Lumbar Strain
Table of Contents
What is a Lumbar Strain?
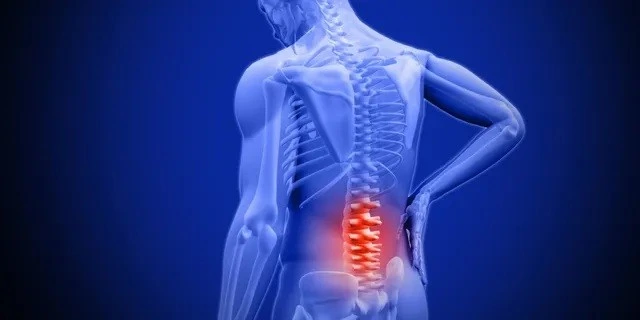
Lumbar strain, also known as lower back strain, refers to an injury or irritation of the muscles and tendons in the lower back. It is a common condition characterized by pain, stiffness, and limited range of motion in the lumbar region of the spine.
Lumbar strains typically occur due to overuse, poor body mechanics, lifting heavy objects, sudden movements, or repetitive activities that put excessive stress on the muscles and ligaments of the lower back.
What causes Lumbar Strain?
Injury can damage the muscles and tendons in the lower back. Pulling and Pushing sports, like weight lifting or football, can main to a lumbar strain. In addition, sports that need immediate twisting of the lower back, like tennis, basketball, baseball, and golf, can main to this injury.
Specific risk factors, like excessive lower back curvature, weak back, forward-tilted pelvis, or abdominal muscles, and tight hamstrings, can increase the risk of this injury.
What are the symptoms of Lumbar Strain?
The following are the very common symptoms of a lumbar strain. Still, each person might experience symptoms differently.
Symptoms might involve:
- Sudden lower back pain
- Spasms in the lower back that result in other severe pain
- Lower back feels sore to the touch
- Stiffness: The lower back may feel tight and restricted in movement.
- Stiffness: The lower back may feel tight and restricted in movement.
- Limited range of motion: It may be difficult to bend, twist, or perform certain movements without pain.
- Tenderness: The lower back may be sensitive to touch or pressure.
- Swelling: In some cases, there may be mild swelling in the affected area.
The symptoms of a lumbar strain might resemble more conditions and medical problems. Always talk with your medical management provider for a diagnosis.
How is lumbar strain diagnosed?
In the introduction to a full physical exam and medical history, the diagnostic process for low back pain might include the following. Still, during various initial assessments and exams, specialized tests aren’t normally recommended.
- X-ray: A diagnostic test that makes a picture of internal tissues, bones, and organs onto film.
- Computed tomography scan (also called a CT scan): This is an imaging test that uses X-rays and a computer to make detailed images of the body. A Computed tomography scan (CT scan) shows complete of the bones, muscles, fat, and organs. A Computed tomography scan (CT scan) shows complete images of bones, fat, muscles, and organs.
- Magnetic resonance imaging (MRI): A diagnostic process that operates a combination of large magnets, radio frequencies, and a computer to make a complete picture of structures and organs inside the body.
- Radionuclide bone scan: A nuclear imaging technique that uses a very little amount of radioactive material, which is injected into the bloodstream to be detected by a scanner. This test shows blood flow to the bone and cell activity inside the bone.
- Electromyogram (EMG): A test to assess nerve and muscle function.
How is Lumbar Strain treated?
Definite treatment for a lumbar strain will be discussed with you by your medical management provider based on:
- Your age, overall health, and medical history
- The extent of the injury
- Your tolerance for special drugs, procedures, and therapies
- Expectations for the course of the injury
- Your opinion or preference
Treatment may include:
- Rest
- Ice packs or heat and compression are applied to the back,
- Exercises (to strengthen the abdominal muscles),
- Stretching and strengthening exercises for the lower back muscles as it heals.
- Education regarding the use and wearing of suitable protective equipment.
Medicines, like anti-inflammatories and spinal injections, might also be used to relieve pain and inflammation.
Medical Treatment
Medical Management of mechanical back strains based on the patient’s conditions of symptoms, the patient’s comorbidities, and the particular cause.
