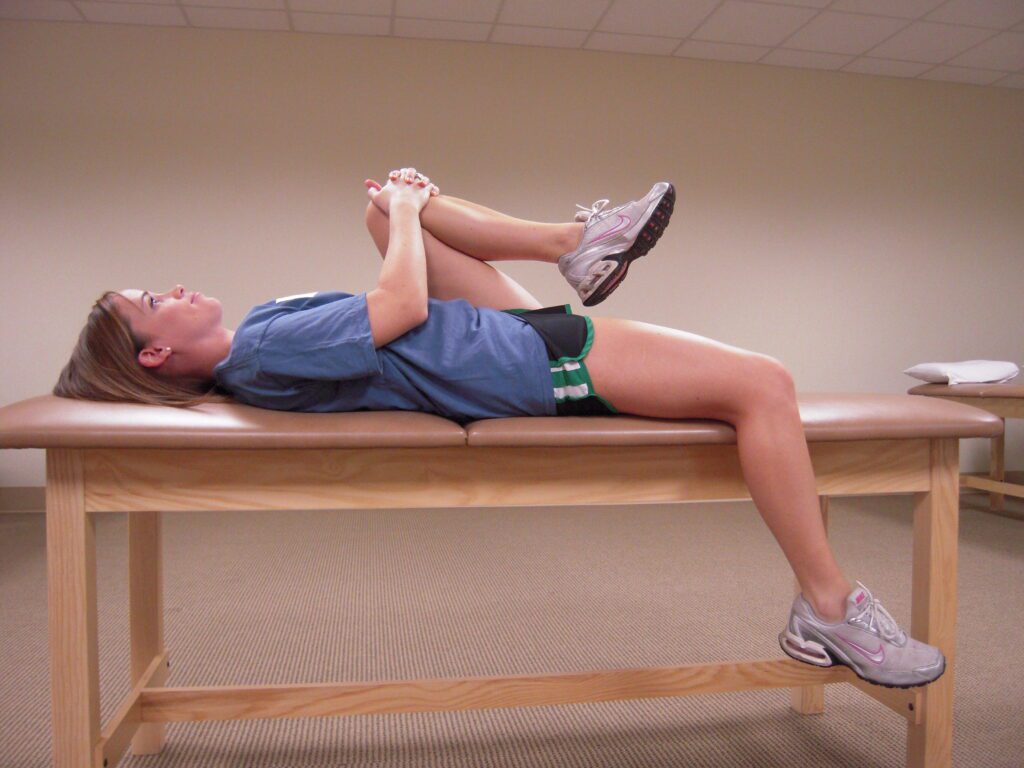
- Hamstring stretch: Sit on the floor with one leg extended and the other bent so that the sole is against the inner thigh of the extended leg. Reach forward toward your toes to feel the stretch in the back of your thigh. Hold for ten to twenty seconds and do in both legs.

- Inner Thigh Stretch: Sit on the floor and bring the soles of your feet together so that your knees bend outward. Gently press your knees to the floor to feel the stretch in your inner thighs.

- Lift Legs: Lying on your back, slowly lift one leg a few inches off the ground, keeping the knee straight. Hold for 3 to 5 seconds and then lower it back downside. Repeat with the other leg.

- Straight Leg Raise: Lie on your back, lift one leg a few inches off the ground, keeping the knee straight. Hold for 5 to 10 seconds and then lower it back downside. Repeat with the other leg.

- Cycling: If approved by your healthcare provider, gentle cycling while standing on a bike can improve circulation and strengthen leg muscles.

Surgical Treatment For Femoral Neuropathy
Nerve Decompression: This involves relieving pressure on the femoral nerve by removing any structures, scar tissue, or other factors that might be compressing it.
Tumor Removal: If a tumor or growth is compressing the femoral nerve, surgical removal might be necessary.
Nerve Transposition: In cases where the nerve is trapped or compressed by nearby structures, surgeons might reposition the nerve to relieve the pressure.
Neurolysis: This procedure involves removing scar tissue or other obstructions that might be impeding the normal function of the nerve.
Nerve Grafting: In severe cases of nerve damage, a nerve graft might be used to bridge the gap between healthy nerve segments and restore continuity.
Lysis of Adhesions: This procedure involves breaking down adhesions or scar tissue that might be causing nerve entrapment.
Summary
Femoral neuropathy is a condition involving damage to the femoral nerve, a significant nerve in the leg. This can result in motor and sensory impairments. The femoral nerve originates in the spine and runs through the thigh, playing a vital role in leg muscle movement and sensation.
Causes include trauma, compression, inflammation, metabolic disorders, and infections. Symptoms encompass muscle weakness, reduced sensation, and pain in the hip or groin.
Early diagnosis and proper management are key, with treatments ranging from addressing underlying causes to physical therapy and surgery. Healthcare professionals require a solid grasp of femoral neuropathy for accurate diagnosis and effective treatment.
FAQ
What is femoral neuropathy?
Femoral neuropathy is a condition that involves damage or compression of the femoral nerve, leading to weakness, numbness, or pain in the thigh and leg.
What are the common causes of femoral neuropathy?
Common causes include diabetes, trauma, pressure on the nerve due to prolonged sitting, hip surgery, and certain medical conditions.
What are the symptoms of femoral neuropathy?
Symptoms often include pain, numbness, or weakness in the front of the thigh, as well as difficulty walking or standing up from a seated position.
How is femoral neuropathy diagnosed?
Diagnosis typically involves a physical examination, medical history review, nerve conduction studies, and possibly imaging tests like MRI or CT scans
What is the treatment for femoral neuropathy?
Treatment depends on the underlying cause. It might involve managing the underlying condition, physical therapy, pain management, and sometimes surgery.
Can femoral neuropathy be prevented?
In some cases, avoiding excessive pressure on the thighs, maintaining a healthy weight, and managing conditions like diabetes can help reduce the risk.
Is femoral neuropathy reversible?
The outcome depends on the cause and severity of the nerve damage. With appropriate treatment and management, some cases can improve over time.
What complications can arise from femoral neuropathy?
Complications might include muscle weakness, difficulty walking, loss of sensation, and reduced quality of life if the condition is left untreated.
When should I see a doctor if I suspect femoral neuropathy?
If you experience persistent thigh pain, numbness, or weakness, especially if it’s interfering with your daily activities, it’s advisable to consult a healthcare professional.
Can physical therapy help with femoral neuropathy?
Yes, physical therapy can play a crucial role in improving muscle strength, mobility, and managing pain associated with femoral neuropathy.