Gardner-diamond Syndrome
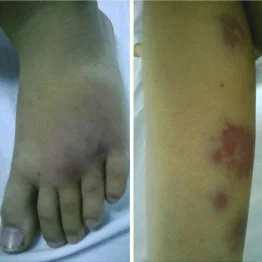
- Gardner-Diamond syndrome (GDS) is a condition characterized by episodes of unexplained, painful bruising that mostly occurs on the arms, legs, and/or face. It is most usual in Caucasian women who have a mental illness or emotional stress. Symptoms typically involve the formation of multiple, small, purple bruises that may be associated with burning, redness, and swelling.
- Most affected people report that the bruising happens either spontaneously, or sometimes after trauma or surgery at other sites of the body. The cause of Gardner-Diamond syndrome (GDS) is poorly understood. Management typically includes psychiatric treatment.
Table of Contents
When do symptoms of this disease begin?
- The most common age for symptoms of a disease to begin is known as the age of onset. The age of onset can vary for various diseases and may be used by a doctor to determine the diagnosis. For certain diseases, symptoms may begin in a single age range or several age ranges. For other diseases, symptoms may certain at any time during a person’s life.
Symptoms
- These symptoms may be varied from person to person. Certain people may have more symptoms than others and symptoms can range from mild to severe. This list does not involve every symptom.
This disease might cause these symptoms:
- Bruising susceptibility
- Ecchymosis
- Abnormality of limbs
- Behavioral abnormality
- Pain
- Superficial dermal perivascular inflammatory infiltrate
- Abnormality of the face
- Abnormality of the nervous system
- Anxiety
- Nausea
- Vomiting
- Gastrointestinal hemorrhage.
Body Systems
- Symptoms related to this disease may affect various parts of the body. The symptoms list shows one or more systems of the body commonly affected. Utilize the filter to view symptoms based on a specific body system.
Medical History and Physical Exam
- To begin the diagnostic process, a doctor or other health care provider (doctor) will take a medical history by asking questions about the patient’s current symptoms and diagnoses. They also usually ask about the past medical history, medications, allergies, the patient’s social history, and the family’s medical history. If available, the doctor may also review a patient’s medical records involving the results of previous tests and procedures.
During the physical exam, the doctor will study the patient’s body to see for physical signs of a medical problem. The methods used during the exam may differ depending on the symptoms but commonly include:
- Checking a person’s vital signs, involving temperature, heart rate, breathing rate, blood pressure, weight, and height.
- Looking at a person’s body to check for normal findings and any exchanges that may indicate a diagnosis.
- Touching parts of a person’s body to check for pain, tenderness, swelling, lumps, masses, or other changes.
- Listening to internal body sounds to detect the heart, lungs, or abdominal organs.
- Tapping on specific parts of the body to check for the presence of air, liquid, or solid structures.
- Evaluating the neurological system by detecting the reflexes, nerves, coordination, sensory function, and motor function, such as strength and balance.
- Depending on the results of the medical history and physical exam, the doctor may then decide whether lab tests, imaging studies, clinical procedures, or referrals to other medical specialists are required to diagnose the cause of the patient’s health problems.
Imaging Studies
- Tell to a doctor to learn if any imaging studies are suggested to diagnose or manage this disease.
- Diagnostic imaging studies let doctors see inside a patient’s body for clues to help diagnose or manage a disease. The type of imaging study a doctor chooses depends on a patient’s symptoms and the area of the body being examined.
Why are rare diseases hard to diagnose?
- A single symptom can be related to many various diseases.
- Doctors may not have experience with an infrequent disease.
How can the diagnostic journey be shortened?
- Find doctors who are easy to tell and understand.
- If possible, seek care at a big hospital or academic medical center.
Building a Medical Team
- Building a medical team can assist speed diagnosis and improving medical care. The primary care physician (PCP) is typically the center of the team. The involvement of other specialists depends on the type of symptoms or the requirement for special evaluations or treatments. The requirements for different specialists may change over time. Members of the medical team for this disease may involve:
primary care provider (PCP)
- A primary care provider (PCP) is a medical care provider (doctor) who is focused on the overall health of their patients. Primary care providers (PCPs) see patients for new or ongoing health problems. Primary care providers (PCPs) can provide referrals to specialists and can help manage and coordinate overall medical care.