First-line nonpharmacologic therapy:
- Acute low back pain involves spinal manipulation, acupuncture, massage, and superficial heat application, while first-line pharmacologic therapy for severe low back pain is nonsteroidal anti-inflammatory medications and muscle relaxants. According to the clinical policy by the American College of Emergency Physicians, opioids should not be day-to-day pharmaceutical therapy but saved for those whose pain is severe or uncontrolled with other medications.
- For chronic low back pain, non-pharmacologic approaches were recommended as the first-line agents, involving exercise, yoga, multidisciplinary rehabilitation, spinal manipulation, acupuncture, psychotherapy, low-level laser therapy, and electromyogram biofeedback. Nonsteroidal anti-inflammatory medicines were again the first-line pharmacologic agents suggested, followed by tramadol and duloxetine as the second-line treatments. Recommendations for opioid therapy are only if the before-mentioned therapies failed and depend on an individualized decision to determine if the benefit outweighs the risk.
Physical Therapy Treatment
Education: Interventions that might aid in injury prevention
- Stretching exercises at the workplace, proper rest breaks, and comfortable modifications. Ergonomic modifications refer to adaptations in the work environment to decrease the physical stress of the employees.
- Educating patients regarding the importance of maintaining correct posture and correct lifting techniques might aid in prevention. Regular physical activity
- Smoking cessation
- Weight loss for obese patients
- Resuming normal physical activity (recent studies have found that continuing ordinary activities within the limits permitted by the pain leads to another rapid recovery than bed rest).
Techniques
Cold Therapy: In the severe phase of a lumbar strain Cold therapy (Ice Pack) should be applied (for a short period of up to 48 h)to the affected parts to limit the localized tissue inflammation and edema.
TENS and Ultrasound: Transcutaneous electrical nerve stimulation (TENS) and ultrasound are often used to assist control of pain and decrease muscle spasms
Stretching: Mild stretching exercises with limited activity. Stretching Exercises below
- Double and Single knee to chest rests down on your back with your knees bent and your heels on the floor. Pull your knee or knees as close to your chest, and hold the pose for 8 to 10 seconds. Repeat this 3 to 5 times.
- Backstretch Lie on your back, hands above your head. Bend your knees and, holding your feet on the floor, rotate your knees to one side, slowly. Stay at one side for 10 to 15 seconds and repeat 4 to 5 times.
- Press up Begin by resting flat on the ground (face down). When doing this exercise it is important to hold the hips and legs relaxed and in touch with the floor. Clasp your hands in line with your shoulders. Inhale, then exhale and press up helping your hands hold the lower half of your body relaxed. Hold until you need to inhale, then move down, lay flat on the ground to rest, and repeat 8 to 10 times.
- Kneeling lunge(stretching iliopsoas)
- Stretching piriformis
- Stretching quadratus lumborum
Soft Tissue Manipulation: Soft tissue manipulation was found to reduce pain and improve Range Of Motion(ROM).
- Massage
- Strengthening Exercises: Progression of strengthening exercises should start once the pain and spasm are under control. The muscles needing the most emphasis are the abdominals, especially the obliques, the trunk extensors, and the gluteals. Placing all of the emphasis on rehabilitation especially on the injured muscle is not beneficial. Training core stability is an important area in the treatment of a lumbar strain and for the prevention of low back pain.
As with spinal injuries, posture, and body mechanics should be assessed and corrected as needed.
Prognosis
A Lumbar strain improves within 2 to 3 weeks. Normal functions are restored after 5 – 6 weeks.
When should I call my doctor?
Call your medical management provider if any of the following occur:
- You’re unable to stand or walk,
- You have a temperature over 101.0°F (38.3°C),
- You have frequent, painful, or bloody urination,
- You have severe abdominal pain,
- You have sharp, stabbing pain,
- Your pain is constant,
- You have numbness or pain in your leg,
- You feel pain in new parts of your back,
- You notice that the pain isn’t reducing after more than a week.
Contact your medical management provider immediately for the following:
- Pain radiating down the leg,
- Pain is followed by fever, weakness in the leg, or loss of control of the bladder or bowels.
Living with lumbar strain
Cold reduces swelling. Both cold and heat can reduce pain. Preserve your skin by placing a towel between your body and the ice or heat origin.
- For the first few days, apply an ice pack for 10 to 20 minutes,
- After the first few days, try to heat for 10 to 15 minutes at a time to ease the pain. Never sleep on a heating pad,
- Over-the-counter medicines can help control pain and swelling. Try aspirin or ibuprofen.
Exercise
Exercise can help your back heal. It also assists your back to get stronger and other flexible, preventing any reinjury. Ask your medical management provider about specific exercises for your back.
Use good posture to avoid reinjury
- When moving, bend at the hips and knees. Don’t bend at the twist or waist around.
- When lifting any weight or object, try to hold the object as close to your body. Don’t try to lift other than you can handle.
- When sitting, hold your lower back supported. Use a rolled-up towel as needed.
Key points
- Lumbar refers to your lower back,
- Strain can cause damage to the tendons and muscles causing pain and inflammation,
- Nonsurgical methods can rehabilitate most low back pain,
- Call your medical management provider if symptoms don’t get better within the next several days or if symptoms get worse.
Next steps
Tips to assist you get the most from a visit to your medical management provider:
- Know the aim for your visit and what you want to occur,
- Before your visit, write down some questions you have,
- Bring anyone with you to assist you ask questions and remember what your provider tells you,
- Write down the details of any new diagnoses, medications, treatments, or tests during the appointment. Also, write down any new requirements your provider gives you,
- Know why a new drug or treatment is prescribed, and how it will assist you. Know the adverse effects as well,
- Ask if your condition can be treated in more ways,
- Know why a test or process is recommended and what the outcomes could mean,
- Know what to expect if you do not take the drug or have the test or process,
- Note the date, time, and reason for any follow-up appointments you have,
- Learn how you can contact your provider if you have any questions.
Summary:
Lumbar strain, also known as lower back strain, is an injury or irritation of the muscles and tendons in the lower back. It is often caused by overuse, poor body mechanics, lifting heavy objects, or repetitive activities. Symptoms include lower back pain, muscle spasms, stiffness, limited range of motion, tenderness, and swelling. Treatment involves rest, pain management with medication, cold and heat therapy, physical therapy, practicing proper posture and body mechanics, and using supportive devices like back braces. Consulting a healthcare professional or physical therapist is important for an accurate diagnosis and personalized treatment plan.
FAQs
Various lower back strains occur during everyday activities, like while exercising or at work. Common causes of lumbar strain and risk factors for low back muscle strain involve Heavy lifting. Strain from heavy lifting, twisting the spine, lifting from the ground, or objects overhead are common causes of low back strain.
Sit with back support (like a rolled-up towel) at the curve of your back. hold your hips and knees at a right angle. Your legs should not be blocked and your feet should be flat on the floor.
More than 90% of cases totally recover from a lumbar muscle strain or sprain within 1 month. Hot and ice treatments are suggested on an as-required basis at home to treat immediate flare-ups of low back pain, along with anti-inflammatory drugs.
Self-care for back muscle strain
Apply cold and heat,
Try topical medication,
Massage your back,
Gently move your back muscles,
Support your lumbar curve,
Use a lumbar brace,
Walk as much as possible,
Try pool therapy.
First-line nonpharmacologic therapy: For Severe low back pain involves spinal manipulation, acupuncture, massage, and superficial heat application, while first-line pharmacologic therapy: for severe low back pain is nonsteroidal anti-inflammatory medicines and muscle relaxants.
Walking engages your core and lower back muscles, and strengthening weak muscles can assist alleviate low back pain from another sedentary lifestyle. Muscle weakness can also lead to fatigue and a greater risk of damage. Walking is a low-impact activity that can assist strengthen muscles throughout the body.
Lumbar Strain can cause injury to the tendons and muscles causing pain and soreness. The nonsurgical technique can cure most low back pain. Call your medical management provider if symptoms don’t get better over the next several days or if symptoms get worse.
Low-impact exercise, like walking, swimming, or simple stretching, promotes healing and increases blood flow. If you do not move the muscles all over your chin might weaken or stiffen, which increases low back pain.
The best-sleeping arrangement for lower back pain is on your side with an incomplete bend in the knees. Holding the knees bent assists balance the body and decreases pressure on the lumbar spine. Many more people notice it is supportive to put a small pillow between their knees to make this position more comfortable.
Anyone who strains a muscle in the lower back should rest to avoid more injury. Still, they should not stop moving altogether. Gentle movements that cause no pain can assist expedite the healing process.
Sitting for prolonged periods of time can be an important cause of back pain, cause improved stress on the back, neck, arms, and legs, and can add a tremendous amount of pressure to spinal discs and the back muscles.


One Comment