- Types of Primary care providers (PCPs) include doctors practicing general medicine, family practice, pediatrics, internal medicine, and obstetrics/gynecology. A nurse practitioner (NP) or a physician assistant (PA) may be the primary care provider (PCP) in some practices.
Dermatologist
- A dermatologist is a doctor who has specialized training in diagnosing, treating, and managing diseases that harm the skin, hair, and nails.
Challenges
- Individuals who live with an infrequent disease can face challenges that can be overwhelming. It is normal for patients, their families, and caregivers to experience a variety of stresses that may exchange over time.
These challenges may involve:
- Limited information about the disease and treatment,
- Financial and economic difficulties,
- Adjustments to daily activities and roles,
- Social consequences and isolation,
- A wide range of feelings and emotions,
- Caregiving responsibilities.
Improving Quality of Life
- The medical team may not be aware of the multiple ways that an infrequent disease can change the quality of life of the patient and family.
- Children and adults who have a rare disease and their caregivers are encouraged to talk about their requirements with the medical team and to reach out for the support they need.
There are so many ways to collect support:
- The medical team can create a care plan and can create referrals,
- Family, friends, and religious leaders can allow support,
- Patient and caregiver organizations can assist connect to others,
- Infrequent disease organizations have informational resources,
- Organizations can allow disability and financial support,
- Disaster supports helplines can offer immediate assistance by phone.
FAQs
Psychogenic purpura, also known as Gardner-Diamond syndrome or autoerythrocyte sensitization syndrome, is a rare condition characterized by the spontaneous development of painful edematous skin lesions progressing to ecchymosis over the next 24 hours. Severe stress and emotional trauma always precede skin lesions.
Gardner-Diamond Syndrome is a rare yet potentially life-threatening disease. Oral surgery for Gardner-Diamond Syndrome can induce intraoral-facial skin lesions. Concomitant systemic manifestations may also arise.
Autoerythrocyte sensitization syndrome (AES) is a disorder characterized by reoccurrence, spontaneous, painful bruising in patients with underlying psychosis and neurosis. Its pathogenesis is uncertain. Purpuric lesions reproduced by injections of washed autologous erythrocytes propose an autoimmune etiology.
The average age at diagnosis is 25 (twenty-five) years; the average life expectancy for untreated patients is 45 years. The disease is characterized by different soft tissue tumors; colorectal adenomas; and multiple osteomas, particularly of the skull.
Gardner syndrome can be a life-limiting diagnosis in certain cases. Without treatment, nearly all people with the condition will develop colon cancer at a certain point. The average age for colon cancer diagnosis in people with Gardner syndrome is 39 (thirty-nine).
Although colonic polyps begin to form in puberty, the average age for Gardner syndrome diagnosis is 22 years. Osteoma formation precedes polyposis. Commonly, progression to malignancy is observed in patients aged 30-50 years. The average age by which malignancy is diagnosed is 39.2 years.
Genetic testing is the only way to definitively confirm the diagnosis of Gardner syndrome. The test detects mutations in the APC gene. Patients are referred for testing if they have a family history of the disease, or if a colonoscopy reveals more than 100 polyps in the colon & rectum.
Gardner’s syndrome treatment: Medications such as an NSAID (sulindac) or a COX2 inhibitor (celecoxib) may be used to assist limit the growth of colon polyps. Treatment also includes close monitoring of the polyps with lower GI tract endoscopy to make sure they do not become malignant (cancerous).
Disease at a Glance: Symptoms typically include the formation of multiple, small, purple bruises that may be associated with burning, redness, and swelling. Most affected people report that the bruising occurs either spontaneously, or sometimes after trauma or surgery at other sites of the body.
In Gardner syndrome, adenomas may be going to (noncancerous) or malignant (cancerous). However, the disorder significantly improves the risk of colorectal cancer and other cancers. While Gardner syndrome is a chronic disease, there are ways to manage the condition and decrease the risk of developing cancer.
Bruises hurt, yet most are not serious and will go away on their own within 2 to 4 weeks. Often, gravity causes them to spread down the body. A leg bruise commonly will take longer to heal than a bruise on the face or arms. Follow-up care is a key area of your treatment and safety.